Kenya Relief at the Brase Clinic
Anya J. Miller, MD Humanitarian Grant Awardee, Resident, Henry Ford Hospital Royal Oak, MI Last September, I traveled with a team from Henry Ford Hospital and the University of Michigan to Migori, Kenya, with Kenya Relief. Under the supervision of Lamont R. Jones, MD, and Greg Basura, MD, PhD, we performed otologic surgery at the Brase Clinic. With the assistance of local nurses, scrub techs, and nurse practitioners, we were able to perform surgeries including hemithyroidectomies, tympanoplasties, cleft lips, and various lumps and bumps. Although we operated out of a clinic and not a hospital, our patients were able to stay overnight for observation due to the support of local nurses. Despite the occasional fly in the operating room, we enjoyed many amenities such as air conditioning, OR tables that moved up and down, operating microscopes, and Neptune suction machines, to name a few. In fact, after touring the local district hospital, our clinic appeared much better equipped thanks to many generous donations throughout the years. Supplementing with some supplies from home such as an ear tray and LED headlights, we were able to safely provide surgical care to the people. The majority of the surgical patients who arrived for ENT evaluation were women with goiters. While we were able to alleviate much of the compression and cosmetic deformity with a hemithyroidectomy, we were not able to provide them with a real long-term solution. For smaller goiters, we prescribed iodine drops and education on iodized salt. It was unfortunate that we had not brought with us any iodine drops to dispense to the patients, so how many people were actually able to get the medication is uncertain. While I do believe our team made a difference and patients were happy to have the surgery, multiple ENT teams arrive at the Brase Clinic each year and perform many surgeries for goiters. Despite this, the patients lined up with goiters are endless each time. It seems that the people in Kenya could benefit from ENT mission groups joining efforts with public health specialists. Given all the resources invested in taking a team to Kenya, a multidisciplinary approach to this issue could be both cost effective and provide a more substantial benefit to the local people. Without this or a similar effort, it seems inevitable that the lines of people waiting to have their goiters removed will continue to be lengthy. While we were there to serve the people of Kenya, from a resident’s perspective, there was much personal benefit derived from this experience as well. I was able to give my undivided attention to each surgical case without pagers going off, heading off to complete other clinical duties, or anything else that might draw my attention away from the case at hand. We also performed similar cases often, so I was able to learn from each case and improve on those skills without having days or weeks between cases to forget what I had learned. Having consistency in attendings also meant that I could reliably anticipate the next move, which also seemed to accelerate my learning. Medical missions are in general a huge undertaking for everyone involved, but patients are universally thankful and resident benefit is priceless. Because time and money committed to this endeavor is great, each mission group should look at the needs of the particular area and try to tailor their mission accordingly to maximize impact. Many thanks to the AAO-HNSF Humanitarian Efforts Committee for its grant that made my participation possible. Kenya Relief Brase Clinic P.O. Box 1078 Suna, Migori Kenya, Africa 40400 Contact: Dominic, Clinical Officer 011-254-724-777-048 Keptembwa@yahoo.com
Anya J. Miller, MD
Humanitarian Grant Awardee,
Resident, Henry Ford Hospital
Royal Oak, MI
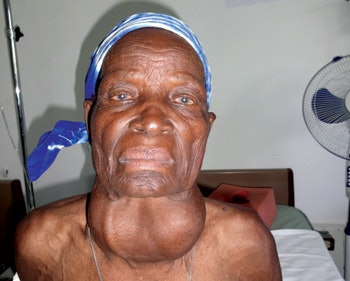 Preoperative photo of a 72-year-old woman with a goiter for more than 30 years.
Preoperative photo of a 72-year-old woman with a goiter for more than 30 years.
Although we operated out of a clinic and not a hospital, our patients were able to stay overnight for observation due to the support of local nurses. Despite the occasional fly in the operating room, we enjoyed many amenities such as air conditioning, OR tables that moved up and down, operating microscopes, and Neptune suction machines, to name a few. In fact, after touring the local district hospital, our clinic appeared much better equipped thanks to many generous donations throughout the years. Supplementing with some supplies from home such as an ear tray and LED headlights, we were able to safely provide surgical care to the people.
The majority of the surgical patients who arrived for ENT evaluation were women with goiters. While we were able to alleviate much of the compression and cosmetic deformity with a hemithyroidectomy, we were not able to provide them with a real long-term solution. For smaller goiters, we prescribed iodine drops and education on iodized salt. It was unfortunate that we had not brought with us any iodine drops to dispense to the patients, so how many people were actually able to get the medication is uncertain.
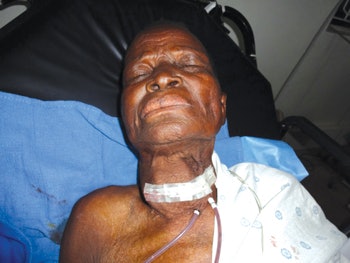 Postoperative photo after hemithyroidectomy. Her thyroid was so large that her carotid was adherent to the capsule and her internal jugular vein had little to no flow.
Postoperative photo after hemithyroidectomy. Her thyroid was so large that her carotid was adherent to the capsule and her internal jugular vein had little to no flow.
While we were there to serve the people of Kenya, from a resident’s perspective, there was much personal benefit derived from this experience as well. I was able to give my undivided attention to each surgical case without pagers going off, heading off to complete other clinical duties, or anything else that might draw my attention away from the case at hand. We also performed similar cases often, so I was able to learn from each case and improve on those skills without having days or weeks between cases to forget what I had learned. Having consistency in attendings also meant that I could reliably anticipate the next move, which also seemed to accelerate my learning.
Medical missions are in general a huge undertaking for everyone involved, but patients are universally thankful and resident benefit is priceless. Because time and money committed to this endeavor is great, each mission group should look at the needs of the particular area and try to tailor their mission accordingly to maximize impact. Many thanks to the AAO-HNSF Humanitarian Efforts Committee for its grant that made my participation possible.
P.O. Box 1078
Suna, Migori
Kenya, Africa 40400
Contact:
Dominic, Clinical Officer
011-254-724-777-048
Keptembwa@yahoo.com