The Worst Spring Pollen Season Ever?
Tips for incorporating allergy testing and immunotherapy into your practice help you address the growing need to treat allergic conditions.
Cecelia Damask, DO, Chair, Allergy, Asthma and Immunology Committee, and Matthew W. Ryan, MD

Using long-term data from 60 North American pollen stations over a 30-year period, Anderegg et al. quantified the role of climate change in patterns of pollen concentration and discovered widespread advances and lengthening of pollen seasons (up to 20 days) and increases in pollen concentrations (up to 21%) across North America, strongly coupled to observed warming.1 These longer and more intense pollen seasons are expected to contribute to seasonal allergic rhinitis and allergic asthma.
Temperature affects the number of winter frost days as well as spring frost-free days and is strongly associated with the timing of pollen seasons, including the start date, peak emission date, end date, and duration.2 Over the past several decades, warmer temperatures have been observed to drive earlier (by 3-22 days) pollen season start dates for spring-flowering trees as well as prolonged pollen seasons have been recorded for both trees and weeds. Increasing atmospheric CO2 concentrations potentially enhance photosynthetic capacity thereby increasing pollen production.3 Furthermore, higher CO2 concentrations have been observed to increase both the quantity of male flowers and their allergenic protein contents.
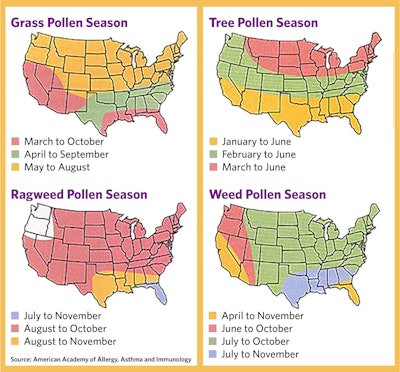
Using historical pollen data and predictive climate models, Zhang and Steiner in a recent publication projected that under future climate scenarios in the U.S., the spring pollen season will start even earlier (up to 40 days earlier) and last longer (19 days longer) with continued temperature change, and the annual total pollen emission will also increase (by 16%-40%).4 Rising temperatures driven by increasing amounts of greenhouse gases in the atmosphere are thought to be the main factor. As average temperatures rise steadily because of climate change, we are only going to see spring starting earlier and lasting longer. Historically, trees have dominated the spring pollen season, followed by grass pollen in late summer, and weeds in the fall. But Zhang and Steiner found that their new model also predicts that these seasons will overlap in the summer when warming temperatures cause some trees to pollinate longer and some grasses to pollinate earlier.
For people with allergies and/or asthma, these potential increases in the duration of the pollen seasons and the amount of pollen produced could have serious consequences and only multiply their misery. Allergic rhinitis (AR) is a comorbidity with many other diseases and conditions treated by otolaryngologists and shares significant symptom overlap with a variety of diseases relevant to our practices. Currently there is a growing need for specialists to treat allergic conditions, and otolaryngologists are uniquely positioned to assess for the presence of allergic disease in patients with upper aerodigestive tract symptoms. Incorporating allergy testing and immunotherapy into your practice allows you to provide comprehensive care to patients and, as an ancillary service, can help build your practice.
Incorporating Allergy Testing and Immunotherapy into Your Practice
Allergy diagnostic testing is one of the first services you can offer your patients. Although a presumptive diagnosis of allergic disease may be made from the patient’s history, allergy testing has several important roles. These include confirmation of the clinical diagnosis, identification of the patient’s relevant allergen sensitivities, and selection of a safe starting dose for immunotherapy.
Several different testing modalities are available. Allergen-specific IgE in the serum can be used as a marker of sensitization. An in vitro-specific IgE test may be accomplished with a simple blood draw and sent out to a reference laboratory. The most commonly employed allergy testing technique is skin testing. A simple prick test performed with an allergen extract and a plastic disposable device can identify preformed allergen-specific IgE via cutaneous mast cell degranulation and the classic wheal-and-flare reaction of the skin. Another technique is to use a small needle to inject diluted allergen into the dermis and look for a similar reaction (intradermal test).
Some practices may choose to incorporate a blended technique of both prick and intradermal tests, commonly known as “modified quantitative testing.” Allergy diagnostic testing provides the clinician with important information to aid in clinical decision making and is a cornerstone in the management of allergic disease. Most otolaryngology practices should be able to add some form of allergy diagnostic testing with minimal investment.
Most patients with AR are treated with allergen avoidance and pharmacotherapy. However, allergen-specific immunotherapy is the only treatment that addresses the underlying immunologic derangement in allergic disease. Successful immunotherapy decreases symptoms and improves disease-specific quality of life.5 Immunotherapy achieves these benefits via a variety of mechanisms. It reduces mast cell and basophil degranulation, induces the production of IgG4 blocking antibody, upregulates tolerogenic regulatory T-cell populations, and reduces allergen-specific IgE over the long term. Comprehensive allergy care thus includes allergen-specific immunotherapy.
