Challenging Bronchoscopy: Dos and Don’ts for a Successful Procedure
In September 2019, during the AAO-HNSF Annual Meeting & OTO Experience in New Orleans, we presented an airway panel titled, “Challenging Bronchoscopy: Dos and Don’ts for a Successful Procedure.” Our target audience was diverse—the resident-in-training, the physician on call and covering for airway emergencies, as well as the airway expert interested in simulation as an educational tool.
Michel N. Nassar, MD, Kaalan E. Johnson, MD, Charles M. Myer IV, MD, Evan J. Propst, MD, MSc, Scott M. Rickert, MD, and Christina J. Yang, MD
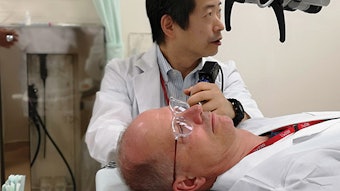
In September 2019, during the AAO-HNSF Annual Meeting & OTO Experience in New Orleans, we presented an airway panel titled, “Challenging Bronchoscopy: Dos and Don’ts for a Successful Procedure.” Our target audience was diverse—the resident-in-training, the physician on call and covering for airway emergencies, as well as the airway expert interested in simulation as an educational tool. The idea was simple—ask airway experts to share challenging cases with the audience and how they managed those cases. The other members of the panel were simultaneously running an airway simulation, projected on two large screens (Figure 1). This allowed the audience to think about the case, see a live demonstration of said case, and interact in real-time with the panel.
 Figure 1
Figure 1But what renders a bronchoscopy procedure challenging? Several factors, in fact.
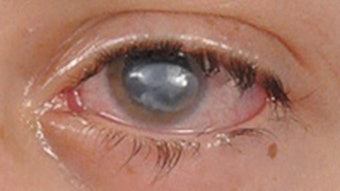
Some are linked to the pathology itself. Take an airway foreign body as an example. It occurs up to 2.5 million times each year in the United States and may result in as many as 2,000 deaths.1 The combined rate of mortality or anoxic brain injury to those patients hovers around 4%.2 The nature of the foreign body (i.e., round bead), the location in a distal bronchus with difficult access, the potential for bleeding, and airway edema are all to be considered and prepared for. Another example can be hemorrhage resulting from an intraluminal mass biopsy or a draining empyema resulting in significant amounts of purulent material. The endoscopist will need to juggle the need to ventilate (aggressive suctioning, possible selective main stem intubation if the bleeding source is from the opposite side) and to establish hemostasis (endotracheal tube cuff to apply pressure against the bleeding source, use of local vasoconstrictors or cautery).
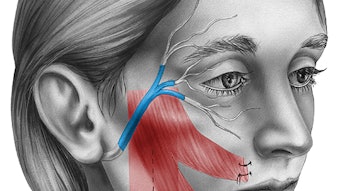
Other factors are patient-related. It is not uncommon for the craniofacial patient to present with micrognathia/retrognathia, midface retrusion, and macroglossia, and that may lead to oral/oropharyngeal airway obstruction and issues with exposure, ventilation, and visualization. It is exceptionally important to optimize laryngoscope and bronchoscope (rigid or flexible) placement in order to have a successful airway evaluation and/or intervention. There are many techniques to help visualize an airway, and it is important to feel comfortable with both rigid and flexible options as they may be needed in these challenging cases. One must remember that every complex airway is unique and a small, subtle adjustment can have a large impact on the success of the surgery.
Finally, a challenging bronchoscopy can sometimes be self-inflicted. Seemingly straightforward bronchoscopies can become challenging due to factors such as inadequate team training, equipment unavailability, infrastructure, and poor communication among OR staff, anesthesiology, and otorhinolarynology team members. Training and preparing for an airway emergency are of utmost importance. Simulation can supplement clinical exposure and provide a safe learning environment for self-paced practice. Thus, bronchoscopy simulation is a major component in boot camps, intensive courses that have been shown to improve self-assessment of confidence,3,4 knowledge,5 and proficiency.6 Various models and modalities including mannikins, animal models, 3D printed models, and virtual reality can be utilized for standard rigid bronchoscopy, foreign body removal, and advanced endoscopic procedures.
Simulation prior to bronchoscopy has become even more essential during the global COVID-19 pandemic. Additional personal protective equipment (PPE) such as N95 masks, goggles, face shields, and impermeable gowns can lead to sweating, fogging, neck discomfort, CO2 retention, and headache. Powered air-purifying respirators (PAPR) are more comfortable to wear but the blowing air makes communication difficult. Added concerns about donning PPE, especially in emergent situations, can be cognitively taxing. Additional drapes placed over patients to minimize the spread of droplets can make sharing the airway with the anesthesiologist confusing. Early collaborative multidisciplinary simulation is essential to identify and mitigate potential issues and improve situational awareness and team dynamics. Checklists and surgical pauses are even more important during these cases. For academic centers, surgical education during the COVID-19 pandemic has been difficult due to distancing requirements, limitations on the number of personnel in the operating room, and requirements for the staff surgeon to perform the case to shorten the duration of droplet exposure.
Airway simulation is essential for surgical education as well as team-building efficiency. It is uniquely positioned to train and prepare for a high acuity, low-frequency event such as airway bronchoscopy.
A special thanks to the AAO-HNSF and the Simulation Committee for their sponsorship and support.
Presented at the AAO-HNSF 2019 Annual Meeting & OTO Experience in New Orleans, LA
References
- Karatzanis AD, Vardouniotis A, Moschandreas J, et al. The risk of foreign body aspiration in children can be reduced with proper education of the general population. Int J Pediatr Otorhinolaryngol. 2007; 71(2):311-5.
- Jacquelyn R Sink, Dennis J Kitsko, Matthew W Georg, Daniel G Winger, Jeffrey P Simons. Predictors of Foreign Body Aspiration in Children. Otolaryngol Head Neck Surg. 2016;155(3):501-7.
- Malekzadeh S et al. ORL Emergencies Boot Camp: Using Simulation to Onboard Residents. Laryngoscope. 2011 Oct;121(10):2114-21. doi: 10.1002/lary.22146. PMID: 21898435
- Jabbour N et al. Psychomotor Skills Training in Pediatric Airway Endoscopy Simulation. Otolaryngol Head Neck Surg. 2011 Jul;145(1):43-50. doi: 10.1177/0194599811403379. PMID: 21493270
- Amin MR, Friedmann DR. Simulation-based Training in Advanced Airway Skills in an Otolaryngology Residency Program. Laryngoscope. 2013 Mar;123(3):629-34. doi: 10.1002/lary.23855. PMID: 23404777
- Gorthey S, Bitners A, Rong E. Gibber M, Yang CJ. Impact of PGY-1 boot camp on procedural skill development. Presented at Triologic Society/COSM. May 4, 2019. Austin, TX.