- Get excited. There’s nothing like spending time with people who share your interests to re-energize and inspire you.
- Learn what works. More than 300 continuing education sessions arm you with new skills you can put into practice right away.
- Tap the minds of leaders. This is your chance to ask the best and brightest leaders in the otolaryngology community your most pressing questions.
- See and touch the latest devices. With more than 300 exhibitors in the OTO EXPOSM, participate in hands-on demonstrations and Q&A about innovative new products and technology.
- Get the exact information you need. Sessions are arranged according to tracks to provide the most beneficial information for your particular needs.
More from September 2014 - Vol. 33 No. 09

Jonathan C. Kopelovich, MD
R5 Resident Physician
University of Iowa Department of Otolaryngology Head and Neck Surgery
Quito, Ecuador
Ecuador Microtia Mission
The 19-year-old father cocked his head to the side as the entire HUGS team gathered to see the excellent results of his prior stage 1 microtia repair. Unlike many of the children who came in for their first evaluation, hair hanging over their ears and avoiding eye contact, he stood proudly, had his hair cut short on the sides, tapered and lined as if to display to the world the ear he had so recently gained. He was proud to show it to us. We were proud to see it. This year he was set to undergo elevation of his framework to create a postauricular sulcus, lined with temporoparietal fascia and skin. He stood testament to the influence our intervention has on the lives of these young Ecuadorians.
Ecuador has a population of 16 million, but for reasons not fully understood has six times the incidence of microtia, or congenital deformity of the ear, of nearby countries. Despite the incidence, these children are, per their parents’reports, castigated and made to feel awful by their peers. Microtia repair is a risky endeavor in the best of circumstances. The procedure is fraught with small, but important nuances that can make or break a result. Here, despite poor resources, we made big changes in the lives of our patients.
Our team was deep and talented. We had six senior plastic surgeons, including Mack Cheney, MD, and Tessa Hadlock, MD, from the Massachusetts Eye and Ear Infirmary (MEEI) and Vito Quatela, MD, from Rochester, NY, the founders of this mission. A dermatologist and her fellow ran their own laser hair removal clinic for returning patients. The rest of the team included two anesthesiologists, four CRNAs, nine RNs, two medical students, three facial plastics fellows, and myself. We also had two administrators, one of whom additionally conducts research on the psychosocial outcomes of microtia repair. With a modicum of planning and lots of initiative, team members fell into the roles that best suited them. I rotated from table to table to help with rib harvests and wound closures, and helped manage the floor with a team consisting of a dedicated RN and a plucky medical student.
The Ecuadorian hospital that hosted our mission had four operating rooms, two of which we occupied with our three surgical teams. An additional supply closet became the minor room—where the MEEI team churned through the myriad follow-up procedures that microtia patients require as they age. Here Dr. Hadlock narrated in English and Spanish for volunteers and patients while she operated under local using the light of her headlamp and a single mayo stand. The early part of the week was dedicated to our stage 1 repairs, while the latter half was devoted to second stage surgeries and other revisions. Our first and last days were devoted to intake and checkout respectively where we reviewed prior results and made plans for further procedures. In all, we performed more than 120 procedures.
HUGS, as an organization, is well established and well run. Now in its 14th year, this organization has been returning to serve the population of Ecuador yearly and has more recently added humanitarian trips to Guatemala, Vietnam, and soon, Peru. These elite plastic surgeons continually push each other to improve and excel in the challenging realm of auricular reconstruction. The senior members have been coming for at least a decade and have warm relationships with each other, with the Ecuadorian physicians who host us, and with many of the children they have watched grow up. I was surprised by the sophisticated level of data collection and documentation. Each child was evaluated, measured, and photographed, and their surgical experience carefully indexed. The surgical approach is constantly evolving. Tracking outcomes has helped this team immensely to refine their approach and achieve uniform results. This team does not rest on its laurels; it is growing, expanding, and improving. I am proud to have been a part of such a world-class surgical team and am grateful to the AAO-HNSF Humanitarian Efforts Committee and HUGS Foundation for co-sponsoring my trip. 
Stewart I. Adam, MD, resident, Yale-New Haven Hospital
Many physicians go into training and practice with the goal of helping patients and contributing meaningfully to society’s betterment. Perspective on the privileges and accompanying responsibilities of being a physician can sometimes be lost, especially during training, where a large body of specialty-based knowledge and surgical skills are developed in the midst of a busy clinical experience. My travel to Riobamba, Ecuador, November 8-16, 2013, helped reinvigorate a personal sense of humanitarianism as the driver of compassionate, artful care.
Our team consisted of 25 healthcare workers, including anesthesiologists, pediatricians, scrub techs, nurses, and two otolaryngologists. Howard Boey, MD, led the group for the ninth year and provided me great mentorship and training. We worked with the private charitable organization FIBUSPAM (http://www.clinicadulcerefugio.com), which was integral in providing a base in Riobamba, organizing patient recruitment, and facilitating the use of the Galapagos Military Hospital for cases requiring general anesthesia.
For a few team members, including myself, the mission was our first experience in Ecuador. Riobamba is a small Andes Mountain city in the Chimborazo Province, nestled between active volcanoes, about 125 miles south of Quito, the country’s capital city. The average household income is about $4 a day. Indigenous populations are prevalent and subsistence farming is the dominant economic activity. There is widespread poverty, unemployment, and hopelessness. Basic primary medical care is limited, and the more indigenous and impoverished people have virtually no access to surgical subspecialties such as ENT.
After taking a redeye flight to Quito and a five-hour drive through the Andes to Riobamba via military buses, we were greeted with a reception featuring indigenous music and dance at the FIBUSPAM clinic. Medical supplies were largely donated and consisted of surgical instruments/kits, medications, anesthesia equipment, microscope, NIMS machine (charitable donation from Medtronic, Inc.), food, etc. Each team member transported supplies in large hockey bags. The equipment required significant manpower in organizing, assembling, and deploying.
Our first workday was spent screening 200-plus patients at the military hospital site. Some patients traveled more than 10 hours from the Amazon basin region of Ecuador. A significant portion of patients had cleft lips, palates, and noses in various pathologies and stages of repair. Some were infants with primary lips, others returned to have their palates repaired following successful lip surgery from the previous mission. A few patients developed palate fistulas following repair, and some teenagers and young adults arrived for cleft nose surgery. Following patient screening, we planned the next four operative day schedules.
We completed 61 surgical procedures in four days. Cases included cleft lip repairs, cleft palate repairs, definitive open septo-rhinoplasty for cleft nose, thyroidectomies, tympanoplasties, a few adenotonsillectomies, and two congenital aural atresia repairs. The operative cases provided a great supplement to residency training and experience in managing cleft patients. The most meaningful part of the trip and surgical care was talking with the parents following the cases in our make-shift PACU and seeing the looks of joy, excitement, and hope on their faces.
