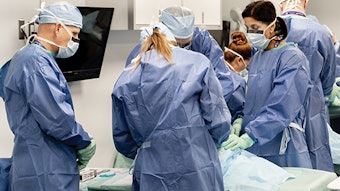
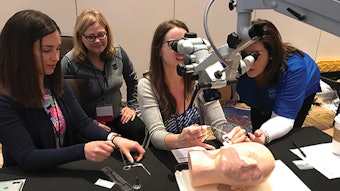
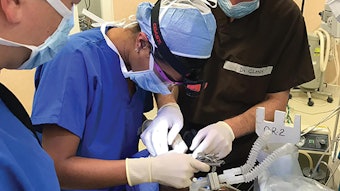
Out of Committee: Patient Safety and Quality Improvement – Safety of Office-based Laryngology Procedures
Within medicine, otolaryngology-head and neck surgery is often recognized for its balance of surgical procedures and clinical care of patients. Throughout the field of otolaryngology, there has been a shift over time to move an increasing number of our surgical procedures into the office setting.
VyVy N. Young, MD
Within medicine, otolaryngology-head and neck surgery is often recognized for its balance of surgical procedures and clinical care of patients. Throughout the field of otolaryngology, there has been a shift over time to move an increasing number of our surgical procedures into the office setting.1-3 Increased efficiency, enhanced cost-effectiveness, and high procedural tolerance coupled with low complication rates have led to both patient and surgeon preference for office-based procedures when appropriate.4-11
In laryngology especially, this trend has been quite pronounced. Laryngology procedures now commonly performed in the office setting include laryngoscopy, bronchoscopy, transnasal esophagoscopy, biopsy, vocal fold injection (e.g., augmentation, steroid, or botulinum toxin), laser treatment of laryngeal pathology, esophageal dilation, and even some airway surgery (e.g., laser, dilation, or steroid injection).6,10-19 For reference, the American Academy of Otolaryngology–Head and Neck Surgery and its Foundation (AAO-HNS/F) outlined a Position Statement with supporting evidence related to in-office photoangiolytic laser treatment of laryngeal pathology.20
Multiple techniques to perform these procedures, either through the use of the working channel of an endoscope versus a percutaneous or transoral approach, have been described. Some methods may be performed with a single surgeon while others require an assistant.2,10,13-16,18,21-24 Often these are unsedated procedures, performed under local anesthesia. The local anesthetic may be administered to the laryngopharynx indirectly via nebulizer treatment, percutaneously via transtracheal approach, or directly through an instrument (e.g., Abraham cannula) or the working channel of an endoscope.2,25 Otolaryngologists performing these procedures should be familiar with multiple techniques, both for administration of local anesthesia and for the procedure itself, to enhance patient safety and likelihood of procedure success.
Office-based laryngology procedures are generally considered safe, related to a low-reported complication rate.5,6,10,14-18,26 Complications are minor (including patient anxiety/intolerance of the procedure, epistaxis, vasovagal response, coughing, or gagging), tend to be mild in nature, and often spontaneously resolve.5,12 More serious complications are even more rare but may include laryngospasm, airway compromise, significant bleeding/hematoma, or a cardiac event.12 It is imperative that the otolaryngologist be aware of the potential for complications and have a safety plan in place to address any issues that arise.
Proper identification of appropriate candidates for these types of procedures is fundamental. Multiple studies have reported hemodynamic changes during awake laryngology procedures, including a 20mm Hg increase in blood pressure (BP).27-29 Therefore, monitoring of vital signs (at a minimum, BP and heart rate) at least before and after the procedure is recommended to verify that the patient remains within a safe range from a cardiovascular standpoint. A multi-institutional study described a screening protocol identifying patients in need of further cardiovascular evaluation prior to pursuing an office-based procedure (e.g., those patients with systolic BP >160, diastolic BP >100, and/or HR >110 beats/minute).30 Risk factors identifying potentially poor candidates for office-based otolaryngology procedures have been nicely summarized by Schmalbach.3 Otolaryngologists performing office-based procedures should have ready access to all the equipment necessary to perform the procedure, as well as any other supplies that may be needed to address potential complications. In this regard, checklists may be particularly helpful—especially for resuscitation equipment, which is thankfully only rarely utilized.3,31
In summary, although it is a procedurally based surgical subspecialty, otolaryngology covers the spectrum from operative to ambulatory practice. Advances in laryngology in particular have allowed an increasing number of procedures to be performed in the office setting. Reports of safety have been favorable to date. Pre-procedure screening (e.g., vital signs and American Society of Anesthesiologist [ASA] level) and suitable patient selection lies at the heart of office-based laryngeal procedure safety. Continued vigilance and monitoring are vital as we move forward, especially for those practitioners newly adding office-based procedures to their clinical practice.
References
- Urman RD, Punwani N, Shapiro FE. Office-based surgical and medical procedures: educational gaps. Ochsner J. 2012; 12:383-388.
- Rosen CA, Amin MR, Sulica Let al. Advances in office-based diagnosis and treatment in laryngology. Laryngoscope. 2009; 119 Suppl 2:S185-212.
- Schmalbach CE. Patient safety and anesthesia considerations for office-based otolaryngology procedures. Otolaryngol Clin North Am. 2019; 52:379-390.
- Bove MJ, Jabbour N, Krishna P, et al. Operating room versus office-based injection laryngoplasty: a comparative analysis of reimbursement. Laryngoscope. 2007; 117:226-230.
