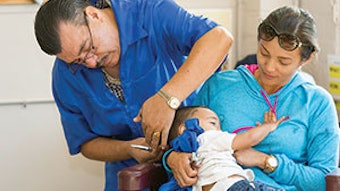
A life of service
When he was around age 70, Jerrold Polterock, MD, considered hanging up his otoscope. “That was 2008. I was thinking about retirement but that only lasted a few days,” quips Dr. Polterock. “So then I thought, ‘Okay, I’ll go out and do locum tenens.’

When he was around age 70, Jerrold Polterock, MD, considered hanging up his otoscope.
“That was 2008. I was thinking about retirement but that only lasted a few days,” quips Dr. Polterock. “So then I thought, ‘Okay, I’ll go out and do locum tenens.’ Once you do that though, your name is out there for recruiters.”
One thing led to another and eventually Dr. Polterock, who spent the majority of his career in San Bernardino, Los Angeles, and San Diego (with a brief stint in South Carolina), landed in Stanislaus County, CA, where he continues to practice.

The average afternoon for Dr. Polterock is seeing three to five patients. He also operates one day each week, averaging six to eight cases.
Dr. Polterock is on staff at a 25-bed hospital where he helps with the emergency room, though he rarely receives calls and if so, it’s usually for a consult.
“I say that I’ve discovered a way to retire and get paid for it. I’m out in a semi-rural community, at a hospital that doesn’t do trauma. You could do this falling off a log,” he says in jest. If he has any really big cases that come in, he sends them to UC Davis or UC San Francisco.
“I still do surgery, though I wouldn’t do a stapedectomy,” Dr. Polterock says with a pause, “Then again, I haven’t done a stapedectomy since 1974.”
That he is pleased to be serving right where he is was evident during a phone interview. “There are no extraordinary demands placed on me, and I’m doing a service for the community,” he says. “Where I’m at is not a huge county though Modesto is in it. I could guarantee you that I do 90 percent of all head and neck work in the county, maybe even more.” Some patients travel four hours to see him. “That may be great for your ego, but then you stop and think about it and realize there is nobody taking a Medicaid patient between you and four hours away.”
Asked about reimbursement frustrations or other business concerns, Dr. Polterock responds, “I haven’t looked at reimbursement, honestly speaking, since probably 1996. The reality is there’s nothing you can do about it. There’s no way you can fight with an insurance company. Any physician that’s out there and is going to war about reimbursement is knocking his own head against a wall. The only time I think you have an argument is if an insurer approves something and then later down the road denies it.” He finishes his point, “You gotta get the work done anyway.”
It’s clear. Dr. Polterock is in this for the patients.
He selected otolaryngology because he would get to see both sexes, all ages, and because it was fun. “And it has continued to be fun,” he interjects.
When he first started out and his own kids were little, he says that he preferred not to treat children. But now, if he could only see kids, he’d be elated. “They’re just the best,” he says.
Another draw for otolaryngology is that most patients get better. “Except for the occasional cancer case that you could never get ahead of, almost everybody gets better because it all boils down to you making the correct diagnosis and treating it. If I have someone come in, treat them and in a week or two, they’re not better. I change my diagnosis.”
He also has a deep respect for surgical relationships. “The only decision you have to make in medicine is whether you’re going to cut somebody or you’re not, and that just depends on your personality that was laid down when you were a little kid. You’re either aggressive enough to do that—and you know, it’s an extremely aggressive act, even if you’re doing it for therapeutic purposes—to cut somebody. So when you operate on somebody and they get better—that feedback—you’ve solved a problem for them for the rest of their life,” says Dr. Polterock. “You develop very personal relationships with the people that you’ve operated on. Even if you get somebody better medically, it’s just not the same connection as when you get somebody better surgically.”
Dr. Polterock feels fortunate to have seen and heard from otolaryngology pioneers. “For the people that trained at the same time as I did, the giants were still around, not only in otology, but in head and neck and in plastics. I think my generation was the last to benefit from that. I’m talking about the people that laid the ground for otolaryngology.”
In 1965, as a resident in Chicago, Dr. Polterock began a habit of taking in our Annual Meetings, which were held there at that time. He now claims to have attended more than 50 since then.
He recalls shortly after he first started practicing and doing outpatient surgeries, running into his former chief and telling him about outpatient tonsillectomies. “Chief thought that was just unbelievably outrageous. He just couldn’t imagine and now, that’s standard of care,” chuckles Dr. Polterock. He has always felt that outpatient procedures were a significant move forward in medicine.
Asked for wisdom to impart, Polterock remarks, “If residents love what they’re doing now, they can love it for the rest of their career. I play tennis, and I always tell the people that I play with: my ego gets fed first by my family, second by my profession, and tennis is a really poor third.”