Acupuncture in Otolaryngology: A Primer
Acupuncture, a therapeutic modality of traditional Chinese medicine (TCM), has been used for centuries in Asian countries.
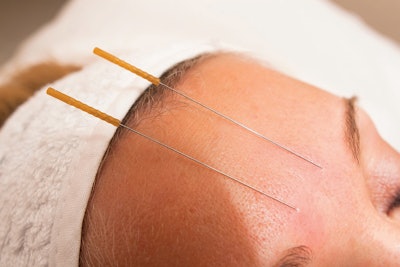
Acupuncture, a therapeutic modality of traditional Chinese medicine (TCM), has been used for centuries in Asian countries. It involves the placement of needles into specific points along the body.1 According to TCM theory, energy or vitality called “qi” flows throughout the body along channels or meridians. Disruption of this flow may lead to impaired function and disease. Acupuncture seeks to restore health and homeostasis through accessing specific points along targeted meridians. Additional core features of TCM are herbal medicine and tai chi.
There are many proposed mechanisms of action for acupuncture’s effects. When a needle is inserted into an acupoint, the feeling elicited is often described as a deep ache, soreness, heaviness, or even numbness. This is referred to as “de qi” in TCM. On a neuroanatomic basis, de qi is generated from the activation of various sensory receptors, small fiber-innervated nociceptors, and myelinated fiber-innervated mechanoreceptors.2 Acupuncture stimulation may create a steady stream of impulses transmitted to the substantia gelatinosa in the spinal cord, causing the gate for pain impulses to close.3
Within otolaryngology, acupuncture has been used for a variety of conditions from perioperative management to hyposmia and xerostomia. Since the 2013 U.S. Food and Drug Administration ban on codeine for post-tonsillectomy pain in children,4 there has been a renewed interest in effective nonopioid therapies. Acupuncture has been used in pediatric pain conditions ranging from headache to complex regional pain, cancer pain, and perioperative pain.5
One of the earliest U.S. reports to address this was from James W. Ochi, MD, in 2013. He retrospectively reviewed 31 cases of children who received acupuncture but not narcotics after tonsillectomy over a three-month period. He found the mean reported pain level before acupuncture was 5.52 (SD = 2.28) out of 10, falling to 1.92 (SD = 2.43) after acupuncture. Duration of effect varied, with 30% reporting pain relief > 60 hours and 30% < 3 hours.6
A group from Stanford performed a randomized, double-anonymized, placebo-controlled trial of intraoperative acupuncture for post-tonsillectomy pain. Through home surveys of patients, the group found significant improvements in pain control in the acupuncture treatment-group postoperatively (p = 0.0065 and 0.051, respectively), and oral intake improved significantly earlier in the acupuncture treatment group (p = 0.01). No adverse effects of acupuncture were reported.7
In 2018 a literature review of complementary and alternative medical treatment of post-tonsillectomy pain and nausea found the greatest amount of evidence for acupuncture and honey. Both were deemed cost-effective and safe.8 As patients, parents, and providers seek nonopioid alternatives, acupuncture may play a useful adjunct role.
A survey of nearly 400 parents showed 98% chose acupuncture for their child when offered for tonsillectomy pain relief.9 A systematic review of the literature found most adverse events in pediatric acupuncture were categorized as mild, such as pain and bruising.10 In a 2021 guideline on procedure‐specific postoperative pain management recommendations for tonsillectomy, interventions that improved postoperative pain were paracetamol, nonsteroidal anti‐inflammatory drugs (NSAIDs), intravenous dexamethasone, ketamine (only assessed in children), gabapentinoids, dexmedetomidine, honey, and acupuncture.11 With a strong desire to avoid opioids and the concern for bleeding from postoperative NSAIDs, acupuncture presents an attractive option for pain control.
Smell dysfunction is a well-documented symptom of COVID-19 illness, which recovers in the majority of patients. A German study published in Otolaryngology-Head and Neck Surgery in 2010 found positive results using acupuncture in a small historical cohort study of 15 patients with post-viral olfactory dysfunction. The mean time with smell loss in the group was 4.3 years (range 2-10). Eight patients had improved smell using Sniffin’ Sticks test as a measurement tool, following 10 weekly sessions of acupuncture.12
Within the realm of head and neck cancer, Matovina et al. reported on the use of acupuncture as an integrative therapy for symptom management of xerostomia, pain, nausea/vomiting, and pain after neck dissection. Their review suggested that acupuncture may be a therapeutic option for patients with head and neck cancer suffering from these adverse effects of treatment.13
With the emerging evidence base for acupuncture use in tonsillectomy, there remain barriers to adoption. Chief among them are training and regulations. States in the U.S. differ in their regulation of acupuncture practice, with some requiring 300 hours of specific training and others open to medical practitioners without additional training. One resource may be the American Academy of Medical Acupuncture at https://medicalacupuncture.org/. Beyond this, there is the time required for counseling and procedure. Finally, the billing and payment for acupuncture is not uniform among insurance providers.
Despite these challenges, interest in this centuries-old practice remains high, judging from continued research and attendance at acupuncture proffered courses for the AAO-HNSF Annual Meeting. More questions remain to be answered, including the individual attributes that may affect acupuncture efficacy, as well as the optimal timing and specific regimen for its application.
















![03 Bites Better Hearing And Speech Graphic [converted]](https://img.ascendmedia.com/files/base/ascend/hh/image/2022/04/03_Bites_Better_Hearing_and_Speech_graphic__Converted_.6268225925563.png?auto=format%2Ccompress&fit=crop&h=191&q=70&w=340)