The mission met its goals of creating accessible care to those most in need. A key factor to this successful trip was working through a well-established organization that coordinated appropriate patients for screening. The most disconcerting aspect of the care we provided is not being able to directly follow up with our patients. The FIBUSPAM clinic did arrange follow-up and we have been able to correspond with two local general surgeons and see patient photos. Working in Riobamba was enriching. I plan to participate in future medical mission trips and strongly encourage my peers to do the same. I am grateful to the AAO-HNS humanitarian grant for funding my trip. From the AAO-HNS Medical Devices and Drugs Committee
Committee Chair and Series Editor: Anand K. Devaiah, MD
Associate Professor, Departments of Otolaryngology, Neurological Surgery, and Ophthalmology
Boston University School of Medicine and Boston Medical Center
Anjum Khan, MD, MPH
Medical Officer, Division of Ophthalmic and Ear, Nose, and Throat Devices
Office of Device Evaluation, CDRH, FDA
Adjunct Clinical Associate Professor of Surgery, Uniformed Services University, Bethesda, MD
Marilyn Neder Flack, MA
Executive Director, Association for the Advancement of Medical Instrumentation (AAMI) Foundation at AAMI, Silver Spring, MD
Rahul Shah, MD, Associate Professor of Otolaryngology and Pediatrics, Children’s National Medical Center and George Washington University, Washington, DC
Member, ENT Device Advisory Panel, FDA
Introduction
As scientific and technological advances enhance the pace of medical device1 innovation, there is increasing reliance on medical devices for patient care. Otolaryngologists, who may work in settings such as outpatient, emergency, surgical, and/or nursing home care, use a wide variety of devices for diagnosis, mitigation, and treatment of medical conditions for their patients.
The inaugural article in this series for the Bulletin introduces the basic concepts of how the Food and Drug Administration (FDA) functions in regulating devices and drugs. Having a more in-depth understanding of the FDA, and how it works to ensure the safety and effectiveness of medical devices used by otolaryngologists in the above care settings is important. It enables otolaryngologists to know how they may play an active role in protecting the safety of their own patients, and in contributing to the nation’s public health related to medical devices. As discussed in this two-part article, one critical role otolaryngologists can play in assisting FDA in its mission to protect and promote the public health is that of an “active reporter”of problems they encounter with actual clinical use of medical devices.
The FDA’s Center for Devices and Radiological Health (CDRH) is responsible for reviewing pre-market applications for medical devices to ensure the devices meet the regulatory requirement of a reasonable assurance of safety and effectiveness. CDRH utilizes both pre-market programs to review device information prior to permitting manufacturers to legally market medical devices and post-market programs to perform surveillance of device performance once it is in widespread clinical use. It also has research, compliance, and educational components that round out the center’s efforts to protect and promote the public health with respect to medical devices. The focus of this article is on the pre-market and post-market work conducted by CDRH, and how otolaryngologists can contribute to ensuring and optimizing medical device safety for their patients.
CDRH Pre-market Activities
Medical devices vary greatly in the complexity of their technology. A device may be as simple as a tongue blade or as technologically complex and sophisticated as a fully implantable hearing aid or cochlear implant.
In 1976, the Medical Device Amendments to the Federal Food, Drug, and Cosmetic Act acknowledged and accommodated for the differences in complexity and level of safety of the myriad medical devices by creating a three-tiered, risk-based classification. The level of regulatory oversight for each device type is based on the classification level (Class I, II, or III) into which it is assigned.
Class I devices pose a low-to-moderate risk for causing patient or user injury and have minimal potential for harm. Examples of otolaryngologic devices in this category include tuning forks, tongue blades, and most air-conduction hearing aids. Most of these items are, in fact, exempt from pre-market review by FDA. They are still required to comply with certain general regulatory controls such as good manufacturing practices, provisions regarding adulteration and misbranding, reporting of certain types of post-market problems, and others to provide reasonable assurance of the device’s safety and effectiveness. Safety and effectiveness of these devices are generally well understood and they constitute about 47 percent of all devices in the marketplace.2
Class II devices typically pose moderate to high risks for patient or user injury and are generally more complex than Class I devices. General controls alone are insufficient to provide a reasonable assurance of their safety and effectiveness. Most require thorough review of a Pre-Market Notification [also known as a “510(k)”] to demonstrate that the device is “substantially equivalent”to a legally marketed “predicate”device. Most 510(k) submissions do not require clinical data if bench/animal data are sufficient to show substantial equivalence (SE) to a predicate device(s). A device is substantially equivalent if, in comparison to a predicate it:
Has the same intended use as the predicate; and
Has the same technological characteristics as the predicate; or
Has the same intended use as the predicate; and
Has different technological characteristics and the information submitted to FDA in the 510(k):
Does not raise different questions of safety and effectiveness; and
Demonstrates that the device is at least as safe and effective as the legally marketed device.3
Thus, a new device may be different from its predicate in composition or technological characteristics and may still claim SE as long as: 1. the new device does not have a new intended use, 2. the new device raises no different questions of safety and effectiveness, and 3. adequate performance data are provided to support the safety and effectiveness of the changes compared to the predicate. For example, when a company marketing endoscopes (e.g., laparoscopes, laryngoscopes, and cystoscopes) makes changes to design or materials of the scopes, but the function and the indications for use of the scopes remain similar to a previous generation of the scopes, marketing clearance may be granted without the manufacturer submitting clinical data with the new device, although relevant preclinical bench performance testing would likely be required. Almost 43 percent of all medical devices currently in the marketplace are reviewed through the 510(k) pre-market notification (PMN) program.4
Otolaryngologic devices in this Class II category include endoscopes, PORPS/TORPS, tinnitus maskers, radiofrequency tonsillectomy devices, and tracheo-esophageal prostheses. As noted above, Class II devices, in additional to the general controls required for Class I devices, have additional data requirements. These typically include submission of a 510(k) and special controls (e.g., specified performance testing, clinical testing, specific information in physician and/or patient labeling) to ensure a reasonable assurance of safety and effectiveness. For example, performance testing for audiometers requires compliance with American National Standard Institute S3.6-1996, “Specification for Audiometers.”
Class III devices pose the highest risk for patients or users and include devices that support or sustain human life, are of substantial importance in preventing impairment of human health, or present a potential unreasonable risk of illness or injury. The safety and effectiveness profiles of these types of devices are typically not well understood, such that special controls cannot be established to provide a reasonable assurance of safety and effectiveness (as for Class II devices). In this case, the safety and effectiveness of the device is evaluated through review of a Premarket Approval (PMA) application. The manufacturer must receive FDA approval of its PMA application prior to marketing the device. Approval of the application is based on a determination by FDA that the PMA contains sufficient information, which usually includes data from a well-designed clinical trial, to provide a reasonable assurance of safety and effectiveness of the device for its intended use(s). Examples of devices in this classification include implantable vagus nerve stimulators, cochlear implants, and auditory brain stem implants. Only about 10 percent of all devices in the marketplace have required review under this program.5
Sources
1. Medical Device Definition as defined in section 201(h) of the Food, Drug, and Cosmetic Act: A medical device diagnoses, cures, mitigates, treats, or prevents a disease /condition or affects the function or structure of the body and does not achieve Intended Use through chemical action and is not metabolized (Source: http://www.gpo.gov/fdsys/pkg/USCODE-2010-title21/pdf/USCODE-2010-title21-chap9-subchapII-sec321.pdf see page 5) (Last accessed on 11-26-13).
2. Classification of Devices http://www.fda.gov/MedicalDevices/ResourcesforYou/Consumers/ucm142523.htm (Last accessed on 11-25-13).
3. Premarket Notification (510k)> How to Find a Predicate Device www.fda.gov/MedicalDevices/DeviceRegulationandGuidance/HowtoMarketYourDevice/PremarketSubmissions/PremarketNotification510k/default.htm (Last accessed on 11-25-13)
4., 5. http://www.fda.gov/MedicalDevices/ResourcesforYou/Consumers/ucm142523.htm (Last accessed on 11-25-13) Liana Puscas, MD
Chair, AAO-HNS Delegation to the AMA House of Delegates
The American Medical Association (AMA) conducted its annual House of Delegates (HOD) meeting in Chicago, Illinois, from June 7-11, 2014. At the meeting, the AAO-HNS was represented by Liana Puscas, MD, MHS, delegation chair; Delegates Michael Goldrich, MD, and Shannon Pryor, MD; and Alternate Delegates Robert Puchalski, MD, and Academy EVP/CEO David R. Nielsen, MD. Joy Trimmer, JD, senior director of Government Affairs, and Danielle Jarchow, JD, health policy analyst provided staff support for the Delegation and OTO Section Council.