- Young VN, Smith LJ, Sulica L, Krishna P, Rosen CA. Patient tolerance of awake, in-office laryngeal procedures: a multi-institutional perspective. Laryngoscope. 2012; 122:315-321.
- Naidu H, Noordzij JP, Samim A, Jalisi S, Grillone GA. Comparison of efficacy, safety, and cost-effectiveness of in-office cup forcep biopsies versus operating room biopsies for laryngopharyngeal tumors. J Voice. 2012; 26:604-606.
- Shah PD. Patient safety and quality for office-based procedures in otolaryngology. Otolaryngol Clin North Am. 2019; 52:89-102.
- Rees CJ, Halum SL, Wijewickrama RC, Koufman JA, Postma GN. Patient tolerance of in-office pulsed dye laser treatments to the upper aerodigestive tract. Otolaryngol Head Neck Surg. 2006; 134:1023-1027.
- Halum SL, Moberly AC. Patient tolerance of the flexible CO2 laser for office-based laryngeal surgery. J Voice. 2010; 24:750-754.
- Howell RJ, Schopper MA, Giliberto JP, Collar RM, Khosla SM. Office-based esophageal dilation in head and neck cancer: safety, feasibility, and cost analysis. Laryngoscope. 2018; 128:2261-2267.
- Franco RA, Jr. In-office laryngeal surgery with the 585-nm pulsed dye laser. Curr Opin Otolaryngol Head Neck Surg. 2007; 15:387-393.
- Marinone Lares SG, Allen JE. Safety of in-office laryngology procedures. Curr Opin Otolaryngol Head Neck Surg. 2019; 27:433-438.
- Belafsky PC, Kuhn MA. Office airway surgery. Otolaryngol Clin North Am. 2013; 46:63-74.
- Verma SP, Dailey SH. Office-based injection laryngoplasty for the management of unilateral vocal fold paralysis. J Voice. 2014; 28:382-386.
- Upton DC, Johnson M, Zelazny SK, Dailey SH. Prospective evaluation of office-based injection laryngoplasty with hyaluronic acid gel. Ann Otol Rhinol Laryngol. 2013; 122:541-546.
- Lippert D, Hoffman MR, Dang P, McCulloch TM, Hartig GK, Dailey SH. In-office biopsy of upper airway lesions: safety, tolerance, and effect on time to treatment. Laryngoscope. 2015; 125:919-923.
- Koszewski IJ, Hoffman MR, Young WG, Lai YT, Dailey SH. Office-based photoangiolytic laser treatment of Reinke’s edema: safety and voice outcomes. Otolaryngol Head Neck Surg. 2015; 152:1075-1081.
- Hoffman MR, Francis DO, Mai JP, Dailey SH. Office-based steroid injections for idiopathic subglottic stenosis: patient-reported outcomes, effect on stenosis, and side effects. Ann Otol Rhinol Laryngol. 2019:3489419889066.
- Postma GN, Goins MR, Koufman JA. Office-based laser procedures for the upper aerodigestive tract: emerging technology. Ear Nose Throat J. 2004; 83:22-24.
- Position statement: in-office photangiolytic laser treatment of laryngeal pathology. American Academy of Otolaryngology–Head and Neck Surgery. Available at: https://www.entnet.org/content/office-photoangiolytic-laser-treatment-laryngeal-pathology. Published March 2014. Accessed January 11, 2020.
- Sung CK, Tsao GJ. Single-operator flexible nasolaryngoscopy-guided transthyrohyoid vocal fold injections. Ann Otol Rhinol Laryngol. 2013; 122:9-14.
- Mallur PS, Rosen CA. Vocal fold injection: review of indications, techniques, and materials for augmentation. Clin Exp Otorhinolaryngol. 2010; 3:177-182.
- Amin MR. Thyrohyoid approach for vocal fold augmentation. Ann Otol Rhinol Laryngol. 2006; 115:699-702.
- Sulica L, Rosen CA, Postma GN, et al. Current practice in injection augmentation of the vocal folds: indications, treatment principles, techniques, and complications. Laryngoscope. 2010; 120:319-325.
- Naunheim MR, Woo P. Topical anesthetic techniques in office-based laryngeal surgery: a comparison of patient preferences. Laryngoscope. 2020; 130:166-170.
- Halderman AA, Bryson PC, Benninger MS, Chota R. Safety and length of benefit of restylane for office-based injection medialization-a retrospective review of one institution’s experience. J Voice. 2014; 28:631-635.
- Yung KC, Courey MS. The effect of office-based flexible endoscopic surgery on hemodynamic stability. Laryngoscope. 2010; 120:2231-2236.
- Morrison MP, O’Rourke A, Dion GR, Eller RL, Weinberger P, Postma GN. Hemodynamic changes during otolaryngological office-based flexible endoscopic procedures. Ann Otol Rhinol Laryngol. 2012; 121:714-718.
- Tierney WS, Chota RL, Benninger MS, Nowacki AS, Bryson PC. Hemodynamic Parameters during laryngoscopic procedures in the office and in the operating room. Otolaryngol Head Neck Surg. 2016; 155:466-472.
- Madden LL, Ward J, Ward A, et al. A cardiovascular prescreening protocol for unmonitored in-office laryngology procedures. Laryngoscope. 2017; 127:1845-1849.
- Anderson J, Bensoussan Y, Townsley R, Kell E. In-office endoscopic laryngeal laser procedures: a patient safety initiative. Otolaryngol Head Neck Surg. 2018; 159:136-142.