Humanitarian Travel Grant: Medical Mission in Ethiopia
I have been interested in global public health for some time and completed a master’s degree in public health as part of medical school. However, as I transitioned to residency, I became slightly jaded with regard to global health. Low-resource countries not only have a shortage of physicians, but also other services such as speech therapists, nurses, and audiologists.
By Nandini Govil, MD, MPH
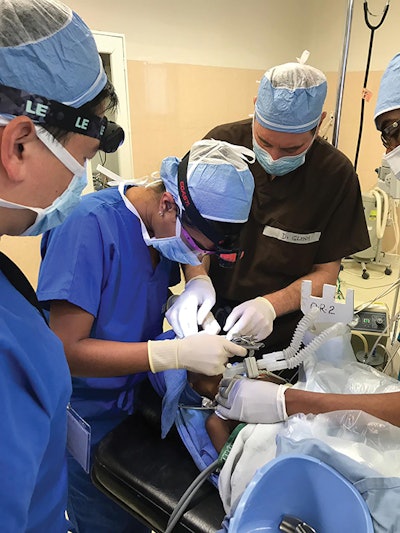
I have been interested in global public health for some time and completed a master’s degree in public health as part of medical school. However, as I transitioned to residency, I became slightly jaded with regard to global health. Low-resource countries not only have a shortage of physicians, but also other services such as speech therapists, nurses, and audiologists. As I progressed through medical training, I realized the value of these other health professionals. So how could I, as a solitary physician, make a difference?
I was quietly harboring some of these cynicisms about global health when I received the AAO-HNSF Humanitarian Travel Grant and traveled to Ethiopia with Healing the Children. I would like to tell you a story about a patient who made me reflect on my prior judgments. I will warn you: This is not your usual happy story.
This is the story of a three-year-old old named Aaron (name changed) who came to our clinic in the arms of his father. He had a tear-stained face, and we immediately noticed that he couldn’t turn his head due to an extremely large neck mass. Aaron had been a normal toddler until as recently as three months prior to seeing him. However, once his family started to notice his neck mass, his health also started to decline. He stopped being able to walk on his own. He then had trouble breathing, and the family took him to a local hospital where he had a tracheostomy. The hospital then heard that our group was in town and decided to send Aaron over for a second opinion.
We ultimately took him to the operating room to do a biopsy and discovered that the neck mass extended into his infratemporal mass and up through his ear canal. We all suspected before, but now it was confirmed. This mass was likely malignant, and Aaron’s prognosis was poor. The next day, we went to meet his family with an interpreter, and I remember thinking to myself, “It must be so odd and terrifying to hear the most terrible news of your life through an interpreter.” His mother and father heard what we had to say with sad, yet slightly relieved faces. Eventually, Aaron was transferred out to another radiation oncology facility. The relief on their faces was surprising and haunted me for some time.
I ultimately realized what I interpreted that look of their faces meant. Although we didn’t end up curing Aaron, we ended up diagnosing him with rhabdomyosarcoma. I realized that just putting a word to what their child was going through gave this family solace and power. They now had knowledge of what was happening, making the experience a little less scary. I discovered that the value in global health work comes from the power of knowledge that we provide patients. Even one lone physician can make a huge difference in this way.