Among the many items of business on the agenda affecting the general House of Medicine, the following issues are highlighted due to their potential influence on members of our Academy.
Guidelines for Medical Healthcare Teams. The AMA’s Council on Medical Service presented its report regarding model healthcare teams and clearly delineated physician leadership of healthcare teams.
Grace Periods under the ACA. Under the Affordable Care Act, patients enrolled in federal plans have a 90-day grace period for paying their premiums. During this time, care provided by a physician would not be covered if the patient does not pay the premiums that are in arrears. The AMA passed policy favoring advocacy in support of insurance company notifications of a patient’s grace period status upon eligibility verification by the physician.
Health Insurance Formulary Transparency. The AMA supports legislation or regulation that ensures private health insurance carriers declare their formularies by October 1 of the preceding year. This would include information regarding generic versus trade formulations, copay responsibilities, and the inability to change a medication to a higher tier within the policy term.
FDA Regulation of All Nicotine Products. The AMA passed resolutions opposing any FDA rule that exempts any nicotine-containing products, including e-cigarettes and cigars, from FDA regulation.
Super Magnetic Toys. The AMA passed a resolution asking for a ban of neodymium magnetics whose magnetic strength index is greater than a certain threshold due to gastrointestinal and choking hazards produced by such toys.
Restrictive Covenants. The AMA adopted a report opining that competition among physicians is ethically justifiable when based on factors such as quality of services, skill, experience, and conveniences offered to patients. Covenants aimed to reduce competition can disrupt continuity of care and limit access to care.
Hospital Policies on Interactions with Industry. The HOD adopted a report by the Board of Trustees that encourages hospitals to craft policies concerning the relationships and interactions between hospital personnel and industry representatives within the hospital setting.
Place of Service Code for Observation Services. In alignment with the Academy, the AMA continues to support advocacy with CMS to modify the rules that govern observation versus inpatient status. Many patients admitted for observation require the same level of care as those who are formally classified as inpatients, especially when that length of stay extends beyond a 24-hour period. Patients are often liable for services provided as part of observation care, and reimbursement is lower for observation status patients than inpatient status patients, even if the services provided by the physician are identical.
Sunshine Act. The AMA website is prominently featuring information and guidelines for physicians during the tiered implementation of this Act.
The next meeting of the AMA HOD is scheduled for November 8-11 in Dallas, Texas. As a reminder, since AMA delegations are in proportion to an organization’s number of AMA members, it is imperative that we continue to grow our AMA membership to maintain otolaryngology’s representation in the HOD.
With questions regarding this report and other AMA House of Delegates activities, please email govtaffairs@entnet.org. 
With the AAO-HNSF 2014 Annual Meeting & OTO EXPOSM only days away, now is the time to learn more about the legislative advocacy-related programming available at this year’s meeting. An exciting development for this year is the availability of a second Legislative Advocacy booth, which will provide attendees with greater access to information regarding the Academy’s legislative, political, and grassroots programs. Visit one (or both) of the booths to meet the Government Affairs team and learn more about our various programs. The booths will be easily accessible in the Orlando Convention Center on either the West Concourse Level 2 or outside Hall B.
Be sure to visit to:
Sign our petition to Congress on a key AAO-HNS legislative issue and receive updates on bills affecting your practice and your patients.
Join the ENT Advocacy Network to receive timely updates on political and legislative issues affecting the specialty and a free subscription to a biweekly e-Newsletter, The ENT Advocate.
Volunteer to be a “state tracker”for the specialty.
Learn how to get involved in the grassroots “I-GO”program.
Obtain information on becoming a 2014 ENT PAC Investor*.
See which training program is leading in the Resident and Fellow-in-Training Advocacy Involvement Campaign.
To recognize our 2014 Investors, the ENT PAC Board of Advisors and staff have also scheduled various events during the meeting. Please mark your calendars to join these events.
The annual ENT PAC Investors “thank-you”reception. This popular event is scheduled to take place from 7:00 to 8:30 pm Monday, September 22, at BB King’s Blues Club. U.S. AAO-HNS members who make donations to ENT PAC prior to, or during, the meeting are invited to the event.
A special “thank-you”luncheon for members of the ENT PAC Chairman’s Club ($1,000+ donors) and winners of the 2013 SRF Advocacy Involvement Campaign. The luncheon, hosted by the ENT PAC Board of Advisors, is a unique opportunity to learn about the Academy’s political strategy and decision-making process while also networking with fellow colleagues. The year’s luncheon will take place from 11:30 am to 1:00 pm on Monday, September 22.
For more information on any of the above-listed programs, email govtaffairs@entnet.org or visit www.entnet.org/advocacy. We look forward to seeing you in Orlando!
*Contributions to ENT PAC are not deductible as charitable contributions for federal income tax purposes. Contributions are voluntary, and all members of the American Academy of Otolaryngology-Head and Neck Surgery have the right to refuse to contribute without reprisal. Federal law prohibits ENT PAC from accepting contributions from foreign nationals. By law, if your contributions are made using a personal check or credit card, ENT PAC may use your contribution only to support candidates in federal elections. All corporate contributions to ENT PAC will be used for educational and administrative fees of ENT PAC, and other activities permissible under federal law. Federal law requires ENT PAC to use its best efforts to collect and report the name, mailing address, occupation, and the name of the employer of individuals whose contributions exceed $200 in a calendar year. From time to time, Education staff receives calls from members regarding aspects of the Foundation’s Education Program. With the launch of the new AcademyU®, www.entnet.org, and ENTConnect, member attention has provided fresh opportunity to address these concerns and questions.
Myth 1—CPD is the Same as CME
Continuing medical education (CME) is the component of continuing professional development (CPD) that offers education credit for physicians. CPD encompasses a larger view of professional development focused on addressing the education needs of all healthcare professionals. CPD goes beyond just providing credit and explores the critical education needs of all ENT professionals.
Myth 2—AAO-HNSF Oversees Maintenance of Certification (MOC)
The Academy is not in charge of MOC.
The American Board of Otolaryngology (ABO), as a part of the American Board of Medical Specialties, oversees the program. Information about MOC can be found on ABO’s website. However, the Foundation is continuously adding to its resources that aid in the MOC process. These include the AcademyQ™question app, live and recorded Clinical Fundamentals courses, and the updated “Otolaryngology Lifelong Learning Manual”out this fall.
Myth 3—AAO-HNSF Produces ENT e-Pimp
ENT e-Pimp is not a Foundation education product, but we do have a robust set of study questions in the AcademyQ™app. An additional 400 questions and a version of the app for Android users will be available this year.
Myth 4—With PMP Going Away, AAO-HNSF Will No Longer Have Case-based Education
While Patient Management Perspectives has been retired, it is the Foundation’s intention to offer a dynamic set of case-based courses available for multiple platforms that will meet the members’wishes for interactive and engaging learning.