A variety of immunotherapy options are used in practice. The simplest method for allergen-specific immunotherapy is sublingual immunotherapy (SLIT) using Food and Drug Administration (FDA)-approved sublingual tablets. These are currently available for the treatment of grass, ragweed, and dust mite allergies. Another option is SLIT using a customized formulation of aqueous allergen extracts that is based upon clinical determination of a patient’s relevant allergen sensitivities. The advantage of this approach is allergens other than grass, ragweed, and dust mite can be treated.
Although SLIT has many advantages, the mainstay of immunotherapy in the U.S. is subcutaneous injection immunotherapy (SCIT). SCIT has the longest track record of clinical use and has been demonstrated to be effective in multiple randomized placebo-controlled trials.6 SCIT is FDA approved and covered by most health insurance plans. Although SLIT is used by many practices in one form or other, most allergy practices use SCIT for these reasons.
Otolaryngologists have a variety of reasons for incorporating comprehensive allergy care into their practices. Before initiating these services, a practice should consider its goals as well as the requirements for success.
Like any other decision involving the services offered by your practice, incorporating allergy care should be undertaken with a business plan in mind. The business plan should include tangible metrics of success: monitoring of referral trends, financials, retention rates of patients, and analyzing patient outcomes.
The primary financial investment when starting an allergy practice is the cost of supplies. These include allergen extracts, syringes, testing devices, and emergency supplies (for anaphylaxis treatment). Usually, the existing personnel in a medical office are able take on the new roles required for allergy care. These roles include performance of allergy skin tests, preparation of testing and immunotherapy vials, and administration of immunotherapy. Medical office assistants or nurses are able to perform these duties depending upon individual state regulations. Ultimately, successful allergy practices will have personnel who are completely dedicated to providing these services.
Office space for the allergy practice must also be considered. A location for preparation of allergen extracts needs to be defined as well as space for testing and administration of immunotherapy injections. Because SCIT carries with it a risk for anaphylaxis, a monitored location within the office will need to be designated for patient observation after injections are administered. When beginning an allergy practice, existing office space can be usedt. However, as the practice grows, so will requirements for space. An ideal office environment includes a dedicated check-in desk for allergy patients, a separate waiting room for observation, and an allergenic extract compounding area as well as space for testing multiple patients simultaneously and giving injections.
Although office staff perform most of the day-to-day tasks, the physician (or advanced practice provider) is the leader of the team and should be the content expert for every aspect of the allergy practice, including the nuances of testing and immunotherapy, management of allergy emergencies, regulatory and compliance issues, proper billing and coding, and documentation. This responsibility entails considerable investment of time and energy on the part of the physician.
Becoming an expert in these topics can be accomplished in a variety of ways. Trusted colleagues are a potential source of information and advice. Allergy-specific CME offerings at the AAO-HNSF Annual Meeting & OTO Experience and from other sources should be used. Read a variety of texts and monographs on allergy directed toward otolaryngologists. Talk to allergen supply vendors. And finally, enroll in a course that reviews proper billing and compliance information.
There is never an ideal time to get started on the journey of building an allergy practice. Fortunately, allergy services can be gradually added to what you are already offering your patients. It is OK to start slowly. Allergy testing is a simple starting point. In vitro testing and skin prick testing are easy to introduce into your practice flow. Sublingual immunotherapy tablets are a safe and effective way to begin offering immunotherapy to your patients. As you and your staff learn more about allergy and are more comfortable with your knowledge and skills, you can expand to offer a full spectrum of allergy services.
References
- Anderegg WRL, Abatzoglou JT, Anderegg LDL, Bielory L, Kinney PL, Ziska L. Anthropogenic climate change is worsening North American pollen seasons. Proc Natl Acad Sci U S A. 2021 Feb 16;118(7):e2013284118. doi: 10.1073/pnas.2013284118. PMID: 33558232; PMCID: PMC7896283.
- Ziska L H, Makra L, Harry SK, et al. Temperature-related changes in airborne allergenic pollen abundance and seasonality across the northern hemisphere: a retrospective data analysis. Lancet Planet Health. 2019;3(3):e124-e131. doi: 10.1016/S2542-5196(19)30015-4
- LaDeau S, Clark J. Pollen production by Pinus taeda growing in elevated atmospheric CO2. Funct Ecol. 2006;20(3):541-547. doi.org/10.1111/j.1365-2435.2006.01133.x
- Zhang Y, Steiner AL Projected climate-driven changes in pollen emission season length and magnitude over the continental United States. Nat Commun. 2022;13(1):1234. doi: 10.1038/s41467-022-28764-0
- Wise SK, Damask C, Roland LT, et al. International consensus statement on allergy and rhinology: allergic rhinitis - 2023. Int Forum Allergy Rhinol. 2023 Apr;13(4):293-859. doi: 10.1002/alr.23090. Epub 2023 Mar 6. PMID: 36878860.
- Wise SK, Damask C, Greenhawt M, et al. A synopsis of guidance for allergic rhinitis diagnosis and management from ICAR 2023. J Allergy Clin Immunol Pract. 2023 Mar;11(3):773-796. doi: 10.1016/j.jaip.2023.01.007. PMID: 36894277.