Challenges Communicating with Hard of Hearing Patients
Effective communication is essential for safe, ethical, and high-quality medical care. It supports accurate diagnosis, shared decision‑making, treatment adherence, and patient satisfaction.
Gauri Mankekar, MD, PhD, and Isaac Erbele, MD, on behalf of the AAO-HNS Hearing Committee

Otolaryngologist: “Mr. Miller, when did you first notice your hearing loss?”
Mr. Miller (with a blank look): “I’m sorry, I can't understand. Can you please say that again? I left my hearing aids in the truck. They don’t really help, and I thought you might have to look at my ears.”
Otolaryngologist (in a raised voice, speaking slowly, enunciating carefully): “Is someone here with you?”
Mr. Miller: “No. I live alone. My children have moved away.”
Otolaryngologist (in a raised voice): “Can you lip-read?”
Mr. Miller: “Not really. I also have blurred vision.”
Otolaryngologist: “Can I get you a hearing amplifier?”
Otolaryngologists, and especially otologists/neurotologists, are attuned to working with hearing-impaired (HI) individuals but can still face challenges. A survey of the AAO-HNS Hearing Committee showed that 85% of members found it challenging to communicate with HI patients, with 57% reporting challenges in being understood by their patients.
Likely, our physician colleagues in other specialties are also facing similar challenges in communicating with HI patients in their clinics and inpatient settings. An article by Leary et al highlighted that, despite the best intentions to communicate effectively, healthcare teams often fail to identify patients’ hearing impairment and disability. Communication failures lead to incomplete histories, misunderstandings, delayed diagnosis, incorrect assumptions of risks and benefits, and inadequate informed consent.1,2
Effective communication is fundamental for safe, ethical, and high-quality medical care. It underpins accurate diagnosis, shared decision‑making, treatment adherence, and patient satisfaction. For individuals who are HI, communication with physicians is often complicated by linguistic, cultural, and systemic barriers. In the United States, one out of seven individuals aged 12 years or older and more than 66% individuals aged 70 or older have bilateral hearing loss.3 Many of these individuals have a shorter duration of hearing loss with less time to adapt and learn skills such as lip reading and sign language. Despite legal and ethical mandates to provide accessible healthcare, many physicians and healthcare teams remain insufficiently equipped and struggle to communicate effectively with HI patients.
Challenges from the Diversity of the HI Population
A significant challenge arises from the diversity of the HI population itself. Some patients have long-duration hearing loss, while others have short-duration hearing loss. Some patients have unilateral hearing loss while others have bilateral hearing loss. Some patients have mild hearing loss, while others may have moderate to severe and even profound hearing loss. Some HI patients speak a foreign language. So, HI patients vary widely in their communication preferences and needs. Although some individuals rely primarily on spoken language with amplification devices, others with long-duration hearing loss are adept at lip‑reading, or culturally Deaf individuals often use American Sign Language (ASL) as their first language.4,5
Although it is assumed that lip-reading or written notes are universally effective, research demonstrates that lip-reading allows comprehension of only a fraction of spoken language and is particularly ineffective for complex medical terminology.3,6 This is exacerbated by using face masks, and everyone experienced this during the COVID-19 pandemic. Learning gaps can interfere with HI patients' understanding of written notes. Reading comprehension scores in HI students have been reported to be significantly lower than in their hearing peers, and this deficit can persist into adulthood.7,8
Certified sign language interpreters are recognized as the most effective means of communication for Deaf patients who use ASL. Studies show they are used in a small minority of healthcare encounters with HI patients.3,6 For HI patients not using ASL, clinicians frequently rely on ad hoc strategies such as writing notes, using gestures, or asking family members to interpret. These approaches are associated with higher risks of miscommunication, breaches of confidentiality, and medical errors.2,5 Such practices also place an unfair burden on patients and families, undermining patient autonomy and safety. Sometimes older patients live independently and do not have family or friends to accompany them to their physician visits or help with translation.
Another major challenge is the lack of formal training in medical education on communicating with HI patients. Many physicians report minimal exposure to Deaf culture, to disability communication strategies, or to effective use of interpreters or amplification devices during their training.9,10 This educational gap can contribute to inconsistent communication practices and reinforce reliance on ineffective methods. Evidence suggests that targeted training interventions can significantly improve clinicians’ confidence and self-efficacy in communicating with HI patients, yet such programs remain uncommon in medical curricula.11
Effective Communication Often Requires Additional Time
Time pressure within modern healthcare systems further complicates communication with HI patients. Effective communication often requires additional time to arrange interpreters, ensure appropriate visual access, and confirm patient understanding through strategies such as teach-back. Physicians frequently perceive these encounters as more time-consuming than those with hearing patients.9,11 In busy clinical environments, these pressures may lead to rushed explanations or incomplete communication. Such shortcuts increase the likelihood of diagnostic errors, poor treatment adherence, and patient dissatisfaction, highlighting how systemic constraints contribute to communication failures rather than individual clinician attitudes alone.