Myth 5—The Foundation Provides Certificates for Its Education Activities
We do not provide certificates for individual activities. The only exception is the Annual Meeting & OTO EXPOSM. Instead, we provide everyone who has participated in a Foundation education activity an annual transcript listing activities and total credit awarded. In the future, transcripts will be replaced with 24/7 access to individual credit records through ENTConnect. It is important that every member has a profile in the member portal. 
Dunia Abdul-Aziz, MD
Paul Konowitz, MD
Madeline Randolph, BS
Jackson Randolph, BS
Dipti Kamani MD
Gregory W. Randolph, MD
In January 2014, a surgical team from the Massachusetts Eye and Ear Infirmary, Boston, composed of American Academy of Otolaryngology—Head and Neck Surgery members Gregory W. Randolph, MD, Paul Konowitz, MD, Dipti V. Kamani, MD, and Dunia Abdul-Aziz, MD, teamed up with ENT surgeons from across India at the Neeti clinic in Chikhaldara, a remote mountain hospital in the outskirts of Nagpur, Maharashtra, India.
Surgical assistants included Madeline Randolph, a student at Providence College, and Jackson Randolph, a student recently graduated from Cornell University. Together, they embarked on an intense three-day effort not only to care for patients with goiter and thyroid disease, but also to educate junior Indian ENT surgeons on thyroid surgical technique, including neural monitoring, through hands-on experience, interactive video surgical conferencing, and formal lectures.
This effort marked the 13th annual thyroid surgical workshop, a surgical camp and educational tour de force sponsored by the Rotary Club of Nagpur South and inspired and led by Madan Kapre, FRCS, DLO, a Rotarian and senior ENT surgeon in Nagpur.
More than a decade ago, Dr. Kapre left his position as senior consultant in the U.K., where he had received much of his surgical training, to return home to India. He sought to facilitate access to high quality medical and surgical care across India, including rural areas. In addition, he had a goal of mentoring and educating junior ENTs in the art of thyroid surgery and the nuances of surgical decision-making.
In this spirit, the Neeti clinic was created—combining Dr. Kapre’s passion for service and education. Annual surgical camps were coordinated with the support of the Rotary Club members. Senior surgeons from across India volunteered at the annual surgical camp to perform thyroidectomies and other surgeries. As each surgery took place, an intense training session was carried out simultaneously in an adjacent room as workshop attendants observed the case via streaming video.
By 2014, the clinic has evolved into a stand-alone rural hospital, with two communal inpatient wards, a two-table operating room equipped with general anesthesia capacity, a pharmacy, laboratory, and full-time medical physician and nursing support. The clinic manages the perioperative care—from pre-operative evaluation to post-surgical recovery—of all patients.
Affiliation with nearby larger hospitals establishes a safety measure for patients who may require higher acuity care. In addition to the thyroid surgical camp, the hospital hosts general surgeons, orthopedic surgeons, and ophthalmologists in similar camps addressing the medical needs of the Melghat tribal communities.
We arrived to the Neeti clinic in the evening of January 12, 2014, after an uphill journey from Nagpur to Chikhaldara. Pre-operative evaluation of each patient had already been completed by the onsite physicians and Dr. Kapre’s medical team, including his wife, an anesthesiologist, and his two daughters and their husbands, who are otolaryngologists in India (Figure 1). Pre-operative ultrasound and fine-needle aspiration results had been obtained. Anesthesia risks, anemia, pregnancy, and thyroid dysfunction were obtained prior to surgery. The patients were slotted for surgery during the next two days.
The start of surgery was marked by a team gathering outside the operating theater with a prayer to lord Ganesha for successful execution of the surgical camp without any obstacles. An excellent surgical team ensured the two-bed operating room ran smoothly (Figure 2). We worked side by side, and took turns with the other Indian ENT surgeons in performing the surgeries (Figure 3).
The procedures were video conferenced to the hall upstairs where 40 ENT surgeons, who had made the journey from across India and as far as United Arab Emirates, were walked through the key teaching points of the procedure. Along the way, the salient aspects of management of thyroid disease were addressed both formally and informally through questions. What is the role of intraoperative nerve monitoring? How should one approach the parathyroid glands during thyroidectomy?
The surgical decision making—whom to operate on and what surgery to perform—required tailoring to this particular clinical and geographic setting. Given the limited access to medical care, performing total thyroidectomies, which would commit patients to lifelong daily thyroid replacement and risk need for calcium supplementation, was limited to special clinical circumstances (papillary thyroid carcinoma in a patient for whom access to medicine was ensured). For goiter disease, surgical planning entailed preservation of residual thyroid tissue to minimize the potential for hypothyroidism.
We introduced the intraoperative nerve monitoring (IONM) technology, pioneered at Mass Eye and Ear, and demonstrated its utility as an adjunct to anatomic identification and preservation of the nerve and as a tool for the initial nerve identification and tracing. We demonstrated the approach to troubleshooting intra-operative loss of signal. Equipment for monitoring was obtained through a grant from Medtronic and was brought from Boston to Nagpur. Nerve monitoring was easily assimilated into the workflow of the procedure and the workshop attendants acquired this skill.
In addition to the delegation from Mass Eye and Ear, senior surgeons and educators from across India took turns to operate and lead the workshop discussion, including: Dr. Kapre; Alok Thakar, MS, FRCSEd, from the All-India Institute of Medical Sciences (AIIMS), Delhi; Jyoti Dabhalkar, MS (ENT), DLO, from King Edwards Memorial (KEM) Hospital, Mumbai; Murad Lala, MD, from Hinduja Hospital, Mumbai; Ashish Varghese, MD, of Christian Medical College, Ludhiana; and Vikram Kekatpure, MD, from Mazumdar-Shaw Cancer Center, Bangalore (Figure 4).
As cases were being performed in the operating room, attendants viewed the procedures in an adjacent room, stimulating active discussion about anatomic landmarks and the appropriate surgical maneuvers of each case. Through video conferencing, surgical knowledge, skills, and techniques could be disseminated across a wide spectrum of practicing surgeons in the communities from across India. Beyond a surgical mission, this workshop was educational, hoping to empower clinicians with expertise in the challenges of thyroid disease.
At the completion of two operative days, the group travelled back to Nagpur for the annual thyroid Continuing Medical Education (CME) conference at The Radisson, Nagpur (Figure 5). Building on the expertise of Dr. Randolph, the course had a special focus on the utility of intraoperative nerve monitoring, stimulating interest in the applicability and potential value of incorporating this new technology into general practice in India.
At the conclusion of the workshop, 12 thyroidectomies had been successfully performed for indications of large multinodular goiter with compression symptoms and for papillary thyroid carcinoma. Beyond this, 40 workshop attendants left with a nuanced understanding of the surgical management of thyroid disease.
The philosophy of this mission is encompassed by the Chinese proverb: “Give a man a fish and you feed him for a day; teach a man to fish and you feed him for a lifetime.”Beyond the patients and families who were directly influenced by the procedures, there was an equally profound emphasis on surgical education from national and global leaders in the field.
These younger surgeons, equipped with the new knowledge and expertise, are the vital link in bridging the medical gap that exists across rural and urban areas, in and outside of India. The surgical camp and conference serves as a “meeting of the minds”—as a vehicle for dissemination of information and surgical know-how—carried out in a concentrated setting. This arrangement can serve as a model for global surgical education, inspiring efforts to advance beyond medical missions in which foreign surgeons operate and depart.
