Tinnitus Instability/Fluctuation: The Most Important Variable in Tinnitus Care
Emerging clinical observation suggests that tinnitus stability is a more mechanistically informative dimension.
Hamid R. Djalilian, MD, Yalda Yazdani, MD, Ella Lee, BS, Dina Kianiazar, BS, and Morgan Nash, MA, on behalf of the Hearing Committee
(See author’s disclosures at the end of this article.)

Some patients experience tinnitus that remains relatively consistent (stable, constant tinnitus), allowing the brain to classify the signal as familiar and gradually reduce its salience. Others develop a percept that fluctuates unpredictably, often worsening with physiologic stressors such as sleep disruption, illness, hormonal changes, or sensory overload (e.g., sound, etc.). These recurrent spikes in tinnitus (instability) recapture attention, disrupt adaptive filtering, and help explain why patients with similar loudness scores follow markedly different clinical trajectories.3
Importantly, emotional distress often follows the sensory change rather than causing it. When tinnitus is unstable (intermittent spikes), the brain is forced to reassess continually, preventing the signal from being consolidated as irrelevant background noise. Distress in these cases appears downstream of network volatility rather than its primary driver.4
Stability provides a clinically observable expression of underlying brain state, unifying major neuroscientific frameworks by distinguishing regulated auditory function from systems vulnerable to recurrent disturbance.
Working Clinical Construct
Stable tinnitus: A persistent percept that remains generally consistent in loudness and character, without routine worsening or fluctuations. Usually quiet during the day and only perceptible when very quiet.
Unstable tinnitus: A percept characterized by unpredictable or trigger-sensitive shifts in loudness or intrusiveness. Patient experiences “good days” and “bad days.” On bad days, the tinnitus takes over attention, and patients feel they cannot escape from it.
This construct is intended to augment clinical reasoning by capturing system behavior rather than focusing solely on loudness or distress.
From Neurophysiological Models to Brain Network Theory
Jastroboff’s neurophysiological model reframed tinnitus as a disorder of central auditory processing shaped by limbic and autonomic systems rather than peripheral injury alone.5 Modern brain network theories extend this view, describing tinnitus as the product of altered interactions among circuits governing salience (attention), emotion, and cognitive control. For example, the triple network model, integrating the salience, default mode, and executive networks, provides a clear structural map for persistent awareness and distress.6
The challenge is that brain networks are inherently dynamic. This means that the more clinically relevant question is not simply which networks are involved, but what determines how and when they are activated. Symptom stability offers a functional answer:
Stable tinnitus represents a prerequisite neural condition for adaptation. When tinnitus is stable, emotional reactions (limbic escalation) diminish, threat signaling softens, and neural reorganization (neuroplasticity) can occur.7
Unstable tinnitus reflects recurrent network activation in which fluctuations repeatedly engage salience (attention), limbic, and autonomic systems. Each shift is processed as a novel sensory event, sustaining vigilance and reinforcing suffering.6
In this way, network models define the circuitry of tinnitus, while stability helps explain both the dynamic equilibrium and the brain's ability to reorganize and heal.
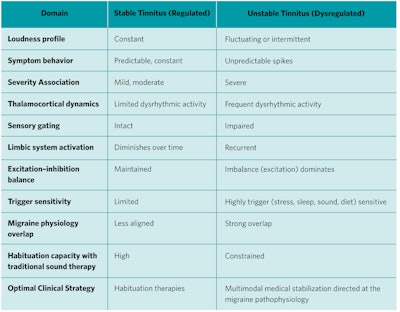
Table 1. Characteristics of Stable vs. Unstable Tinnitus.
Thalamocortical Dysrhythmia as the Neural Signature of Instability
Thalamocortical dysrhythmia (TCD) provides an important neurophysiological account of tinnitus, describing how alterations in thalamic neurons can allow internally generated activity to reach conscious perception through abnormal oscillatory coupling.8
Critically, TCD does not appear in all tinnitus cases, suggesting it may reflect the regulatory state of the auditory brain rather than the mere presence of a phantom percept.9 Clinical behavior reinforces this distinction. Tinnitus that turns on and off (intermittent tinnitus) or fluctuates without peripheral change points toward a dynamically regulated central process.
