Fact Sheets: Post-SGR Payment Policy: APMs
MACRA replaced the Sustainable Growth Rate (SGR) and created the Merit-based Incentive Payment System (MIPS) and the Advanced Alternative Payment Model (APM) program. The proposed start date for the Advanced APM program is January 1, 2017.
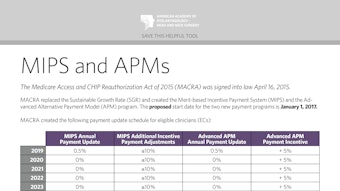
The Medicare Access and CHIP Reauthorization Act of 2015 (MACRA) was signed into law April 16, 2015.
MACRA replaced the Sustainable Growth Rate (SGR) and created the Merit-based Incentive Payment System (MIPS) and the Advanced Alternative Payment Model (APM) program. The proposed start date for the Advanced APM program is January 1, 2017.
Alternative payment models are a form of payment reform that incorporate quality and total cost of care into reimbursement rather than a traditional fee-for-service structure. Eligible clinicians (ECs) that participate in a CMS-defined Advanced APM may be exempted from MIPS reporting.
The Advanced APM program creates the following distinctions between different APMs:
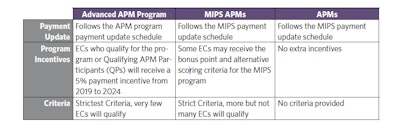
- Qualifying APM Participants (QPs): QPs are ECs who meet the minimum percentage of patients or payments through an Advanced APM and are eligible to participate in the Advanced APM program.
- All QPs in the Advanced APM program will receive a 5% payment incentive from 2019 until 2024.
- The payments for QPs will be based off claims reported during the reporting periods, which will occur 2017-2022.
- Academy advocacy: The Academy has a history of working closely with regulatory agencies to maintain our visibility and credibility with national representatives regarding federal regulatory issues.
- The Advanced APM requirements outlined in the proposed rule would only allow a very limited group of physicians to be held exempt from MIPS reporting by meeting the minimum percentage of patients or payments through an Advanced APM.
- The Academy is actively advocating on Members’ behalf to work with CMS to expand the definition to be closer in line with the intent of the law.
To learn more visit, www.entnet.org/content/alternative-payment-models.
Download a pdf of “Post-SGR Payment Policy: APMs.”