Shaping healthcare policy
May is Better Hearing and Speech month. In the April Bulletin, we highlighted the recent evolution of the hearing aid market place in the United States. As we continue to follow changes closely, we must remain cognizant that we can do more to highlight preventable causes of hearing loss through public educational campaigns.
 James C. Denneny III, MD
James C. Denneny III, MD
AAO-HNS/F EVP/CEO
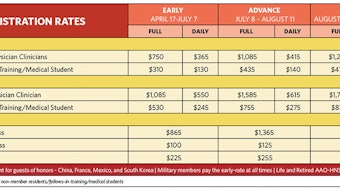
Registration opens this month for our 121st Annual Meeting & OTO Experience in Chicago, IL. This promises to be an exceptional educational opportunity with increased CME/CE offerings. As part of registration, all attendees will have access to the AcademyU library of recorded 2017 sessions, an electronic version of all meeting presentations, allowing them access to sessions they were previously unable to attend, and an opportunity for up to 50 additional CME credits. This package will also be available after the meeting for those who were unable to attend. Our keynote speaker at the Opening Ceremony, Daniel Kraft, MD, will present his thoughts on “The Future of Health and Medicine: Where Can Technology Take Us?” We will also have an outstanding group of speakers for the Conley, Cotton-Fitton, House, Myers, and Neel Lectures. The International Symposium will be expanded this year, and CME credit will be available for U.S. attendees of these diverse international sessions. I encourage you to register during the early registration period to get the most value from the meeting as well as securing the hotel of your choice.
MACRA and MIPS
Foremost in the minds of all involved in the healthcare profession and industry is the legislative and regulatory process relating to MACRA and the Affordable Care Act (ACA) “repeal and replace” activity. This, combined with the implementation phase of the Merit-based Incentive Payment System (MIPS) has created significant, justifiable anxiety for all participants in the healthcare system. We will continue to advocate on both the legislative and regulatory fronts for policies and laws based on principles of access, affordability, quality, and reduced administrative burden. The current ACA contains upward of 1,400 regulations that the new secretary of Health and Human Services (HHS) can change unilaterally. The Academy along with the house of medicine will continue to work with the secretary to relieve physicians of some of the burdensome provisions of the ACA that contribute to the burgeoning problem of “burnout” that is affecting healthcare workers at all levels.
While the Academy and its members may not agree with the concepts and details of the implementation of MIPS, we must continue to educate our members on how to participate and give them the tools to do so. That will not stop us from working to improve the system and ease the burden of participation for our members. The “transition year” announced by CMS is a direct result of continuous discussion and recommendation by the house of medicine, including otolaryngology. The transition to quality and value-based payment will continue. Our goal is to make that as easy as possible for our members through products like Reg-ent℠ while we continue to work for improvement in the system.
The evolution of the value-based payment system was dictated by the projection that overall healthcare spending would approach 25 percent of the gross domestic product by 2030, a level that the United States is unwilling and unable to sustain. Attempts to solve this problem have and will continue to result in the opportunity to improve upon policy and statutes that dictate the way we practice. This will be a marathon rather than a sprint. We depend on input from our members to identify specific areas that are not working well and do not benefit patients and further suggest ways to create a better system. Working with other stakeholders in the provider community to effect positive changes will allow us the opportunity to succeed where we would not be able to on our own.