In the end, our experience, operatively and beyond, was intensely moving and inspiring. Camaraderie among the participants of the mission was fast to form, growing from a shared commitment to excellence and safety. Out of one week grew a fellowship with the local Melghat community, ENT attendants, and Rotarians that we hope will flourish with time. David L. Steward, MD
Member of the Endocrine Surgery Committee
September is national Thyroid Cancer Awareness Month, which coincides with our AAO-HNSF Annual Meeting & OTO EXPOSM, September 21-24 in Orlando, FL. The AAO-HNSF plans to highlight thyroid cancer awareness in several ways. The Endocrine Surgery and Program Advisory committees have worked together to designate specific endocrine sections at the meeting.
This will include a hands-on, all-day ACS Ultrasound Course: Thyroid and Parathyroid Ultrasound Skills-Oriented Course on Saturday, September 20, as well as numerous oral and poster presentations, instruction courses, and four miniseminars.
The incidence of thyroid cancer is rapidly rising nationally and abroad and is projected to be the second most common cause of cancer in women by 2020. The cause for the rapid growth remains unknown, but is likely multifactorial and related to improved detection, environmental factors, and increasing lifespan.
Our understanding of the molecular basis of thyroid cancer is swiftly advancing, which has led to improvements in the management of patients with nodular thyroid disease. The recently completed NIH-sponsored papillary thyroid cancer genome project is expected to move from bench to bedside within a few years, an unprecedentedly short timeframe.
Attend the AAO-HNSF Annual Meeting & OTO EXPOSM in Orlando during September, Thyroid Cancer Awareness month, and learn about the advances in this field. On July 3, the Centers for Medicare & Medicaid Services (CMS) posted the proposed Medicare physician fee schedule (MPFS) for calendar year (CY) 2015. Key provisions of the MPFS affecting otolaryngologists, include, but are not limited to, ENT services captured by the CMS misvalued codes screen, CMS’proposal to phase out 010 and 090 globals and convert all codes to 000, and the expansion of clinical quality measures available to ENTs for quality reporting. The Academy submitted comments to CMS on the proposed rule on September 2. The Academy also developed a member summary, which goes into greater detail of all of the important proposed requirements. The summary can be accessed on the Academy’s Regulatory Advocacy page at http://www.entnet.org/content/regulatory-advocacy. Some of the key provisions Members should be aware of from the proposed rule include:
Medicare Sustainable Growth Rate (SGR)
Within the proposed rule, CMS projects that the Conversion Factor (CF) for the first three months of CY 2015 will be $35.7977 (compared to the 2014 conversion factor of $35.8228). This estimate is based on a zero percent update (through March 31, 2015), as provided under the Protecting Access to Medicare Act of 2014 (PAMA) and the adjustments necessary to maintain budget neutrality for the policies in this proposed rule. CMS applies this CF to all of CY 2015 for purposes of completing its regulatory impact analysis. However, absent further Congressional action, a Medicare Sustainable Growth Rate (SGR)-induced reduction of more than 20 percent would occur on April 1, 2015.
Potentially Misvalued Services
As members know, CMS and the AMA Relative Update Committee (RUC) have taken increasingly significant stepsto address potentially misvalued codes. Under the ACA, the Secretary of HHS is directed to examine misvalued services in the seven key categories, including: 1. Codes and families of codes for which there has been the fastest growth; 2. Codes or families of codes that have experienced substantial changes in practice expenses; 3. Codes that are recently established for new technologies or services; 4. Multiple codes that are frequently billed in conjunction with furnishing a single service; 5. Codes with low relative values, particularly those that are often billed multiple times for a single treatment; 6. Codes that have not been subject to review since the implementation of the RBRVS (the so-called ‘Harvard-valued codes’); and 7. Other codes determined to be appropriate by the Secretary.
In addition to the Secretary having the authority to identify potentially misvalued codes, the public also is able to nominate codes as potentially misvalued. During the 2014 notice and comment periods, the Academy nominated CPT 41530 (Submucosal ablation of the tongue base, radiofrequency, 1 or more sites, per session) as misvalued. This assertion came after receiving feedback from Members, experts of the Sleep Committee, and other stakeholders that two of the practice expense inputs for the code were outdated and required refinement based on current pricing and technology used. As such, CPT 41530 was identified within the 2015 proposed rule as being potentially misvalued.
Not only was CPT 41530 identified, but CMS also identified 10 additional potentially misvalued codes relevant to otolaryngology, using a new screening process that targets codes the usual identification process overlooks. According to CMS, the traditional identification process may miss certain services because the specialty that typically furnishes the service does not have high volume relative to the overall PFS utilization. In response to this gap in the identification, CMS proposes to identify the Top 20 codes by specialty in terms of allowed charges that have not been reviewed since CY 2009. For otolaryngology, CMS identified the following as potentially misvalued using this new screen:
11100 Biopsy skin lesion
11101 Biopsy skin add-on
14060 Tis trnfr e/n/e/l 10 sq cm/< 31575 Diagnostic laryngoscopy
31579 Diagnostic laryngoscopy
92557 Comprehensive hearing test
95004 Percut allergy skin tests
95165 Antigen therapy services
According to CMS, review of these codes is necessary to assess changes in physician work, to update direct PE inputs, and because these codes have a significant influence on PFS payment at the specialty level. For these reasons CMS believes review of the relativity of the codes is essential to ensure that the work and PE RVUs are appropriately relative within the specialty and across specialties.
Valuation of the Global Surgical Package
Also within the 2015 proposed rule is a major change to reporting global surgical procedures. CMS has proposed a two year transition of all 010 and 090 global services to a 000 global, RVUs used to develop PFS payment rates critical need to reflect the most accurate resource costs associated with PFS services. CMS does not believe that maintaining the post-operative 10-and 90-day global periods is compatible with their continued interest in using more objective data in the valuation of PFS services and accurately valuing services relative to each other. Because the typical number and level of post-operative visits during global periods may vary greatly across Medicare practitioners and beneficiaries, CMS believes continued valuation and payment of these face-to-face services as a multi-day package may skew relativity and create unwarranted payment disparities within PFS payment. CMS also believes that the resource-based valuation of individual physicians’services will continue to serve as a critical foundation for Medicare payment to physicians, whether through the current PFS or in any number of new payment models. Therefore, CMS feels it is critical that the RVUs under the PFS be based as closely and accurately as possible on the actual resources involved in furnishing the typical occurrence of specific services.
To address these issues, CMS proposes to retain global bundles for surgical services, but to refine bundles by transitioning over several years all 10- and 90-day global codes to 0-day global codes. Medically reasonable and necessary visits would be billed separately during the pre- and post-operative periods outside of the day of the surgical procedure. CMS proposes to make this transition for current 10-day global codes in CY 2017 and for the current 90-day global codes in CY 2018, pending the availability of data on which to base updated values for the global codes. CMS believes that transitioning all 10- and 90-day global codes to 0-day global codes will increase the accuracy of PFS payment by setting rates for individual services based more closely upon the typical resources used in furnishing the procedures. CMS also believes the transition will help avoid potentially duplicative or unwarranted payments, eliminate disparities between the payment for E/M services in global periods and those furnished individually, maintain the same-day packaging of pre- and post-operative physicians’services in the 0-day global, and facilitate availability of more accurate data for new payment models and quality research.
As they transition these codes, CMS acknowledges they will need to establish RVUs that reflect the change in the global period for all the codes currently valued as 10- and 90-day global surgery services. Further, if CMS adopts this proposal, they intend to monitor any changes in the utilization of E/M visits following its implementation and seeking comment on potential payment policies that will mitigate such a change in behavior.
