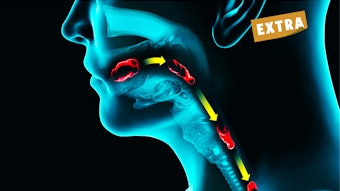
A Resident’s Perspective: The Role of Sleep Surgeons in the Treatment of OSA
Reports of obstructive sleep apnea as a formal diagnosis were first made in the 1950s, but it would be decades before the effective treatments were developed.
Dylan Bertoni, MD, Resident, PGY-4, Otolaryngology—Head and Neck Surgery, Thomas Jefferson University Hospital

I have been unknowingly surrounded by sleep apnea for my entire life. I’ve never quite understood how my mother could sleep given the volume of snoring that emanates from my father at night. The sweet English bulldog I grew up with almost certainly had the canine equivalent of obstructive sleep apnea (OSA). My grandmother frequently forgot to pack her continuous positive airway pressure (CPAP) machine when traveling. My father-in-law complains about how irritated his nose gets from his nasal CPAP mask. Sleep apnea has become so ubiquitous in our lives, it has become easy to ignore; we become blind to it and the effects it has on those around us. I certainly wasn’t thinking about sleep apnea when applying to residency.
 Dylan Bertoni, MD
Dylan Bertoni, MD
It wasn’t until matching into residency at Thomas Jefferson University that I considered the role of the sleep surgeon. With Thomas Jefferson having dedicated sleep-trained faculty serving as the residency program director and assistant program director, as well as one of the busiest hypoglossal nerve implant centers in the country, I could no longer remain blind to the OSA surrounding me.
OSA is a relatively recently identified pathology. Charles Dickens is frequently credited as first describing a sleepy patient in The Pickwick Papers in 1836. Reports of OSA as a formal diagnosis were first made in the 1950s, but it would be decades before the development of effective treatments. At that time, divorce was an acceptable solution for snoring. Tracheostomy was the only medical treatment to cure Pickwickian syndrome, and even that wasn’t used until the 1970s. CPAP was introduced as a treatment in 1981—the same year the uvulopalatopharyngoplasty was first performed in the United States. Although the field of sleep surgery continued to slowly smolder, the advent and effectiveness of CPAP led to the explosion of medical sleep specialists, predominantly pulmonologists, managing these patients.
The U.S. obesity epidemic has only exacerbated this country’s snoring problem. Recent studies have shown that although effective, the discomfort and inconvenience of CPAP use leads to poor compliance and decreased overall efficacy. CPAP remains the first-line treatment for moderate to severe OSA, but my grandma and father-in-law were onto something—there has been a gap in our treatment of these patients. In recent years, this gap has been explored by the otolaryngologist. With the advent of the hypoglossal nerve stimulator in 2014, sleep surgery has become a sleek alternative to CPAP in the appropriate patient. The number of available surgical options continues to grow, further driving the market for a surgeon capable of managing patients who are dissatisfied with their masks and their tubes. The current job market is catching on as well, with both private and academic institutions looking to expand their reach with trained sleep surgeons.
As a resident, I am still fascinated by those 18-hour free flap surgeries, but as a father to a 7-month-old baby, they have started to feel a lot more like 18-hour cases. I find myself drawn toward a field that can still have profound impact on patients but allows me the freedom to make it home for bath time. My exposure to the surgical treatments for OSA has opened my eyes to the prevalence and impact that sleep apnea can have and has influenced how I see and speak to those in my life afflicted by it. Daisy the bulldog might not have been a candidate for sleep surgery, but other members of my family, or yours, just might be. My hope is that I, along with my fellow otolaryngology-head and neck surgery residents across the country, can continue to learn from faculty sleep surgeons, so we can further address this growing need.