The Road to Relevance
The Road to Relevance Last month, the Academy and Foundation conducted their board meetings, immediately following our annual strategic planning. These events were part of our Leadership Forum, which included our Board of Governors meetings and their associated committees, and advocacy and health policy training. Additionally, clinical practice guidelines, The Sunshine Act, practice management, and a Model Society Forum sharing best practices from our BOG societies, among others, were topics of interest. The breadth of offerings and knowledge needed for otolaryngologists to learn what’s necessary to comfortably navigate the healthcare industry can be daunting. As you can imagine, when your boards of directors meet, one of their greatest challenges is how to cover that broad range of needed information, and still maintain the focus necessary to target the highest priority issues for you, our members, and your patients. For the last two years, the Academy has benefited from the personal facilitation and the published knowledge of Harrison Coerver, who along with Mary Byers, has co-authored two books for association management professionals: Race for Relevance and Road to Relevance. Following a model, which they have proposed, Academy leaders have done a lot of pre-strategic planning homework reviewing Academy and Foundation projects and processes, and creating a “forced ranking” of all our work. Just the simple tabled outline of this prioritized matrix takes almost 70 rows and 14 columns to summarize on a spreadsheet. A more detailed work plan is many times that size. Everything from products (educational, journal, quality improvement guidelines and measures, Annual Meeting programming) to advocacy services (health policy, legislative, and regulatory) to support services (humanitarian support, grants and financial services, communications, IT) and much more is part of this review. The purpose of this critical evaluation, and the points of Coerver’s books and consultative services, is to strategically maximize benefit to members. Coerver defines strategy as “the skillful, creative, and disciplined use of an organization’s resources to achieve its objectives.” Like most primary national medical associations, our membership is robust and diverse in its needs, desires, and expectations. Without a systematic and disciplined process, “mission creep” expands our initiatives to the point that excellence and efficiency in critical areas are compromised to accommodate wide-ranging desires. The process of prioritizing is painful and fraught with strongly held competitive positions, passionately expressed. Concentrating our efforts is essential to increasing our relevance to you. A famed management consultant, author, and educator, Peter Drucker, is quoted as writing, “Wherever we find a business that is outstandingly successful, we will find that it has thought through the concentration alternatives, and has made a concentration decision.” He continues: “The worst thing to do is a little bit of everything. This makes sure that nothing is being accomplished. It is better to pick the wrong priority than none at all.” While we have no desire to pick the wrong priority, we agree with Drucker that it’s dangerous to pick none at all. Any list of services suggested by our members, even if it contains elements that the majority of our members do not value or would not use, contains items that somebody felt was a priority. But, when you prioritize everything, you’ve prioritized nothing. Coerver writes, “[It’s] better to have an honest conversation about [the] future—however difficult this may be—than not to talk at all.” Based on this facilitation, membership surveys and engagement, and board and staff preparation, including extensive review of our past strategies, products, and services, and our future challenges, we are working to advance our effectiveness and value to otolaryngologist-head and neck surgeons by: Building on strengths Concentrating resources Integrating programs and services Aligning people and processes for efficiency, and when indicated, Abandoning services and activities when necessary This year you will see the Academy offering you increasingly relevant products and services, as well as opportunities for community, engagement, service, and a more satisfying professional experience. With Road to Relevance, we intend to focus on helping you “work less stressfully, more productively, and more profitably.”
 David R. Nielsen, MD AAO-HNS/F EVP/CEO
David R. Nielsen, MD AAO-HNS/F EVP/CEOThe Road to Relevance
Last month, the Academy and Foundation conducted their board meetings, immediately following our annual strategic planning. These events were part of our Leadership Forum, which included our Board of Governors meetings and their associated committees, and advocacy and health policy training. Additionally, clinical practice guidelines, The Sunshine Act, practice management, and a Model Society Forum sharing best practices from our BOG societies, among others, were topics of interest. The breadth of offerings and knowledge needed for otolaryngologists to learn what’s necessary to comfortably navigate the healthcare industry can be daunting.
As you can imagine, when your boards of directors meet, one of their greatest challenges is how to cover that broad range of needed information, and still maintain the focus necessary to target the highest priority issues for you, our members, and your patients.
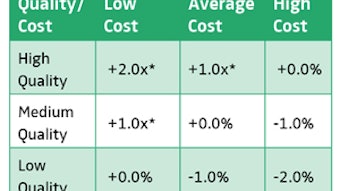
For the last two years, the Academy has benefited from the personal facilitation and the published knowledge of Harrison Coerver, who along with Mary Byers, has co-authored two books for association management professionals: Race for Relevance and Road to Relevance. Following a model, which they have proposed, Academy leaders have done a lot of pre-strategic planning homework reviewing Academy and Foundation projects and processes, and creating a “forced ranking” of all our work. Just the simple tabled outline of this prioritized matrix takes almost 70 rows and 14 columns to summarize on a spreadsheet. A more detailed work plan is many times that size. Everything from products (educational, journal, quality improvement guidelines and measures, Annual Meeting programming) to advocacy services (health policy, legislative, and regulatory) to support services (humanitarian support, grants and financial services, communications, IT) and much more is part of this review.
The purpose of this critical evaluation, and the points of Coerver’s books and consultative services, is to strategically maximize benefit to members. Coerver defines strategy as “the skillful, creative, and disciplined use of an organization’s resources to achieve its objectives.”
Like most primary national medical associations, our membership is robust and diverse in its needs, desires, and expectations. Without a systematic and disciplined process, “mission creep” expands our initiatives to the point that excellence and efficiency in critical areas are compromised to accommodate wide-ranging desires. The process of prioritizing is painful and fraught with strongly held competitive positions, passionately expressed.
Concentrating our efforts is essential to increasing our relevance to you. A famed management consultant, author, and educator, Peter Drucker, is quoted as writing, “Wherever we find a business that is outstandingly successful, we will find that it has thought through the concentration alternatives, and has made a concentration decision.” He continues: “The worst thing to do is a little bit of everything. This makes sure that nothing is being accomplished. It is better to pick the wrong priority than none at all.”
While we have no desire to pick the wrong priority, we agree with Drucker that it’s dangerous to pick none at all. Any list of services suggested by our members, even if it contains elements that the majority of our members do not value or would not use, contains items that somebody felt was a priority. But, when you prioritize everything, you’ve prioritized nothing. Coerver writes, “[It’s] better to have an honest conversation about [the] future—however difficult this may be—than not to talk at all.”
Based on this facilitation, membership surveys and engagement, and board and staff preparation, including extensive review of our past strategies, products, and services, and our future challenges, we are working to advance our effectiveness and value to otolaryngologist-head and neck surgeons by:
- Building on strengths
- Concentrating resources
- Integrating programs and services
- Aligning people and processes for efficiency, and when indicated,
- Abandoning services and activities when necessary
This year you will see the Academy offering you increasingly relevant products and services, as well as opportunities for community, engagement, service, and a more satisfying professional experience. With Road to Relevance, we intend to focus on helping you “work less stressfully, more productively, and more profitably.”