Due to CMS’proposed timeline with this change in reporting global surgical procedures, these procedures will not be afforded the opportunity of surveying time and intensity information of each for valuation purposes. CMS believes, absent any new survey data regarding the procedures themselves, data regarding the number and level of post-service office visits can be used in conjunction with other methods of valuation to adequately determine the appropriate time and intensity information. Other valuation methods include:
Using the current potentially misvalued code process to identify and value the relatively small number of codes that represent the majority of the volume of services that are currently reported with codes with post-operative periods, and then adjusting the aggregate RVUs to account for the number of visits and using magnitude estimation to value the remaining services in the family;
Valuing one code within a family through the current valuation process and then using magnitude estimation to value the remaining services in the family; and/or
Surveying a sample of codes across all procedures to create an index that could be used to value the remaining codes.
Malpractice RVUs
CMS is required to review, and if necessary adjust, RVUs no less often than every five years. For 2015, CMS proposes to implement their third comprehensive review of malpractice (MP) RVUs. The proposed MP RVUs were calculated by a CMS contractor based on updated MP premium data obtained from state insurance rate filings. The calculation requires using information on specialty-specific MP premiums linked to a specific service based on the relative risk factors of the specialties that furnish a particular service. MP premium information is weighted geographically and by specialty to account for variations by state and specialty. CMS used three data sources: CY 2011 and 2012 premium data; 2013 Medicare payment and utilization data; and 2015 proposed work RVUs and geographic practice cost indices (GPCIs). CMS describes the steps for calculating the proposed MP RVUs to include the following: 1. compute a preliminary national average premium for each specialty, 2. determine which premium class(es) to use within each specialty, 3. calculate a risk factor for each specialty, 4. calculate malpractice RVUs for each HCPCS code, and 5. rescale for budget neutrality so that the total proposed resource-based MP RVUs equal the total current resource-based MP RVUs. CMS says that, on average, work represents about 50.9 percent of payment for a service under the PFS, PE about 44.8 percent, and MP about 4.3 percent.
Quality Reporting Initiatives
In the proposed rule, several new initiatives and requirements were brought forth for Physician Compare, the Electronic Health Records (EHR) Meaningful Use (MU) Incentive Program, Physician Quality Reporting System (PQRS), and Value Based Payment Modifier (VM). While not nearly an exhaustive list, here are a few of the important changes proposed within the various programs: 1. adding additional quality reporting participation and rankings of both individuals and group practices on Physician Compare, 2. not requiring Eligible Professional (EPs) to ensure that their CEHRT products are recertified to meet the most recent version of the electronic specification for CQMs in 2015, 3. additional proposals related to the 2017 PQRS payment adjustment, 4. inclusion of two otolaryngology-specific measures groups in the PQRS program, 5. application of the VM to all physicians, nonphysicians, and groups of physicians, regardless of group size beginning in 2017, and 6. increasing the amount of payment at risk under the VM from -2.0 percent in CY 2016 to -4.0 percent in CY 2017, which when combined with the PQRS penalty creates a total -6 percent penalty for all quality reporting.
Members are encouraged to review the more detailed summary of the proposed requirements not only for the programs highlighted above, but also for additional information and changes of other programs within the proposed rule that potentially impact our specialty. Stay informed by visiting the Academy’s Regulatory Advocacy page at http://www.entnet.org/content/advocacy. 
Alabama claims Julius N. (Buddy) Hicks, MD, as one of its own. He was born in Enterprise, AL, and became one of its most influential otolaryngologists.
Richard W. Waguespack, MD, will honor the life of the late Dr. Hicks with a Presidential Citation that specifies, “…he truly fostered our specialty’s betterment for decades.”Dr. Waguespack further cites Dr. Hicks’s encouragement and professional support in his career.
After graduating from Duke Medical School in 1953, Dr. Hicks completed an internship and six months of an otolaryngology residency program at the University of Alabama at Birmingham (UAB). He then served as a captain in the U.S. Air Force for two years.
In 1960 he completed residency in otolaryngology at Massachusetts Eye and Ear Infirmary, Boston, Massachusetts. However, it was not long (1961) before the Alabamian returned to his roots at the UAB division of otolaryngology head and neck surgery. There he continued to enhance his knowledge and skill to become professor and director in 1985.
When Dr. Hicks retired from that role in 1992, he became a professor emeritus, but did not stop advocating for patient health joining an AAO-HNS campaign that explored the effects of air pollution on health.
He is called a pioneer in his field. During his life and since his death in 2009, he has been internationally honored as a researcher, clinician, distinguished surgeon, author, teacher, society leader, and mentor of many grateful otolaryngologists. 
For much of the past 20 years, Reginald F. Baugh, MD, has worked to improve patient safety and quality care by involving himself in emerging initiatives essential to the evolution of patient care in the U.S.
According to Dr. Waguespack, speaking on this 2014 Presidential Citation, “Reggie is being honored for contributing to the advancement of patient safety and quality improvement in otolaryngology-head and neck surgery. He has demonstrated this commitment by chairing several Clinical Practice Guideline workgroups, participating in survey and database studies, while educating our membership about these topics.”
Dr. Baugh earned his medical degree and completed residency at the University of Michigan in Ann Arbor. His otolaryngic focus has centered on pediatric otolaryngology, sleep medicine, and sinus disease. He is professor of otolaryngology at the University of Toledo.
Dr. Baugh was an early adapter of the drive for patient safety and quality. His activities have included contributing to advancing the Foundation’s clinical practice guidelines program, serving as assistant chair, Benign Paroxysmal Positional Vertigo (BPPV) Guideline (November 2008); chair, Tonsillectomy Guideline (January 2011); and chair, Bell’s Palsy guideline (November 2013)
He devoted time to improving the regulatory side of care delivery providing leadership as the physician liaison from PSQI to the Ambulatory Quality Alliance (AQA), a voluntary multi-stakeholder collaborative to improve performance measurement, data aggregation, and reporting in the ambulatory care setting.
Dr. Baugh’s commitment to improved care led him to the position of frequent Otolaryngology-Head and Neck Surgery reviewer and a deeper commitment still as a member of its editorial board. He has published on more than 70 topics nationally and internationally. 
A short biography of Byron J. Bailey, MD, outlines a figure of tremendous stature and an image of a formidable icon.
Richard W. Waguespack, MD, has a more personal view of Dr. Bailey, and in his 2014 Presidential Citation, he notes two of his own descriptors, “I choose [to call him] …”friend and mentor,”for someone who has truly been my ‘professional’father, and which almost equally applies to his wife, Margi.”
Dr. Bailey graduated from and took his residency at the University of Oklahoma and its College of Medicine. He followed that with a residency in head and neck surgery from UCLA and then served four years on its faculty. From 1968 to 2003, he took a position at the University of Texas Medical Branch at Galveston as the Wiess Professor and Chair of the department of otolaryngology.
He has been involved with specialty societies from the start of his career, notably the American Academy of Otolaryngology—Head and Neck Surgery and its Foundation, serving as its 1998-1999 president. He has led many others in that capacity including the Society of University Otolaryngologists, the Texas Association of Otolaryngology Head and Neck Surgery, the Association of Academic Departments of Oto-HNS, the American Society for Head and Neck Surgery, the American Board of Otolaryngology, the American Laryngological Association, and the National Association of Physicians for the Environment.
