Pearls from Your Peers | Pediatric Tonsillectomy: Optimizing Pain Control and Minimizing Perioperative Risk
Pediatric tonsillectomy is a very common procedure with over 500,000 procedures performed in pediatric patients every year.

In some patients, postoperative pain can be severe and require opioid medications. Inadequate pain control can lead to dehydration requiring IV fluids. The need for urgent or emergent control of oropharyngeal hemorrhage can be anxiety-provoking for both patients and parents. The Department of Pediatric Otolaryngology at Nationwide Children’s Hospital in Columbus, Ohio, led by Kris R. Jatana, MD, professor and director of Clinical Outcomes for the Surgical Services, approached these challenges from a quality improvement perspective. I sat down with Dr. Jatana to get a better sense of the efforts made and progress.
How are you balancing the goal of making sure postoperative pain is being controlled while still trying to minimize the use of opioid medications?
We initially optimized the use of nonopioid medications as first-line therapy. We developed a visual pain tracking form for use of nonsteroidal anti-inflammatory drugs and acetaminophen, including maximal weight-based dosing and frequency on discharge instructions. For patients admitted overnight or monitored in our short-term observation unit—if they did not require an opioid dose during this period—they were not sent home with a prescription. For ambulatory surgery center patients, opioids were considered on a case-by-case basis by the surgeon.
One key driver was the ability to e-prescribe opioids, which allowed us to avoid the prior inconvenient requirement of a paper script. If pain was uncontrolled, parents could call in and discuss with our team 24/7. When we launched the project, we realized our surgeon-prescribing practices were quite variable. When prescribed, we now give an average of 14 doses.
Prior to prescribing, we utilize a written opioid consent that discusses the side effects, risk of addiction, proper storage, and disposal. This consent is signed by the parent or legal guardian, and one copy is given to them, with the other placed in the patient’s chart.
What efforts have been made to decrease post-tonsillectomy hemorrhage?
In parallel, our department has tracked return to the operating room (OR) for control of post-tonsillectomy hemorrhage cases. As we utilized more ibuprofen to reduce opioid prescriptions, we saw our hemorrhage rate increase. We then incorporated the use of a new celecoxib protocol (no platelet dysfunction) instead of ibuprofen that includes a pre-prescribing discussion with families of its off-label use.
While postoperative pain control is an off-label indication for celecoxib, the medication has long been used for pain control in juvenile rheumatoid arthritis in pediatric patients and is FDA-approved over the age of two for that indication. In addition to the celecoxib protocol, our surgeons now offer both total and intracapsular tonsillectomy techniques when appropriate.
Our group worked collaboratively to educate surgeons who had not previously utilized the intracapsular technique, and utilization of intracapsular tonsillectomy has increased. As another risk-reduction strategy, we worked with our hematology colleagues to develop a focused and standardized preoperative bleeding risk assessment tool that is only six questions. If an elevated preoperative risk is identified with this instrument, a hematology evaluation is completed prior to surgery.
Let’s talk numbers. What sort of impact has the group seen since initiating these efforts?
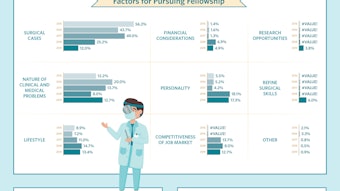
We went from about 90% of patients getting an opioid prescription in 2016 to 11% in 2021. When prescribed, the number of doses has been reduced by >50%. In addition, our group has reduced the operative control of hemorrhage rate by >60% since implementation.
In 2020-2021, by implementing these interventions in the context of our surgical volumes, we have prevented 91 children from returning to OR for control of hemorrhage. We have also reduced nonoperative readmissions and emergency room and urgent care visits for post-tonsillectomy complications by >50%. In the days of value-based care and continued commitment to quality patient care, these efforts have enhanced the quality and safety of one of the most frequently performed procedures on our pediatric patients.











![Getty Images 1013668346 [converted] 01](https://img.ascendmedia.com/files/base/ascend/hh/image/2022/03/GettyImages_1013668346__Converted__01.6244bdb1d9995.png?auto=format%2Ccompress&fit=crop&h=191&q=70&w=340)

