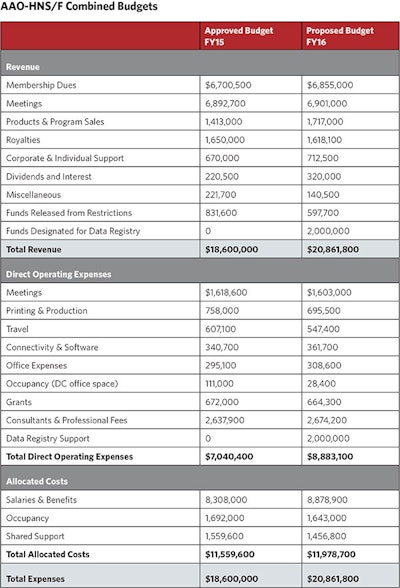
Proposed 2015-2016 (FY16) combined budget
Budgeting for FY16 represents the collaborative work of both the staff leadership and the members of the Finance and Investment Subcommittee (FISC) to develop a proposed combined AAO-HNS/F budget for the next fiscal year, July 1, 2015, through June 30, 2016 (FY16).
By Gavin Setzen, MD, Secretary-Treasurer
The FY16 budget preparation began in advance of the Boards of Directors strategic planning meeting with staff leaders reviewing their budgets to ensure that all continuing strategic items were able to be funded for FY16. The budget planning process involved each of the business units of AAO-HNS/F submitting their budgets to the financial team that worked with them to assure that revenue and expenses are in line with the mission and priorities of AAO-HNS/F. The financial team is composed of Lynn Frischkorn, director of Budgeting and Special Projects, and Carrie Hanlon, CPA, senior director of Financial Operations. The financial team presented the proposed budget to the FISC for review and approval in March.
The FISC was pleased to see that the strategic goal of identifying $600,000 of cost savings in the FY16 budget was able to be achieved. This allowed for new strategic items developed during the strategic planning meeting to be funded and incorporated into the proposed budget.
The Executive Committees (ECs) of the Boards of Directors (BODs) were presented with the FISC proposed FY16 budget and recommended endorsement for approval by the BODs. During their April meeting the BODs reviewed and conditionally approved the FY16 budget that is presented here for our membership.
In early spring, the FISC also reviewed financial results for the first six months of the FY15 budget year showing that a favorable variance, as compared to budget, is projected for the year.
Highlights of the FY16 budget
The FY16 balanced budget is being presented at $20.86 million and prioritizes the direction of the BODs. As an outcome of the strategic planning meeting the BODs approved up to $3 million of reserves to be used for the implementation of a new data registry and incorporated $2 million into the FY16 proposed budget for this purpose. This addition accounts for the majority of the difference between the FY15 and FY16 total budget.
Proposed FY16 revenue, before consideration of reserves to be used for the data registry, is composed of approximately one-third membership dues, one-third Annual Meeting revenue, and one-third other revenue. Areas where revenue is budgeted to increase include membership dues, as a result of the dues increase in calendar year 2015; product and program sales, as a result of pricing changes; and interest income, as a result of the investment of cash held for repayment of the building debt. Annual Meeting revenue from the Dallas meeting is budgeted to be consistent with the Orlando meeting even with the change to provide Instruction Courses at no additional cost. An increase in EXPO booth sales is expected to make up the shortfall in registration revenue in the first year of the Annual Meeting format change. Miscellaneous income remains largely comprised of sublease income for the lease of unused office space. Revenue from restricted funds varies from year-to-year depending on donor restrictions and timing.
The expenses for the AAO-HNS/F are separated below into two areas.
Direct Operating Expenses include costs directly related to carrying out the priorities of the strategic plan and on-going mission-related programs. Budgeted costs have been included to allow for the implementation of the new data registry; development of appropriate use criteria based on clinical indicators and guidelines; and development of a consensus on a comprehensive otolaryngology curriculum, including resources for content development.
Allocated Costs relate to staffing and benefits as well as the operating costs that are incurred for the good of the whole organization, such as occupancy and building-related expenses, and organizational-wide HR, financial, and IT costs. Increases in these costs are due to inflation, salary adjustments, and the addition of staff to support the newly approved initiatives.
The complete budget is available to any Academy Member who requests it in writing. Email requests to Carrie Hanlon, CPA, senior director, Financial Operations to bulletin@entnet.org.