He has accrued many honors during his career. He has received the Academy’s Jerome C. Goldstein, MD Public Service Award and the Distinguished Award for Humanitarian Efforts. 37th Annual Dinner Meeting
6:30 pm to 11:30 pm
Monday, September 22
Featured speaker: Douglas Waddell on the Affordable Care Act: What It Means for Otolaryngologists
Hyatt Regency Orlando Hotel, International Tower
Executive Board Meeting
4:30 pm to 5:45 pm Sunday, September 21
ICS Room, Orange County Convention Center
For Board Attendance: Satish.govindaraj@mountsinai.org
General Body Meeting
10:00 pm after dinner on Monday, September 22
www.aaoih.com
For Dinner Reservations: dcmehta@aol.com or call 914-953-6495
Please contact:
Ameet Singh, MD (dr.ameetsingh.ent@gmail.com) for membership application
Ashutosh Kacker, MD (kacdoc@aol.com) for more information and program details
The President and the Board of Governors of the American Association of Otolaryngologists of Indian Heritage (AAOIH) cordially invite you to attend our 37th Annual Dinner Meeting.
This year our featured guest is Douglas Waddell, director of managed care and government markets. He will address the meeting and discuss the topic of “The Affordable Care Act: What it means for otolaryngologists.” Mr. Waddell has lectured extensively on this subject around the country and has educated many physicians on this important piece of legislation.
Attendance at the meeting this year is anticipated to be large. RSVP for dinner is strongly recommended. For program details and information, please email Ashutosh Kacker, MD, at kacdoc@aol.com or visit www.aaoih.com.
Otolaryngologists of Indian Heritage who are interested in becoming AAOIH members and wish to take part in the activities of our association are recommended to email Ameet Singh, MD, at dr.ameetsingh.ent@gmail.com for details.
The president will convene the Executive Governing Board meeting of AAOIH on Sunday in the ICS room of the Convention Center to discuss the pending issue of the AAO-HNSF’s AAOIH-IVS program. Board members are urged to RSVP attendance to Satish Govindaraj, MD. The IVS issue will be finally settled in the General Body meeting.
RSVP:
For Board Attendance: Satish.govindaraj@mountsinai.org
For Dinner Reservations: dcmehta@aol.com or 914-953-6495 
Jeremy Hornibrook, MD, FRACS
In the early 19th century, the bony structure and some of the membranous structure of the inner ear were anatomically well described, but their functions unproven. A common notion was that canals were for the transmission of bone-conducted sound and for the perception of sound direction.
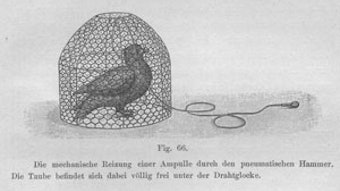
In 1824, Pierre Flourens had published the results of his research in pigeons, in which he showed that the canals were associated with eye and head movements.
Julius Ewald (1855-1921) was professor of physiology at the University of Strasbourg. His work on the inner ears of frogs, pigeons, and dogs was published in 1892, as Physiologische Untersuchungen uber das Endorgan des Nervus Octavus. Although the book is widely referred to by vestibular system investigators, few have ever seen it.
A full English translation of the book was accomplished. Unfortunately, much of the book deals with ablative experiments on pigeon inner ears, but it conveys Ewald’s ingenuity in experiment and equipment design, long before the operating microscope.
The most elegant and important findings are in Experiments 81 and 82. Selective cannulation of the canals enabled the application of positive and negative pressures. These correctly implied a direct connection between the canals and eye muscles except the lateral rectus, which was the only error.
Ewald’s important, but perfunctory description of eye movements has come to be known as Ewald’s Laws of canal function. At the time some inconsistencies were perplexing (Ewald’s Paradox) and were not explained for another 60 years by the electron microscope.
Ewald’s observations have become a quoted cornerstone of vestibular physiology and are now clinically relevant in explaining the eye movements seen in benign paroxysmal positional vertigo (BPPV). Craig Derkay, MD
Professor and Vice-Chairman Department of Otolaryngology-Head Neck Surgery
Eastern Virginia Medical School
Director, Pediatric Otolaryngology
Children’s Hospital of the King’s Daughters
I am pleased to announce that the 20th Jacobson Award for Surgical Innovation was presented to Robin T. Cotton, MD, for his seminal work in the care and reconstruction of the stenotic pediatric airway. Dr. Cotton received his award at a dinner in his honor in Chicago, IL, on June 5.
The prestigious Jacobson Innovation Award honors living surgeons who have been innovators of a new development or technique in any field of surgery and is made possible through a gift from Julius H. Jacobson II, MD, and his wife Joan. Dr. Jacobson is a general vascular surgeon known for his pioneering work in the development of microsurgery.
Dr. Cotton is the director of the Aerodigestive Center at Cincinnati Children’s Hospital, and professor, department of pediatrics, at the University of Cincinnati’s department of otolaryngology, both in Cincinnati, OH. He is the first otolaryngologist to receive this prestigious honor. Children, who were sentenced to a lifetime of breathing through a tracheotomy and having their lifestyle altered as a result, are now afforded the opportunity for reconstructive surgery and a more normal lifestyle thanks to Dr. Cotton’s pioneering work. 
In these times of change, it becomes of upmost importance that the Board of Governors (BOG) remains in touch with the day-to-day practicing otolaryngologist. One major focus of the BOG during this past year has been engaging local, state, and regional societies, non-society affiliated academy members, and independent specialty societies within otolaryngology. We have used a multi-tiered approach to reinforce these connections. Our goal has been to strengthen lines of communication on grassroots and legislative issues, help those societies that are having organizational challenges, and OTO-HNS societies, which each have a representative to the BOG.
The BOG Regional Plan is entering its third year. This idea, which emerged from the Socioeconomic and Grassroots (SEGR) Committee several years ago, has blossomed into an ever stronger vehicle with which to capture emerging socioeconomic trends and alert the BOG SEGR and pass items on to the Physician Payment Policy (3P) Workgroup. SEGR Committee Chair David Edelstein, MD, and Vice-chair Ken Yanagisawa, MD, have worked exceedingly hard to hone the process into a streamlined and efficient organization.
The regional organizational structure not only includes geographic representation, but also society representation with the addition of a representative to facilitate the commitment. The BOG section of the wonderfully revamped Academy website will direct you to the correct region matching representative.
Our local and regional societies are the lifeblood of our grassroots organization. However, many of these societies are facing immense challenges in staying vibrant and viable due to the strain of decreasing financial support, time constraints by members, increasing hospital employment, and from dormant societies that have a renewed interest, among other reasons. We receive calls and emails to help the BOG-related societies through their challenges. It became clear that we needed a more formal and streamlined approach to aid with varying needs.
A group, called Societies Connected, is being organized within the BOG, composed of BOG committee members, Academy staff, executive directors of strong state societies, and the BOG member-at-large. Although there are numerous pathways to initiate communication from the society to the Academy (through the SEGR regional rep, website inquiry, ENT Connect, direct communication with a physician leader or staff), there needs to be a go-to group of seasoned experts to help the societies who need assistance. This may entail direct advice, or just connecting the society in need with another that may have strengths to complement the challenges of the society.
The ultimate goal is simple—a solidified, organized, and detailed line of communication throughout the BOG societal organization creates empowerment and engagement. We cannot force anyone to get engaged in the important grassroots issues, but we certainly can make it appealing and straightforward. Please join us in that mission. 
In January 2015, James C. Denneny III, MD, will become the next Executive Vice President/CEO of the American Academy of Otolaryngology—Head and Neck Surgery and its Foundation following the 13-year tenure of David R. Nielsen, MD.
“I am incredibly honored and excited to join the staff at the Academy,”Dr. Denneny said. “I will do everything I can to continue the positive momentum that we have maintained over the years.”
