Sustainable Surgical Outcomes in the Pediatric Airway: The Operation Airway Experience
As a surgeon there is nothing more gratifying than using your own skill set to perform complex airway reconstruction and allowing children to breathe, speak, and ultimately rediscover their livelihood again. At Operation Airway, however, the goal of the teaching surgeon is quite the opposite.
Asitha Jayawardena, MD, MPH; Jose Bonilla, MD; Marcos Mirambeaux, MD; Evelyn Zablah, MA; Christopher Hartnick, MD, MS
As a surgeon there is nothing more gratifying than using your own skill set to perform complex airway reconstruction and allowing children to breathe, speak, and ultimately rediscover their livelihood again. At Operation Airway, however, the goal of the teaching surgeon is quite the opposite. By the end of the mission, or series of missions, the goal is ultimately to be able to participate solely as an observer, watching the local team navigate through complex decision-making and technically challenging cases. At the end of the mission, the less operating that is necessary for the teaching surgeon to do, the better.
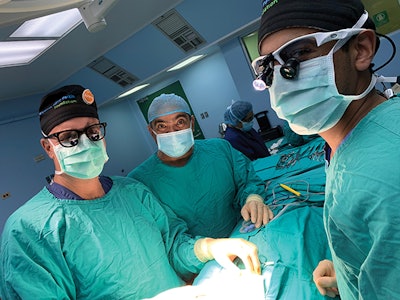 Christopher Hartnick, MD, of MEEI; Jose Bonilla, MD, of Bloom Hospital, El Salvador; and Asitha Jayawardena, MD, of MEEI conducting laryngotracheal reconstruction.
Christopher Hartnick, MD, of MEEI; Jose Bonilla, MD, of Bloom Hospital, El Salvador; and Asitha Jayawardena, MD, of MEEI conducting laryngotracheal reconstruction.This philosophy has guided Operation Airway’s strategy over the past 10 years. A careful program of surgical teaching that relies on graduated autonomy and discipline-to-discipline teaching has allowed two countries to have “graduated” from the program into conducting pediatric airway surgeries in a safe, effective manner.
This thoughtful, surgical teaching program relies on a carefully vetted team of pediatric otolaryngologists, pediatric anesthesiologists, pediatric intensivists, speech-language pathologists, respiratory technicians, and nursing staff. Airway surgery is inherently a team sport, meaning that a supremely skilled surgeon still relies on high-quality intensive care, anesthesia, respiratory, and nursing teams to manage the postoperative course of the airway reconstruction.
To that end, a multidisciplinary technology-based teaching module has been created and utilized to obtain optimal outcomes. Each teaching module is available in multiple languages and accessible at all times via QR codes. The QR codes themselves are placed at the patient’s bedside so any practitioner with specific questions can have them answered in real time.
Sustainable surgical approaches are the focus of these missions, with airway tools being constructed out of local resources (e.g., tube within a tube, needle cricothyrotomy kits). In fact, we have learned from our colleagues in other countries and use a portable, handheld suction for patient/family use in the postsurgical airway. This allows the local practitioners to feel that they can conduct safe surgeries even after the teaching team leaves.
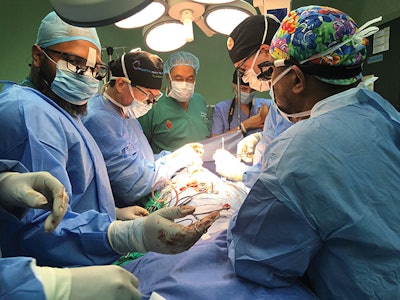 Marcus Mirambeaux, MD, of the Dominican Republic and Christopher Hartnick, MD, of MEEI conducting a slide tracheoplasty.
Marcus Mirambeaux, MD, of the Dominican Republic and Christopher Hartnick, MD, of MEEI conducting a slide tracheoplasty.Measuring long-term surgical outcomes is imperative in mission trips, and too many teams fail to do this adequately. We now utilize a homegrown electronic medical record system that allows, for example, operative reports and follow-ups to be directly uploaded into the system. This facilitates multidisciplinary communication and allows prompt end-of-mission summaries to be created for the local teams. Lastly, this facilitates scrutiny of our team’s postsurgical outcomes.
Thus far, we have conducted 14 missions in Ecuador, El Salvador, and the Dominican Republic.1 A total of 135 procedures have been performed on 90 patients. Thirty-six of those procedures were laryngotracheal reconstruction. A decannulation rate of 82% has been achieved, and two countries—Ecuador and the Dominican Republic—have graduated from the program. Achieving specific graduation criteria suggests that a country is now able to perform complex pediatric airway reconstruction (laryngotracheal reconstruction with rib graft, tracheal resection, slide tracheoplasty, etc.) autonomously.
Although this is a surgery-centered effort, our interventions are not limited to surgery alone. A retrospective review of our data revealed that the pediatric intensive care unit (ICU) in one of our hospitals had a mortality of 27% for all admitted non-airway patients. Further review found that the team needed education in appropriate securement of endotracheal tubes and management of a cuffed endotracheal tube. A multidisciplinary education effort reduced accidental extubation rates in the ICU by nearly 50% and dropped mortality by 4%. The cost-effective intervention was only $1.32 per patient and therefore about $30.70 per life saved. This intervention would only be possible with thorough review of the reported outcomes, philanthropic donations (Thank you, Benjamin Harry Peikin Foundation!), curiosity of the investigators, and an enormous effort by the local teams to improve their own outcomes.
Local support is imperative and the crux of Operation Airway’s success. Local surgical leaders help our team navigate the complexity of an international healthcare system and facilitate the growth of national airway programs within each country. Furthermore, the training of local surgical trainees is an important aspect of each mission. Residents of all levels participate in experience-appropriate aspects of the surgeries. Surgical leaders of graduated programs often teach in other countries and help share local pearls and pitfalls to facilitate success.
The surgical learning that occurs on these trips is by no means a unilateral effort. We learn as much from local surgeons in low-resourced settings about management using limited resources as they learn from us regarding surgical techniques.
One of the most rewarding aspects of participating on these trips, however, is not the surgical experience. Rather, it’s handing the reigns over to local, junior surgeons and observing as they complete a complex pediatric airway operation, needing you for only the celebratory high five at the end of the case. The friendships, mentorships, and partnerships are priceless.
More information regarding our team and our efforts can be found here: https://www.operationairway.com/
This topic was presented as part of the International Symposium of the AAO-HNSF 2020 Virtual Annual Meeting & OTO Experience.
References:
- Jayawardena ADL, Ghersin ZJ, Mirambeaux M, et al. A sustainable and scalable multidisciplinary airway teaching mission: the Operation Airway 10-year experience. Otolaryngol Head Neck Surg. 2020. doi: 10.1177/0194599820935042