The increasing popularity of AI scribes that utilize ambient intelligence to transform clinical conversations into structured documentation helps reduce physicians’ administrative burden. However, it introduces a new level of complexity for physicians who rely on written notes to communicate with their HI patients.
Assistive technologies, including hearing amplifiers, speech-to-text applications, and video remote interpreting (VRI), can support communication. VRI systems can increase access to interpreters, especially in rural or emergency settings, and can be useful when supported by reliable technology and proper implementation. Computer-Assisted Real-Time Transcription (CART) is a service that provides instant access to spoken-word-to-text communication for individuals with HI. It is offered both on-site and remotely using video-conferencing platforms like Zoom, Microsoft Teams, or Cisco Webex by certified professionals and vendors. Technical failures, poor video quality, or inadequate screen placement can significantly impair communication and frustrate both physicians and patients.
Members of the Hearing Committee report using a large font on laptop-written notes, speech-to-text apps, and Google Translate to communicate with their HI patients. One member stated that they are in the process of acquiring a pair of speech-to-text captioning glasses for communication. Speech-to-text glasses provide real-time captions of conversations directly to the wearer’s field of vision using augmented reality (AR) and AI-powered speech recognition. Clinics and hospitals offering on-site hearing amplifiers, CART, speech-to-text apps, and speech-to-text glasses can help mitigate some of the challenges and improve physician communication with HI patients.
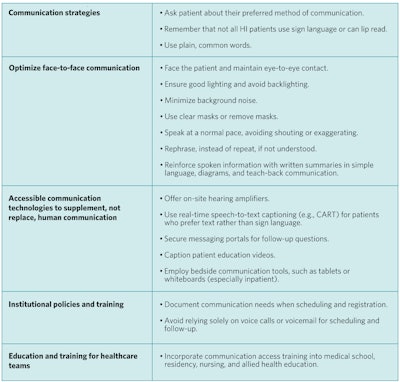
Table 1. Strategies for addressing challenges and improving communication with HI patients in outpatient and inpatient settings.
Conclusion
Physicians face numerous challenges when communicating with HI patients, including population diversity, interpreter shortages, insufficient training, time constraints, and technological limitations. These barriers compromise patient safety, quality of care, and health equity. Addressing them requires systemic change, including improved access to qualified interpreters, integration of disability communication training into medical education, and institutional commitment to accessible care. By recognizing and addressing these challenges, healthcare systems can move closer to mitigating physician challenges and providing equitable, patient-centered care for HI individuals.
References
- O’Leary DP, O’Leary TJ. Communicating With Patients With Hearing Loss or Deafness—Can You Hear Me? JAMA Intern Med. 2024;184(4):345–346. doi:10.1001/jamainternmed.2023.8563
- Ali N, Cobb M. (2018). Emergency care communication barriers for deaf patients: A qualitative study. Journal of Communication in Healthcare, 11(2), 115–125. https://doi.org/10.1080/17538068.2018.1453538
- Lezzoni, LI, O’Day BL, Killeen M et al (2004). Communicating about health care: Observations from persons who are deaf or hard of hearing. Annals of Internal Medicine, 140(5), 356–362. https://doi.org/10.7326/0003-4819-140-5-200403020-00011
- Goman AM, Lin FR. Prevalence of hearing loss by severity in the United States. Am J Public Health. 2016;106(10):1820-1822. doi:10.2105/AJPH.2016.303299
- U.S. Centers for Medicare & Medicaid Services. (2023). Improving communication access for individuals who are deaf or hard of hearing. https://www.cms.gov
- Weerapol N, Leelakanok N (2024). Communication between healthcare professionals and patients with hearing loss: A systematic review and meta-analysis. American Journal of Health‑System Pharmacy, 81(12), 521–530. https://doi.org/10.1093/ajhp/zxae045
- Rogers KD, Ferguson-Coleman E, Young A. (2018). Challenges of realising patient-centered outcomes for deaf patients. The Patient-Centered Outcomes Research, 11(1), 9-16.
- Traxler CB. (2000). The Stanford Achievement Test: National norming and performance standards for deaf and hard-of-hearing students. Journal of Deaf Studies and Deaf Education, 5(4), 337-348.
- Char CA, McKee MM. (2024). Understanding the health care needs of the Deaf community through medical interpreters. American Family Physician, 110(4), 349–350. https://www.aafp.org
- McFadden SE. (2025). Interactions between the Deaf community and healthcare (undergraduate honors thesis). University of Mississippi. https://egrove.olemiss.edu/hon_thesis/3206
- Grazioli VS, Morisod K, Bodenmann P, Singy P. (2022). Improving communication with hard of hearing and D/deaf patients: A capacity‑building intervention. European Journal of Public Health, 32(Suppl. 3). https://doi.org/10.1093/eurpub/ckac129.178