Making a Difference in the Lives and ENT Health of Our Armed Forces
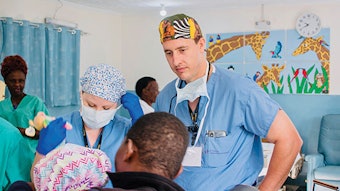
LaKeisha R. Henry, MD, holds the rank of Colonel in the U.S. Air Force (USAF) and currently serves as Division Chief at the Department of Defense Hearing Center of Excellence (HCE), located in the Wilford Hall Ambulatory Surgery Center at Joint Base San Antonio-Lackland, Texas. HCE is part of the Defense Health Agency and is a collaborative effort with the Department of Veterans Affairs.
LaKeisha R. Henry, MD, holds the rank of Colonel in the U.S. Air Force (USAF) and currently serves as Division Chief at the Department of Defense Hearing Center of Excellence (HCE), located in the Wilford Hall Ambulatory Surgery Center at Joint Base San Antonio-Lackland, Texas. HCE is part of the Defense Health Agency and is a collaborative effort with the Department of Veterans Affairs. HCE facilitates auditory and vestibular research and develops best practices that enhance the prevention, diagnosis, mitigation, treatment, and rehabilitation of patients with associated disorders.
 LaKeisha R. Henry, MD, Colonel, USAF, MC, FS
LaKeisha R. Henry, MD, Colonel, USAF, MC, FSDr. Henry is an assistant professor in the Department of Surgery at the Uniformed Services University of the Health Sciences (USUHS) and an Advanced Trauma Life Support instructor. She was Otolaryngology Consultant to the Air Force Surgeon General for several years, which allowed her to mentor residents and other otolaryngologists. She served as the 59th Medical Group’s Otolaryngology Master Clinician and has held the position of Squadron Commander in addition to other leadership roles during clinical assignments both in the United States and overseas.
“I knew that I enjoyed helping people, and I was looking for a long-term career where I could make a difference in the military beyond my initial commission. I thought I might become a pediatrician, but with a bachelor’s degree in Engineering Management, I like to tinker with my hands, so I considered surgery,” she said.
Dr. Henry is a cross-service graduate, which means that after graduating from the U.S. Military Academy at West Point, she took a commission into the USAF instead of the Army. Along the way, two of her West Point classmates encouraged her to attend medical school and a mentor inspired her to consider otolaryngology as a career path.
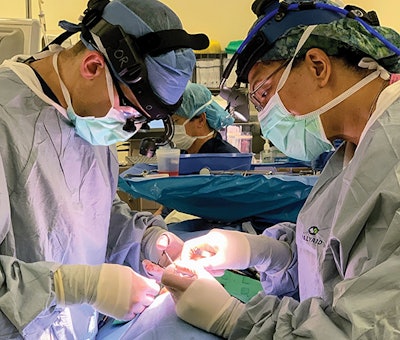 Dr. LaKeisha R. Henry performs surgery with resident John W. Lally, MD
Dr. LaKeisha R. Henry performs surgery with resident John W. Lally, MD“I became interested in providing service for all genders, all age groups, and after being exposed to a number of surgical specialties, I learned more about otolaryngology and began to appreciate the complex anatomy of the specialty, the people, the personalities, the family, and community concept of ENT surgeons, and the ability to mix aspects of the whole patient, whether they need surgery or not. I really liked the provider-patient relationship of other medical specialties, so ENT appealed to me.”
During the time between graduating from medical school from USUHS and completing a residency in otolaryngology at the San Antonio Uniformed Services Health Education Consortium, Dr. Henry became a flight surgeon. Trained in aerospace medicine and disorders that can occur at or are associated with altitude, a flight surgeon is the primary care provider for an aviation unit’s members and their families.
Upon completing her residency, Dr. Henry was based mostly in community-sized hospitals, which meant moving every three to four years while enjoying a comradery with other clinicians and a true team approach to patient care. She was assigned to Royal Air Force Lakenheath Hospital in Suffolk, England, before being transferred to Landstuhl Regional Medical Center in Germany. She returned to the U.S. when she was assigned to Mike O’Callaghan Military Medical Center at Nellis AFB, Nevada. After being selected as a Squadron Commander, she began assuming more leadership responsibilities in the Washington, DC, area before arriving at Joint Base San Antonio-Lackland.
