FROM THE EDUCATION COMMITTEES | How to Diagnose and Manage the Patient with Olfactory Loss
Many budding physicians and surgeons who choose the field of otolaryngology do so based on our specialty’s ability to help patients regain their senses and help them interact more fully with the world around them.

Zara M. Patel, MD
Chair, Rhinology and Allergy Education Committee
Many budding physicians and surgeons who choose the field of otolaryngology do so based on our specialty’s ability to help patients regain their senses and help them interact more fully with the world around them. In otology, we help people hear again; in laryngology and head and neck surgery, we help people speak and swallow again; and in facial plastic surgery, we help patients regain lost facial function, smile again, and feel their most confident.
![Shutterstock 2020737482 [converted]](https://img.ascendmedia.com/files/base/ascend/hh/image/2022/04/shutterstock_2020737482__Converted_.6266f5284a80c.png?auto=format%2Ccompress&fit=max&q=70&w=400)
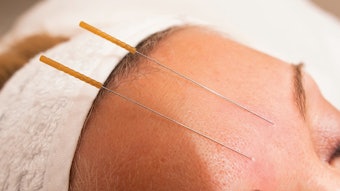
One silver lining of the COVID-19 pandemic has been the sudden interest in this sense, as hundreds of millions of people around the world fell prey to what would become one of the hallmarks of the early COVID-19 variants—a loss of smell and taste. Now with millions of those people suffering from long-term loss and dysfunction, general otolaryngologists and rhinologists will continue to be sought out for help in diagnosing and treating these symptoms at rates higher than ever before.
The quantity and quality of evidence in this field has a wide range, and desperate patients will look to anyone and anything they hear may help. It is our responsibility to educate them about the evidence we currently have and let them know there are options for treatment, while also protecting them from treatments lacking in evidence and could potentially be harmful.
Although COVID-19 may be a common cause of smell loss currently, there are dozens of different potential etiologies, ranging from the commonly known ones of post-viral, sinonasal inflammation, and post-traumatic, to neurodegenerative, metabolic, endocrinologic, environmental, and many more.
The first step in accurate diagnosis is a thorough history, including onset, timing, duration, quality, severity, or any inciting events. Specific questions to ask should be about history of sinonasal inflammatory disease, viral illness, trauma, toxin exposure, medications, anesthetic events, radiation, other cancer treatment, autoimmune disorders, endocrine disorders, vitamin/mineral deficiency, neurodegenerative disease or any cognitive changes, seizure activity, headache history, other neurologic disorder, changes in BMI, and smoking history.
The next step is to perform a validated, quantifiable smell test. There are many commercially available options from which to choose. And the next step is to perform a full head and neck exam, including cranial nerve examination and nasal endoscopy. If anything about the history leads you to suspect a specific underlying disorder, the physical exam should be widened and directed to other sites (for example, a full neurologic exam in someone suspected of developing Parkinson’s disease).
With regard to imaging, if the history/physical exam suggests sinus disease, a CT sinus is indicated. If history/physical exam suggests an underlying neoplasm, a CT or MR could be indicated. If the history/physical gives a specific underlying etiology not related to the sinuses or underlying neoplasm, no imaging is indicated. If the history/physical does not provide any specific etiology, an MR is an option to rule out any underlying intracranial pathology. An MR can also be used as a prognostic tool in patients with long-term loss or dysfunction.
For treatment, this should be tailored specifically to the underlying disorder and referral to the appropriate specialist. For example, for olfactory dysfunction related to chronic rhinosinusitis, we are the appropriate specialists, but for olfactory dysfunction related to an underlying kidney disorder, a nephrologist would be more appropriate. There are some treatment options that are globally applicable, such as olfactory training, and others that have only proven to help a particular type of smell loss, such as oral zinc for post-traumatic loss.
Depending on the etiology (see reference for details), topical steroid irrigations (but not sprays), topical vitamin A, and omega-3 may be helpful, as well as topical sodium citrate, but this one is only for short-term improvement. Physicians and other providers should not offer systemic vitamin A, minocycline, systemic phosphodiesterase inhibitors, such as theophylline, pentoxyphylline or caffeine, intranasal zinc, or oral zinc for non-trauma-related smell loss. There are many other proposed treatments that simply need more study and data before they can be recommended or recommended against as options in treating these patients.
Finally, due to the significant burden experienced by patients suffering from loss or dysfunction of smell, counseling should be provided regarding physical safety and psychological sequelae, or patients should be referred to someone who can.















![03 Bites Better Hearing And Speech Graphic [converted]](https://img.ascendmedia.com/files/base/ascend/hh/image/2022/04/03_Bites_Better_Hearing_and_Speech_graphic__Converted_.6268225925563.png?auto=format%2Ccompress&fit=crop&h=191&q=70&w=340)


