Are Your Pediatric Patients Part of the “Team?”
Because February is our Academy’s Kids ENT Health month, we all have the opportunity to shine the spotlight on certain Kids ENT health issues and direct patients and parents to accurate information that affect this younger segment of our patient population (ENTHealth.org). This month, we also have a chance to pause and reflect on the way we communicate with, care for, and influence our pediatric patients along with their parents.
 Duane J. Taylor, MD AAO-HNS/F Past President
Duane J. Taylor, MD AAO-HNS/F Past President
Every interaction I have with a child has been viewed through a different lens based on experiences (including being a parent). My pediatrics hospital rotation in medical school was my initial exposure to working with sick children, and I remember it vividly. My first patient was a 12-year-old boy (call him Andy) who suffered from a rare congenital cardiomyopathy. Andy had frequent hospital admissions, and the staff were quite familiar with him and his condition. Andy’s twin had passed away from the same condition just a few months prior to my starting the rotation, and his life expectancy was not anticipated to be much longer without a transplant.
This initial experience (as a soon-to-be doctor) required me to understand the perspective and experiences of this young patient and his parents as they struggled through this ritual of hospitalizations with an ominous prognosis. The lessons and insights I learned from following and listening to this young person and watching how the experienced team interacted with both him and his parents would lay the foundation for my relationships with many pediatric patients and their parents throughout my training and career.
Andy knew the possibility of an early demise was real, yet he stayed positive. He yearned for support through hope with every interaction and appreciated the human touch as well as the measured realities that were presented to him daily by his doctors and the rest of the healthcare team. Such wisdom and courage I had never witnessed in someone this young, but I appreciated it. I realized the value of making kids (along with their parents) part of the “team” from the beginning was as important as the information, knowledge, and compassion given to the parents.
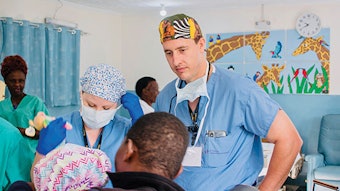
My second most memorable early experience with a pediatric population was a month-long medical mission to South America during my senior year of medical school. This was one of the many life-changing experiences that truly shaped me as a person and reaffirmed my commitment to be a physician. I was selected to join a team of doctors, nurses, medical students, and other volunteers from North America as a part of an ophthalmology medical mission traveling to a small town in Ecuador. We worked in a makeshift clinic housed in a church that saw hundreds of patients (most of whom were children of all ages brought in by their parents) who waited patiently in line after trekking for miles to be seen by our team.
Those patients needing surgery were scheduled and had procedures in a tiny OR in a nearby hospital. Although supplies were shipped in, the resources and facilities were limited. The need to triage patients by severity of condition, availability for follow-up visits, and compliance had to be discerned with an interpreter by members of the team quickly.
I admired the parents who brought their children dressed in their “Sunday best” for medical care in spite of the challenges of poverty they faced back home. I tried my best to meet and greet each with the dignity they deserved for this effort.
Each of us on the front lines heard personal perspectives from each child (who could give it) and their parent or grandparent regarding their problem and followed with an engaging dialogue and treatment plan. The gratitude and appreciation shown by these parents/relatives and children was heartfelt, and the growth I experienced (in this case in another culture) was priceless and immeasurable.
In both of these early experiences, communication, understanding, building trust, being nonjudgmental, and inclusion in team decisions proved to be equally important and critical to building my foundation for the many youth/parent encounters that would follow. As the composer John Powell said, “Communication works for those who work at it.” So, let’s not forget this applies to the kids you see and their parents. I encourage you all to explore and review how you and your staff might enhance interactions with your pediatric patients this month.