Hearing loss alone does not reliably produce fluctuating or intermittent tinnitus. Modeling studies indicate that dysrhythmia emerges only when hearing loss-related central auditory activation starts tinnitus, but the central attention center modulates the tinnitus.10
Viewed this way, TCD is best understood as the electrophysiological expression of instability. From a thalamocortical perspective:
Stable tinnitus likely reflects a system operating outside an active dysrhythmic state, with sufficient inhibitory control to permit perceptual down-regulation.
Unstable tinnitus suggests a brain repeatedly entering dysrhythmic modes, where fluctuating excitability refreshes the percept and continually recruits salience and limbic networks, preventing habituation.
This framing shifts the clinical question. Rather than asking only if TCD patterns are present, we must ask what allows the thalamus to lose regulatory control. This naturally leads to an investigation of impaired sensory gating, the putative upstream failure that permits dysrhythmic activity to emerge.11
Sensory Gating, Instability, and the Biological Preconditions for Habituation
Sensory gating is the brain’s capacity to suppress redundant input before it reaches awareness. For example, when you have shoes on, the neural signal from your feet constantly reaches the brain, but after perceiving a repeated signal, sensory gating reduces attention to or blocks that signal. This is why we are not constantly aware of shoes on our feet, but if our eyes are closed, we can tell if we have shoes on by unblocking that signal when our attention is directed to it.
Within the auditory system, the medial geniculate body acts as a primary inhibitory filter, regulating whether signals, including internally generated activity, gain cortical access.11 When this inhibitory control weakens, the tinnitus percept is no longer treated as background noise but repeatedly re-enters awareness. This breakdown aligns closely with thalamocortical dysrhythmia, as both reflect instability within inhibitory thalamocortical circuits. Dysrhythmic oscillations signal loss of regulatory control, while impaired gating explains why the percept cannot be effectively suppressed.8, 11
Importantly, sensory gating capacity correlates with tinnitus severity. Neurophysiologic and behavioral data show poorer gating in individuals with more bothersome or decompensated tinnitus, along with broader cortical recruitment as severity increases.12, 13 Unpredictability, therefore, carries physiologic consequences. A fluctuating percept is less easily categorized as safe and more likely to sustain attentional and limbic engagement.
Habituation is fundamentally a neurophysiologic process requiring consistent inhibitory regulation. When filtering remains stable (stable tinnitus), repeated input can be deprioritized, and neural responses attenuate. When inhibitory control is unreliable (unstable fluctuating tinnitus), the signal repeatedly reasserts itself as salient, constraining adaptive down-regulation.13 From a gating perspective:
Stable tinnitus suggests inhibitory filtering that is consistent enough for the brain to gradually reduce the percept’s priority.
Unstable tinnitus reflects a breakdown of filtering in which the signal repeatedly re-enters awareness, maintaining network engagement and limiting adaptation.
Stability, in this sense, functions less as a descriptive feature and more as a biological prerequisite for habituation.
Migraine as a Biological Model of Brain Network Instability
Migraine is increasingly understood as a sensory processing disorder characterized by excitation-inhibition imbalance and sensory gating deficits.14 Across sensory systems, migraine brains demonstrate impaired habituation to repeated stimulation, reflecting reduced inhibitory control and heightened cortical responsiveness.15 This inability to habituate to repeated stimulation can manifest itself as light, sound, and motion sensitivity, among others. Evoked potential studies consistently show that, unlike healthy brains, migraine brains fail to dampen their response to repetitive input. Instead of decreasing over time, neural responses remain amplified, suggesting a fundamental disturbance in adaptive filtering.15
This physiology maps directly onto the tinnitus stability construct. Triggers such as sleep disruption, hormonal fluctuation, illness, sensory overload, and metabolic stress do not create new structural injury. Rather, they transiently alter brain excitability, shifting the brain into a sensitized state in which ordinary stimuli acquire exaggerated perceptual weight.16, 17, 18 This reflects a brain operating near the threshold of excitability. Within a migraine-informed framework:
Stable tinnitus may emerge when excitability remains sufficiently constrained for inhibitory filtering to function with relative consistency. In stable tinnitus, the cortical activity is below the excitability threshold.
Unstable tinnitus may reflect a sensitized network state in which fluctuating excitability repeatedly amplifies the auditory signal and goes above the excitability threshold.
This framing implies that unstable tinnitus is a migraine variant. In this way, stability represents the boundary between a brain capable of adaptation and one that remains biologically primed for sensory escalation. It also provides a roadmap for medical interventions to restore neurophysiologic stability.
