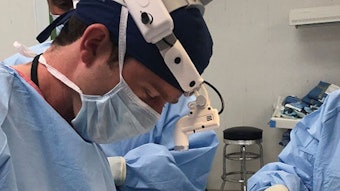
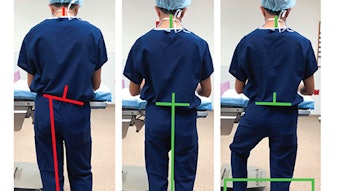
UK simulation-based otolaryngology-head and neck surgery “Boot Camp”
Medical training has shifted over recent years to a focus on developing trainee competence and proficiency according to predetermined approved standards. A challenge has been to deliver this training paradigm within a time-restricted program, which has had a significant impact, especially on surgical specialities where developing expertise relies heavily on appropriate clinical exposure.
International Guest of Honor SERIES, (I of IV): The UNITED KINGDOM

R. Anmolsingh, Department of Otolaryngology-Head and Neck Surgery, Wrightington, Wigan and Leigh NHS Foundation Trust, United Kingdom;
O. Mirza, Department of Otolaryngology-Head and Neck Surgery, Machester NHS Foundation Trust;
B.N. Kumar, President-elect, ENT UK
Medical training has shifted over recent years to a focus on developing trainee competence and proficiency according to predetermined approved standards. A challenge has been to deliver this training paradigm within a time-restricted program, which has had a significant impact, especially on surgical specialities where developing expertise relies heavily on appropriate clinical exposure. As such, a greater need to maximize learning, develop acquired competences, and accelerate skills acquisition in order to meet the educational needs of otolaryngology trainees has been identified. Correspondingly, higher surgical training curricula have adapted to incorporate alternate educational modalities, such as simulation, in order to meet this need.
Simulation-based training, a form of experiential learning, is not a new concept. It provides realistic “clinical exposure equivalent” situations that allow deliberate practice in order to achieve expertise in a non-threatening, controlled environment. High-fidelity training platforms are used extensively within the aviation industry and have contributed greatly to advances in airline safety through helping to train pilots to manage specific flight conditions and potential scenarios. There are obvious parallels to the medical sphere, where there is a need to train future clinicians without jeopardizing patient care and maintaining safety. There are several established methods of surgical training that incorporate simulation, including verbal simulation (role play), anatomical models, and virtual/computer-based patients. Simulation has the ability to track trainee progress and allow objective assessment of performance while enhancing the learning process by incorporating feedback and reflection and reinforcing positive behaviors and identifying negative actions.
Otolaryngology-head and neck surgical emergencies encompass a wide spectrum of pathologies that can be time sensitive, and if not recognized early and managed appropriately, can be potentially life-threatening. The prospect of managing these patients may be daunting for junior trainees who may have limited prior emergency exposure and who are expecting to make the transition into higher specialty training and lead the management of these conditions in a more senior role. Ideally, trainees should be given the opportunity to learn about specific emergencies and practice common emergency procedural skills before encountering the real clinical situation. The term “boot camp” is derived from a military concept of intensive, focused training to prepare new recruits and has been applied to surgical training with a similar aim over recent years. The North American otolaryngology-head and neck surgical boot camp has been established with great success since 2011. The UK ENT boot camp came into fruition in 2015, and similarly aims to provide a comprehensive and standardized level of training to all newly appointed higher specialty trainees entering otolaryngology, covering the whole spectrum of emergency clinical presentations and acute procedural skills.
The boot camp is a practical, simulation-based course held over a two-day period and comprising of several stations mapped to the otolaryngology curriculum through which candidates rotate. Each station incorporates either actor patients, mannequins, or cadaveric models and is manned by faculty comprising of consultant ENT surgeons and/or anaesthetists. Procedural skills stations cover flexible nasopharyngolaryngoscopy, rigid bronchoscopy/pharyngo-oesophagoscopy and foreign body retrieval, cortical mastoidectomy using a high-fidelity temporal bone simulator, and airway management using nonsurgical/surgical methods. Human factors training is incorporated into an immersive station mimicking a busy operating theatre environment, and a high-
fidelity interactive mannequin is used to run an acute airway emergency scenario. A series of immersive, simulated “ward round” scenarios allow candidates to lead a junior team in the assessment and management of patients presenting with acute pathology. Candidates have the opportunity to reflect on performance at the end of each station and receive formative feedback.
Our experience of running a simulation-based ENT boot camp has been a positive one, and we believe there is a potential role within surgical training. As such, the course is now an annual fixture for new trainees. Trainee feedback has been encouraging, with increased levels of confidence and self-perceived skill reported. It is debatable how this translates into actual clinical practice, which will be an area of interest for future study.