Dr. Denneny has been devoted to the organization for years, said AAO-HNS/F President Richard W. Waguespack, MD. “He is a proven leader who has an obvious passion for the specialty and a keen understanding of the challenges facing both practitioners and patients.”
An active member since 1984, Dr. Denneny served as president of the AAO-HNS/F (2007-2008). His involvement also includes 11 years on the Boards of Directors, 22 years on the Board of Governors with a term as BOG Chairman (1998-1999), and leadership positions in many partnerships, coalitions and workgroups. He co-chairs the Academy’s Physician Payment Policy Workgroup, serves as the Coordinator for Socioeconomic Affairs and chairs the Ad Hoc Payment Model Workgroup.
Dr. Denneny’s career spans both private and academic practice. Before serving the Knoxville, TN, community for 24 years as a private practitioner, he held academic appointments in Houston and Indianapolis. In 2011, he left private practice to join the Department of Otolaryngology—Head and Neck Surgery at University of Missouri as Professor of Clinical Otolaryngology.
Born in St. Louis, Dr. Denneny grew up in Oklahoma City. After receiving a Bachelor of Science from Baylor University in Waco, TX, he earned his medical degree and did a general surgery residency at the University of Oklahoma Medical School. He completed his residency in otolaryngology-head and neck surgery at the University of Pennsylvania School of Medicine in Philadelphia. He subsequently completed a fellowship in facial plastic reconstructive surgery while teaching otolaryngology-head and neck surgery as a clinical instructor at the University of Illinois in Chicago.
“He has my unbridled enthusiasm and support as he steps into this new role,”Dr. Nielsen said. To ensure a smooth and positive transition, Dr. Nielsen and Dr. Denneny will be working closely together with the Boards of Directors and Academy staff.
“Please join me in celebrating both Dr. Denneny and Dr. Nielsen for their leadership, vision and passion for this organization and for the specialty,”Dr. Waguespack said. 
Our Annual Meeting brings us great educational content, including exceptional named lectures. These were highlighted for our Members in the July Bulletin. While I hope you will attend all of them, I’d like to emphasize one that is linked to a critical issue of which most of us are not aware. The following is edited from a report by Michael M. Paparella, MD, whose eponymous lecture this year is being given by Richard A. Chole, MD, PhD. Don’t miss it!
Virtually every hospital in the United States and worldwide has a pathology department for every field in medicine except one: ear diseases (Otology-Neurotology). Whether from OR frozen sections or autopsy studies clinical, surgical, and forensic pathology often represent the best way to understand disease or injury and their causes, helping the physician better understand how to diagnosis and treat.
Ear diseases are common in society and in otolaryngology. For example, according to NIH studies nearly 90 million Americans have dizziness and many have incapacitating Meniere’s Disease; 40 million have significant hearing losses and tinnitus. Otitis media occurs in almost every child before age 5 and chronic forms of otitis media with effusion (OME) occur in about 10 percent of children. Furthermore, many have chronic otitis media and chronic mastoiditis characterized by the development of tissue pathology, not fluid.
Considering the above, tragically there are only three active temporal bone laboratories in the United States currently receiving and preparing temporal bones for study and research analysis. There should be many more in academic and other centers. The cost to acquire, prepare, and study a single human temporal bone is about $3,000 and requires special expertise and training available only in temporal bone laboratories. For this reason, human temporal bone pathology has become a special and costly, but critical research endeavor.
Your Academy has encouraged focus on how human temporal bone pathology research will enhance your ability to diagnose and treat your patients with ear (and other) diseases. In future Bulletin articles you will learn more about otopathology and how important it is to assure a future supported by this critical foundation of research and knowledge.
What Can I Do?
Be aware of the critical need to resurrect human temporal bone research from its near demise.
Be aware of and support the National Human Temporal Bone Registry at Harvard and the three currently active laboratories at Harvard, University of Minnesota and UCLA.
Help create other temporal bone facilities in other universities and centers.
Educate your congressional delegation of the dire need for NIDCD support for this overlooked critical area of research.
Support the blue ribbon Task Force chaired by Dr. Richard A. Chole, professor and chairman at Washington University and Michael J. McKenna, MD, professor at Harvard, developed under the aegis of the Academy with the generous initial funding from Michael M. Paparella, MD, that has created an Otopathology Endowment to help reverse the decline in otopathology.
Encourage and recruit a patient with a significant ear condition, disease, or clinical course with good clinical records to bequeath their temporal bones to the National Human Temporal Bone Registry.
Thank you for your support and your patients’support including financial pledges either current or in an estate plan. If you or your patients would like to support the AAO-HNSF/ Michael M. Paparella, MD Endowed Grant for Research in Clinical Otopathology, visit www.entnet.org/donate, click on “donate,”and you will be taken to the donation page where this Endowment is listed. Or, you may email Ron Sallerson, senior director of development at rsallerson@entnet.org. 
When the baton is passed from one elected leader to another, it carries with it a responsibility of stewardship and the privilege of trust. After nearly a year, I now prepare to ensure a smooth transfer to my successor and colleague, Gayle E. Woodson, MD. As I prepare for this transition, I am excited that the AAO-HNS/F has come so far this year and that I had the honor to be so engaged. Since I assumed office, we have strategically worked in areas that we hope will make the biggest difference for you. With ongoing networking and education opportunities and added resources to improve your medical practice, our goal is to help you navigate your career path and meet your professional goals. Let me share a brief overview:
Membership and Communications
We moved forward in key areas of Member communication. You are able to discuss sensitive issues through the new Member-only portal ENTConnect, a newly designed Member-friendly website offering a format that is easy to read on the go, attractive, media rich, and navigable.
Education and the Annual Meeting
The AAO-HNS/F acted to consolidate and enhance the otolaryngology practice gap analysis and needs assessment process. As a result, the Annual Meeting abstract submission process is including education needs identified via our assessment. To that end, 10 live Clinical Fundamentals courses were presented at the 2013 Annual Meeting and hosted online in January 2014 and more than 260,000 CME credits were awarded.
Policy and Research Combined for Quality Care
From evidence-based clinical practice guidelines to reimbursement guidance, the resources we make available to Members are invaluable and often result in recouping the cost of annual dues. You will see this expressed as “We’ve Got You Covered.”These resources developed with the Academy’s Physician Payment Policy (3P) workgroup, included information about the transition to ICD-10 and CMS Quality Programs. During the past year, the Academy has developed five Fact Sheets on CMS quality reporting, which will include payment penalties for those who do not successfully participate by 2015.
Clinical Practice Guidelines that will be published soon in Otolaryngology—Head and Neck Surgery are Acute Otitis Externa, Tinnitus, Allergic Rhinitis, Update to Adult Sinusitis and several Consensus Statements.
Federal and Grassroots Advocacy
AAO-HNS Members are backed by a network of nearly 12,000 peers and a dedicated staff working to achieve policy changes at the federal, state, and local levels. Grassroots activities have been enhanced to recognize and involve Members with the In-district Grassroots Outreach (I-GO) program that had 20 local events scheduled through June 2014. Integrating advocacy with health policy issues, the AAO-HNS met face to face with CMS and CMMI (Center for Medicare and Medicaid Innovation) in November and June on payment and measures issues, with development of two new measures groups resulting from our advocacy efforts.
I have no doubt that Dr. Woodson will contribute significantly to the AAO-HNS/F’s advancement as she assumes her presidential responsibilities and accepts the baton at the conclusion of our upcoming annual meeting in Orlando.