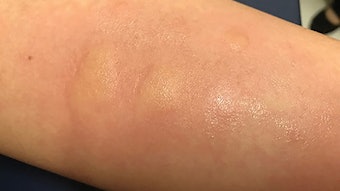
Transition to In-office Treatments: Allergy
During this unprecedented season of social distancing and significant restrictions in patient care as a result of the coronavirus pandemic, it is easy to feel helpless in finding ways to help our patients and our communities. Without question, our systems for delivery of otolaryngic and allergy care to our patients will change as a result of this pandemic.
Penicillin Allergy Testing – Something We All Can Do for Our Community
Erik R. Swanson, MD, and Jamie F. Kimbrough, MD
During this unprecedented season of social distancing and significant restrictions in patient care as a result of the coronavirus pandemic, it is easy to feel helpless in finding ways to help our patients and our communities. Without question, our systems for delivery of otolaryngic and allergy care to our patients will change as a result of this pandemic. And although we still have much to learn regarding keeping our patients safe from novel viral infections, there is a step we can all take to decrease the rise of resistant bacterial infections in our community—engage more in skin testing for penicillin allergy.
Approximately 10% of patients report an allergy to penicillin. However, when skin tested to penicillin, over 90% of these patients test negative and tolerate a subsequent oral challenge.1 Treating patients who report a penicillin allergy without a complete evaluation of this potential drug allergy impacts patients and our communities in several ways. These patients are often treated with broad spectrum antibiotics for infections that could have been appropriately managed with a beta-lactam antibiotic. In our specialty, this includes avoiding preferred first-line antibiotics for our most common infectious presentations such as sinusitis, tonsillitis, and otitis media. It also includes our use of perioperative antibiotics for soft tissue surgical cases. Use of alternative antibiotics in these cases leads to increased healthcare costs, the progression of multiple drug-resistant organisms, and higher risks of toxicity for patients receiving these antibiotics. Patients who report a penicillin allergy have increased risk for contracting Clostridium difficile colitis (23%), methicillin-resistant Staphylococcus aureus (14%), and vancomycin-resistant Enterococcus (30%) compared with the general population.2
Skin testing for penicillin allergy has been performed since the 1950s and now is commercially available in an FDA-approved, standardized test kit. This allows for the testing of a major antigenic determinant in all our clinics in a safe manner. In fact, penicillin allergy testing is safe in most all populations, including pregnant patients3 and those requiring organ transplantation.4 Patients who have had a negative skin test have minimal risk of developing an IgE-mediated reaction to an oral challenge of penicillin. We perform this oral challenge in our clinic in a controlled setting following the receipt of a negative penicillin skin test. We use a graded oral challenge starting with a 50 mg dose of amoxicillin followed by a dose of 250 mg. We have the fortune of having exceptional medical allergists in our practice who can support us in cases of equivocal skin test results or complicated histories with severe reactions. Resensitization is rare after treatment with oral penicillin, but it can occur more commonly after parenteral administration. Following a negative skin test and successful oral challenge, the patient should still be counseled of the very low risk of a false negative test and the risk for resensitization.
Unfortunately, at this time, skin testing for antibiotic allergies other than beta-lactams is not standardized. But we all have an opportunity to use the highly effective tool of penicillin allergy testing to improve the lives of our patients and the trajectory of infectious disease in our community. For most disease entities we treat, very few can be permanently removed from a patient’s medical record as a result of our care for them. Penicillin drug allergy is a wonderful exception to this rule. By simply setting up our clinics with the ability to skin test patients and asking screening questions on a routine basis, we can remove this harmful “diagnosis” from our patient’s medical record in over 90% of cases. What a great example of “First, do no harm.”
References
- Macy E, Ngor E. Safely diagnosing clinically significant penicillin allergy using penicilloyl-poly-lysine, pencillin, and oral amoxicillin. J Allergy Clin Immunol Pract. 2013;1(3):258-263.
- Macy E, Contreras R. Health care use and serious infection prevalence associated with hospitalized patients. J Allergy Clin Immunol Pract. 2014;133(3):790-796.
- Philipson E, Land D, Gordon S, Burlingame J, Emery S, Arroliga M. Management of group B Streptococcus in pregnant women with penicillin allergy. J Reprod Med. 2007;52(6):480-484.
- Gutta R, Radojicic C. Safety and effectiveness of penicillin allergy evaluation in pre-lung transplant patient population. J Allergy Clin Immunol. 2012;129(2):A102.