Bridging the Gap: A Cleft Lip and Palate Mission to China
Abby R. Nolder, MD PGY-5 resident, University of Arkansas for Medical Sciences, Department of Otolaryngology—Head and Neck Surgery In July 2010, I joined a group of nine dedicated physicians, nurses, and coworkers on a cleft-lip and palate surgical mission to Hangzhou, China. The team was led by Lisa M. Buckmiller, MD, director of the vascular anomalies center of excellence and the cleft lip and palate team at Arkansas Children’s Hospital in Little Rock, AR. Dr. Buckmiller has taken part in and led many international surgical missions to China, Africa, and Central America. She is very involved in the pediatric otolaryngology and cleft fellowship program at Arkansas Children’s Hospital. One of her former fellows, Robert Glade, MD, now a pediatric otolaryngologist and cleft surgeon at Oklahoma University Medical Center in Oklahoma City, OK, was part of the team as well. In cooperation with the Operation Smile Charity Hospital, Hangzhou, our Change of Face Mission Team provided cleft lip and/or cleft palate surgeries for 20 Chinese children. Many of the children were residents of the Starfish Foster Home, a special place founded by a South African school teacher, Amanda de Lange, to save the lives of Chinese orphans with special health needs. Some of the children and their caretakers traveled more than 50 hours by train in the sweltering summer heat to reach the hospital. The tireless work and dedication shown by Amanda and her volunteers was a true testament to their commitment to providing these children with a better life. This made our contribution even more rewarding. The Operation Smile Charity Hospital was well-equipped with two operating suites as well as a pre- and postoperative patient ward with 24-hour nursing care. We worked closely with the Operation Smile surgeons in evaluating the patients preoperatively to determine the appropriate procedure and timing for each patient. The operating room staff was skillful and efficient. The surgeries went smoothly, and the transformations were amazing. Our team provided the children with medications, diapers, arm restraints (“no-no’s”) and feeders, all much-needed supplies for the long trip back to the foster home. In China, one in 600 children is born with a cleft deformity. These children, often placed in orphanages because of their facial defects, are ineligible for adoption until they have at least had the lip repair. Many of these children will die of malnutrition and poor access to adequate care. The need for appropriate surgical treatment for these children is so great, and the rewards are immeasurable. The children we served on this mission were forever changed, and the values I learned from being a part of it will last my lifetime. Thank you to the American Academy of Otolaryngology—Head and Neck Surgery Foundation Humanitarian Efforts Committee for making this trip possible for me. To learn more about resident travel grants, contact humanitarian@entnet.org.
Abby R. Nolder, MD PGY-5 resident, University of Arkansas for Medical Sciences, Department of Otolaryngology—Head and Neck Surgery
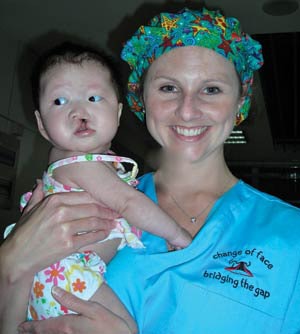 Abby Nolder, MD, and patient.
Abby Nolder, MD, and patient.In July 2010, I joined a group of nine dedicated physicians, nurses, and coworkers on a cleft-lip and palate surgical mission to Hangzhou, China. The team was led by Lisa M. Buckmiller, MD, director of the vascular anomalies center of excellence and the cleft lip and palate team at Arkansas Children’s Hospital in Little Rock, AR.
Dr. Buckmiller has taken part in and led many international surgical missions to China, Africa, and Central America. She is very involved in the pediatric otolaryngology and cleft fellowship program at Arkansas Children’s Hospital. One of her former fellows, Robert Glade, MD, now a pediatric otolaryngologist and cleft surgeon at Oklahoma University Medical Center in Oklahoma City, OK, was part of the team as well.
In cooperation with the Operation Smile Charity Hospital, Hangzhou, our Change of Face Mission Team provided cleft lip and/or cleft palate surgeries for 20 Chinese children. Many of the children were residents of the Starfish Foster Home, a special place founded by a South African school teacher, Amanda de Lange, to save the lives of Chinese orphans with special health needs.
Some of the children and their caretakers traveled more than 50 hours by train in the sweltering summer heat to reach the hospital. The tireless work and dedication shown by Amanda and her volunteers was a true testament to their commitment to providing these children with a better life. This made our contribution even more rewarding.
The Operation Smile Charity Hospital was well-equipped with two operating suites as well as a pre- and postoperative patient ward with 24-hour nursing care. We worked closely with the Operation Smile surgeons in evaluating the patients preoperatively to determine the appropriate procedure and timing for each patient.
The operating room staff was skillful and efficient. The surgeries went smoothly, and the transformations were amazing. Our team provided the children with medications, diapers, arm restraints (“no-no’s”) and feeders, all much-needed supplies for the long trip back to the foster home.
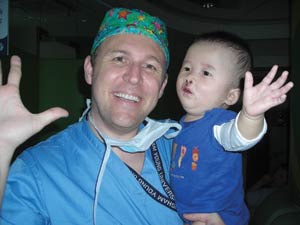 Robert Glade, MD, and patient.
Robert Glade, MD, and patient.In China, one in 600 children is born with a cleft deformity. These children, often placed in orphanages because of their facial defects, are ineligible for adoption until they have at least had the lip repair. Many of these children will die of malnutrition and poor access to adequate care. The need for appropriate surgical treatment for these children is so great, and the rewards are immeasurable. The children we served on this mission were forever changed, and the values I learned from being a part of it will last my lifetime.
Thank you to the American Academy of Otolaryngology—Head and Neck Surgery Foundation Humanitarian Efforts Committee for making this trip possible for me. To learn more about resident travel grants, contact humanitarian@entnet.org.