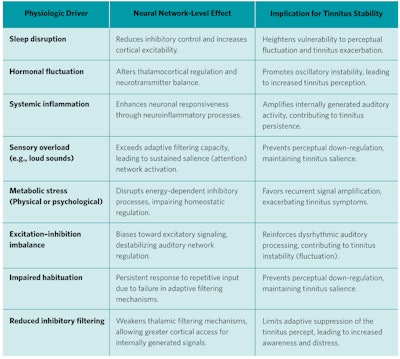
Table 2. Physiologic Drivers of Network Instability in Migraine and Tinnitus.
Clinical Implications: Stability as a Marker of Regulatory State
Symptom stability can be identified in a standard tinnitus history, yet it often reveals something severity scores cannot: whether the auditory system is sitting in a relatively regulated equilibrium or cycling through a state of active dysregulation.
That pattern matters because it changes what “treatability” looks like. In many cases of unstable (fluctuating) tinnitus, the clinical behavior is most consistent with a migraine-style sensory processing state: a brain that is intermittently hyperexcitable, less able to inhibit repetitive input, and prone to volatility across multiple sensory domains.14 These patients have intermittent tinnitus or tinnitus that can be very loud some days and very quiet other days.
If unstable tinnitus is, in a meaningful subset of patients, a migraine-variant expression of network instability, then it is not merely something to “habituate to.” It is potentially stabilizable, and therefore treatable, because migraine physiology is treatable.19, 20
Stability as a Triage Guide: Habituation vs. Stabilization
Habituation is not purely psychological; it depends on sufficiently consistent inhibitory regulation so the brain can learn that the signal is familiar and safe enough to ignore. Stable tinnitus more often provides that consistency. Unstable tinnitus repeatedly re-triggers attention and threat appraisal, keeping salience and limbic circuitry engaged. This triggers an emotional reaction, further increasing attention to and thus the loudness of the tinnitus. In this sense, tinnitus stability becomes a triage variable:
Stable tinnitus: Habituation-based interventions (CBT, sound therapy) are appropriate as first-line strategies.
Unstable tinnitus: Consider medical protocols aimed at stabilizing network excitability (e.g., atypical migraine), with standard interventions as part of a multimodal strategy.19, 20
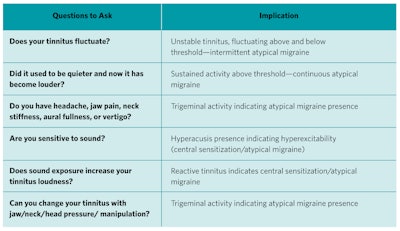
Table 3. Questions to ask patients to evaluate for unstable, atypical migraine-related tinnitus.
Take Home Points to Remember
- Fluctuating and intermittent (unstable) tinnitus causes more distress for patients because it causes an unpredictable course of the tinnitus.
- Patients often have “good days” when the tinnitus is very quiet or even silent, and “bad days” when it is very loud.
- Fluctuating, unstable tinnitus is driven by the atypical migraine pathophysiology and is triggered by stress, poor sleep, diet, hormonal changes, and overstimulation (e.g., sound, weather changes).
- Treatment of unstable (fluctuating) tinnitus requires controlling the migraine pathophysiologic process (medications and lifestyle changes) before attempting habituation (e.g., sound therapy) regimens.
Author’s disclosures: Dr. Djalilian is an advisor and equity holder in Elinava Technologies, Finally Quiet!, and NeuroMed Care LLC. He has granted and pending patents related to devices and medications related to tinnitus. The companies with which the author is affiliated had no role in the conception, design, execution, or interpretation of this paper. The other authors have no conflicts of interest.
References
- Bauer CA. Tinnitus. New England Journal of Medicine. 2018;378(13):1224–1231. doi:10.1056/NEJMcp1702408
- Langguth B, Elgoyhen AB, Cederroth CR. Tinnitus: Clinical insights into its pathophysiology and treatment. Journal of the Association for Research in Otolaryngology. 2024;25:1–18.