 Dr. LaKeisha R. Henry welcomes speakers and attendees to the Society of Military Otolaryngologists Trauma Symposium prior to the start of the AAO-HNSF 2018 Annual Meeting & OTO Experience in Atlanta, GA
Dr. LaKeisha R. Henry welcomes speakers and attendees to the Society of Military Otolaryngologists Trauma Symposium prior to the start of the AAO-HNSF 2018 Annual Meeting & OTO Experience in Atlanta, GA“My practice would be based on the population of the military installation I was assigned to, including beneficiaries such as active-duty personnel, retirees, and their family members, as well as reservists and VA patients,” she explained. “Sometimes, that also included patients who had been evacuated from deployed or austere environments.
“Prior to being assigned in Germany, I deployed to Afghanistan. I don’t think there was another ENT in theater, but we had a head and neck team that included a neurosurgeon, myself, our technician, and a colleague who was a reservist dentist. It was a comprehensive practice that included treating trauma and battlefield-type exposures…and during my tour, we took care of U.S. forces, NATO and coalition forces, the host nation [Afghan] army, and civilian [local national] patients who were injured.
“There were opportunities to provide humanitarian care while I was deployed. Deployment is one of the highlights of my career because it was rewarding and challenging in many ways. You’re not looking for someone to give you gratitude but having the opportunity to make a difference in the lives of our forces and others was something very special. I was grateful to have had that opportunity.”
Dr. Henry describes her typical practice as general in nature, treating conditions similar to other otolaryngologists, but there are specific requirements for ensuring that someone is fit for active military duty. Trauma-related conditions and noise-induced hearing loss are of particular interest to the military because there are certain aspects of military service that make hearing a critical sense. Service members need to maintain situational awareness, be able to localize within their surroundings, and communicate clearly and effectively with their unit.
Because military otolaryngologists move to various assignments more often than their civilian counterparts, being able to take advantage of and secure funding for continuing education courses can be a challenge. As a member of the AAO-HNS since she was a resident, Dr. Henry explains that military members often do not receive permission to attend the AAO-HNSF Annual Meeting & OTO Experience, for example, until right before it begins. That can make logistical planning and registering for pre-meeting courses—valuable opportunities for residents and staff surgeons—difficult.
Even so, she feels that military members are encouraged to participate in and become involved with AAO-HNS committees, and she sees opportunities for certification and continuing education growing, such as online learning options and being able to view Annual Meeting session presentations back home (non-attendees can purchase the Annual Meeting Webcasts with all 338 recorded sessions through AcademyU). “The Academy is constantly looking for ways to add value for its members.”
Dr. Henry serves as Chair of the AAO-HNS Trauma Committee. In conjunction with the Society of Military Otolaryngologists (SMO), the committee hosts a Trauma Symposium on the Saturday before the start of the Annual Meeting, which is another forum for military otolaryngologists to network and share lessons learned that may not be solely unique to military situations, but cross over the breadth of the specialty. The Trauma Symposium welcomes Annual Meeting and local participants and offers CME credit.
Dr. Henry feels that the specialty has grown in diversity and maintains the highest standards of care and expectations from the AAO-HNS community. She feels that it’s important to continue encouraging diversity in all forms, particularly for women and fulfillment and balance in surgical specialties, as well as developing leadership and mentoring opportunities.
“Our specialty encourages broad competencies for generalists as well as subspecialists and I would like to see that continue,” she explained. “I’ve noticed in specialties outside of otolaryngology there seems to be more and more restrictions placed on generalists and the types of procedures they can perform. Especially within the military, we are expected to practice appropriately within our capabilities, but we must maintain comprehensive and broad skills sets given varying practice environments. This is also important when caring for deployed patients in theater hospitals.
“We’re also able to collaborate and consult with colleagues who may have more specialized training or experience in a certain area, and I hope we continue to maintain that level of comradery within our specialty in order to provide the best possible care for our patients. I appreciate the opportunity to practice alongside a community of talented ENT specialists while leading the HCE and guiding enthusiastic new residents.”
The views expressed are those of the author and do not necessarily reflect the official policy of the DoD Hearing Center of Excellence, Defense Health Agency, or Department of Defense. This information is provided for education purposes only. Reference to any commercial product or service does not imply endorsement by the Department of Defense or DoD Hearing Center of Excellence.