Humanitarian Travel Grant: Medical Mission in Mongolia
In May 2020 I traveled with the New York University (NYU) Department of Otolaryngology to Ulaanbaatar, Mongolia, for a humanitarian mission.
Zahrah M. Taufique, MD

In May 2020 I traveled with the New York University (NYU) Department of Otolaryngology to Ulaanbaatar, Mongolia, for a humanitarian mission. The surgical team was composed of head and neck surgeons Theresa Tuyet-Phuong N. Tran, MD, and Adam S. Jacobson, MD, along with me, a fourth-year resident, and microvascular fellow Jason L. Yu, MD. We were accompanied by physician assistant Sabrina Tarafdar, as well as operating room nurses Ana Mae Gaolingo, Justine Padilla, Chris Abanico, Vicsyl Rodriguez, and Lauren Hamill.
Mongolia is an East Asian country that lies between China and Russia. The Mongolian Empire was the largest empire to have ever existed due to the leadership of Chinggis Khan, a figure who still heavily dominates current Mongolian culture. As a result of its historically nomadic culture, its capital Ulaanbaatar only settled in its current location in 1773. The group traveled with the Virtue Foundation, a nonprofit organization that has been sending surgeons to Mongolia for over a decade.
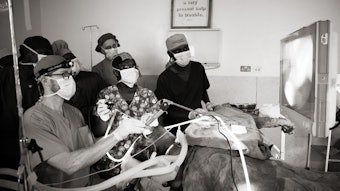
There were two hospitals in Ulaanbaatar where the group attended clinic and operated: the military hospital and the National Cancer Center. Though team members performed a variety of surgeries ranging from rhinoplasties to oncologic resections, they discovered there was a great need for education on reconstructive techniques for oncologic, traumatic, and iatrogenic defects. Specifically, microvascular reconstruction is a relatively new field in Mongolia. The only hospital in Mongolia currently performing free flaps is the National Cancer Center, where the first free flap was performed about 10 years ago. Still, the demand for free flap reconstructive expertise is high, and the surgeons performing these surgeries were eager to learn from the NYU group throughout the week.
One exemplary case was a fibular free flap for an orocutaneous fistula in a young man who had suffered from a gunshot wound to the face one year prior. He had undergone mandibular plating immediately after the injury; however, there was nonunion of the bone and fistula development. He had been following up at the military hospital for some time for local wound care. Upon arrival in Ulaanbaatar, the NYU team reviewed his case, and he underwent segmental mandibulectomy, excision of orocutaneous fistula, tracheostomy, fibula free flap, and plating. His postoperative course was uneventful. He was decannulated on postoperative day four and was able to resume a diet one week after surgery. Though the surgery itself was a success, even more valuable was the ability to teach the local surgeons these techniques and improve on their baseline knowledge of head and neck surgery.
By the end of the week, it was clear that a strong partnership developed between the American and local surgical teams, and there is ongoing discussion on how to continue this educational relationship in the future.