- Dawes P, Cruickshanks KJ, Fischer ME, et al. Natural history of tinnitus in adults: A cross-sectional and longitudinal analysis. BMJ Open. 2020;10:e041290. doi:10.1136/bmjopen-2020-041290
- De Ridder D, Schlee W, Vanneste S, et al. Tinnitus and tinnitus disorder: Theoretical and operational definitions (an international multidisciplinary proposal). Progress in Brain Research. 2021;260:1–25. doi:10.1016/bs.pbr.2020.12.002
- Jastreboff PJ. Phantom auditory perception (tinnitus): Mechanisms of generation and perception. Neuroscience Research. 1990;8(4):221–254. doi:10.1016/0168-0102(90)90031-9
- De Ridder D, Vanneste S, Langguth B, Llinás R. Thalamocortical dysrhythmia: A theoretical update in tinnitus. Frontiers in Neurology. 2015;6:124. doi:10.3389/fneur.2015.00124
- Rauschecker JP, Leaver AM, Mühlau M. Tuning out the noise: Limbic-auditory interactions in tinnitus. Neuron. 2010;66(6):819–826. doi:10.1016/j.neuron.2010.04.032
- Llinás RR, Ribary U, Jeanmonod D, Kronberg E, Mitra PP. Thalamocortical dysrhythmia: A neurological and neuropsychiatric syndrome characterized by magnetoencephalography. Proceedings of the National Academy of Sciences USA. 1999;96(26):15222–15227. doi:10.1073/pnas.96.26.15222
- Adjamian P, Sereda M, Zobay O, Hall DA, Palmer AR. Neuromagnetic indicators of tinnitus and tinnitus masking in patients with and without hearing loss. Journal of the Association for Research in Otolaryngology. 2012;13(5):715–731. doi:10.1007/s10162-012-0340-5
- Gault R, McGinnity TM, Coleman S. A computational model of thalamocortical dysrhythmia in people with tinnitus. IEEE Transactions on Neural Systems and Rehabilitation Engineering. 2018;26(6):1212–1223. doi:10.1109/TNSRE.2018.2831667
- Caspary DM, Llano DA. Auditory thalamic circuits and GABA receptor function: Putative mechanisms in tinnitus pathology. Hearing Research. 2017;349:197–207. doi:10.1016/j.heares.2016.09.015
- Morse K, Vander Werff KR. Cortical auditory evoked potential indices of impaired sensory gating in people with chronic tinnitus. Ear and Hearing. 2024;45(1):34–45.
- Mohebbi M, Farhadi M, Daneshi A, Mahmoudian S. Toward an exploration of habituating to tinnitus: Perspectives on sensory gating. Journal of the American Academy of Audiology. 2019;30(10):896–903. doi:10.3766/jaaa.18038
- Coppola G, Di Lorenzo C, Schoenen J, Pierelli F. Habituation and sensitization in primary headaches. The Journal of Headache and Pain. 2013;14:65. doi:10.1186/1129-2377-14-65
- Schoenen J, Wang W, Albert A, Delwaide PJ. Potentiation instead of habituation characterizes visual evoked potentials in migraine patients between attacks. European Journal of Neurology. 1995;2(2):115–122.
- Hwang JH, Tsai SJ, Liu TC, Chen JC, Lai JT. Association of tinnitus with a history of migraine: A nationwide population-based study. JAMA Otolaryngology–Head & Neck Surgery. 2018;144(8):712–717. doi:10.1001/jamaoto.2018.0939
- Lee A, Abouzari M, Akbarpour M, Risbud A, Lin HW, Djalilian HR. A proposed association between subjective nonpulsatile tinnitus and migraine. World J Otorhinolaryngol Head Neck Surg. 2022 Oct 13;9(2):107-114.
- Goshtasbi K, Abouzari M, Risbud A, Mostaghni N, Muhonen EG, Martin E, Djalilian HR. Tinnitus and Subjective Hearing Loss are More Common in Migraine: A Cross-Sectional NHANES Analysis. Otol Neurotol. 2021 Oct 1;42(9):1329-1333. doi: 10.1097/MAO.0000000000003247. PMID: 34238896; PMCID: PMC8590584.
- Dichter A, Bhatt K, Gutiérrez Pérez ML, Lee EJ, Tawk K, Djalilian HR. Potential therapeutic role of calcitonin gene-related peptide medications for tinnitus. J Chin Med Assoc. 2026 Jan 30. doi: 10.1097/JCMA.0000000000001351. Epub ahead of print. PMID: 41612541.
- Abouzari M, Tawk K, Kim JK, Larson ED, Lin HW, Djalilian HR. Efficacy of Nortriptyline-Topiramate and Verapamil-Paroxetine in Tinnitus Management: A Randomized Placebo-Controlled Trial. Otolaryngol Head Neck Surg. 2025 Apr;172(4):1348-1356. doi: 10.1002/ohn.1063. Epub 2024 Nov 26. PMID: 39588680; PMCID: PMC12579525.