Pearls from your Peers | Worst Case Scenarios: Managing OTO Emergencies in Practice
Katherine Kavanagh, MD discusses worst case scenarios with Johnathan D. McGinn, MD.

Worst Case Scenarios is an Academy course that provides experience with high acuity, low frequency clinical events. This is an opportunity to practice and learn in a simulated, but realistic no-risk environment, with your peers.
Who should participate in Worst Case Scenarios?
We envisioned this course as being directed toward practicing otolaryngologists and others working in otolaryngology practice, such as advanced practice providers. We have had some residents join as well, and the course is also appropriate for this level. We understand that advanced practice providers and practicing otolaryngologist may not have other facilities or access to engage in simulation education, so this course gives them that opportunity.
What should a participant expect from the course?
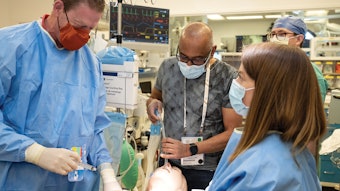
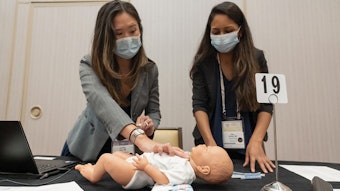
First and foremost, they need to expect to participate. Some people are fearful of simulation because they are afraid of being put on the spot. We do this in a team-based setting, so everyone has the opportunity to work as a team leader and also as a team member. The scenarios have a limited introductory explanation, and then you get right into the scenario where you have to manage a problem—it is a hands-on experience. You engage with the mannequins as you would a live patient. You are encouraged to engage with your team to develop and enact a plan for managing the situation. The scenarios help you develop a process of thinking on your feet and moving through what would be a stressful situation in real clinical settings.
What would you say to a participant who has never experienced simulation education?
I think you might like it more than you thought you would. Some participants may have some anxiety about the setting. It is very immersive—it is not unusual to feel your heart rate climb and your palms get a little sweaty as you try to save your patient. Although the patient is a mannequin, it feels fairly real. The key is that this is a team-based event; you are never alone, and you can always “phone a friend” who is standing right there. The goal is to do the best for that patient scenario. It is also a great opportunity to learn from your colleagues. We as otolaryngologists have the same basic training but different life experiences. In this course, you are working with adult learners who have real world experience. I have learned things from the students—I’ll think to myself, “I’ve never done that before, but it’s a great idea.”
What do you see as advantages to learning through simulation?
I think that everyone has their own personal best learning style. The immersive nature and the mechanics of thinking in the moment and doing something with your hands, which is what we do as surgeons, helps learner retention.
What have you found to be the most valuable aspects for the participants and facilitators?
The scenarios we have picked for this are things that are realistically situations one might experience in your day-to-day practice. You may not have experienced them with any frequency, but they are looming out there as possibilities. The opportunity to work through a case where there is no harm to patients, try new things, and learn from your colleagues is such a unique learning environment. There may be multiple ways to tackle the situation. For that low-frequency, high-stakes event that we don’t want to face but will, it is great to have a trial run before we encounter it in real clinical settings.















![03 Bites Better Hearing And Speech Graphic [converted]](https://img.ascendmedia.com/files/base/ascend/hh/image/2022/04/03_Bites_Better_Hearing_and_Speech_graphic__Converted_.6268225925563.png?auto=format%2Ccompress&fit=crop&h=191&q=70&w=340)


