Private practice will thrive
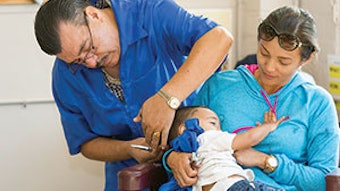
In this issue we spotlight Jerrold Polterock, MD, a semi-retired otolaryngologist practicing in California who has found a very satisfying way to remain active in a field he loves.
We have highlighted the diverse nature of otolaryngology practices across the United States in the “Practice Profile” feature in the Bulletin. In this issue we spotlight Jerrold Polterock, MD, a semi-retired otolaryngologist practicing in California who has found a very satisfying way to remain active in a field he loves. There are many veteran Members of our Academy who have taken advantage of opportunities such as this or are looking for similar ways to continue practicing. Challenges inherent in this type of practice are materially different than those faced by physicians practicing in larger groups or academic centers, particularly in the availability and depth of supporting resources.
I was recently privileged to attend and speak at the Large Group Executive Forum (LGEF), a component group of the Association of Otolaryngology Administrators (AOA), and experienced firsthand the cutting-edge strategies and allocation of resources that allow otolaryngologists to best serve their patients. The willingness to share “best practices” regarding such crucial issues as scheduling, compliance, reporting, and services provided gave me great confidence that the private practice of otolaryngology will not only survive but thrive in the future.
One of the driving forces behind the creation of our clinical data registry, RegentSM, was the realization that otolaryngologists, irrespective of their clinical situation and access to resources, will need to demonstrate and report on quality-based practice going forward. Regent will allow them to do that as well as allow the specialty to help define standards of clinical care rather than relying on other agencies to do so. The initial participation in the registry has been well beyond our expectations and is continuing to grow.
Single-use devices
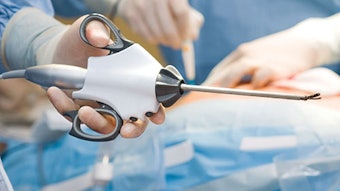
One of the feature articles in this month’s Bulletin concerns FDA deemed “single-use devices.” I would like to compliment and thank the group led by C. W. David Chang, MD, for this informative educational piece on a topic that cuts across multiple areas of our specialty. This document includes contributions from the diverse clinical areas and societies of otolaryngology that potentially would deal with this issue along with the Ethics, Patient Safety and Quality Improvement, and Medical Devices and Drugs committees, the 3P Advisory Group, and the FDA. This article informs our Members of the current landscape regarding these devices and how they are regulated.
Payers scrutinize common procedures
There seems to be a resurgence in the scrutiny applied to some of our more common procedures by payers across the country. Our Health Policy team has been working with the 3P Advisory Committee to provide cogent comments on potential policy changes by various insurers affecting some of our most common procedures such as fiberoptic flexible laryngoscopy, nasal and sinus endoscopy, functional endoscopic sinus surgery (FESS), balloon sinus ostial dilation (BSOD), and vocal fold injection for paralysis and glottic insufficiency. These proposals range from change in indications to change in pre-certification requirements and all the way to reclassification of long-standing, successfully performed procedures such as FESS and vocal injection for paralysis and glottic incompetency to “investigational.” There is an accelerating concern by payers related to BSOD, particularly ones performed in the office setting. As part of a collaborative effort with the American Academy of Otolaryngic Allergy and the American Rhinologic Society, Joseph Han, MD, led a special project to revise our Position Statement on BSOD, which was approved at the September Board of Directors meeting and is posted on our website. As part of a longer-term strategy, a Consensus Statement will also be considered. Recently, in Pennsylvania and Delaware there have been requests for refunds from our Members of up to three years for in-office BSOD. It is clear that the specialty must take the lead in establishing reasonable indications based on evidence for this procedure or others will do it for us.
Perhaps the most concerning of all of these above-mentioned issues was the proposed reclassification of FESS as investigational after more than 30 years of use. Several senior rhinologists worked with our Health Policy staff to produce an evidence-laden reply documenting multiple studies validating the utility and value of the procedure. We will use the same model with senior laryngologists to respond to a similar change proposed for vocal injection for paralysis.
It is critical that we receive input from our Members across the country when changes are recognized relating to insurer policies so we can be on board early. With your help, we will continue to work aggressively to protect our patients and the ability to perform procedures that give them benefit.