Fact Sheets: MIPS and APMs
MACRA replaced the Sustainable Growth Rate (SGR) and created the Merit-based Incentive Payment System (MIPS) and the Advanced Alternative Payment Model (APM) program. The proposed start date for the two new payment programs is January 1, 2017.
The Medicare Access and CHIP Reauthorization Act of 2015 (MACRA) was signed into law April 16, 2015.
MACRA replaced the Sustainable Growth Rate (SGR) and created the Merit-based Incentive Payment System (MIPS) and the Advanced Alternative Payment Model (APM) program. The proposed start date for the two new payment programs is January 1, 2017.
MACRA created the following payment update schedule for eligible clinicians (ECs):
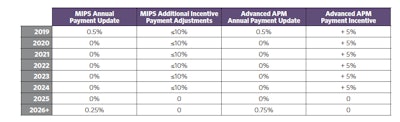
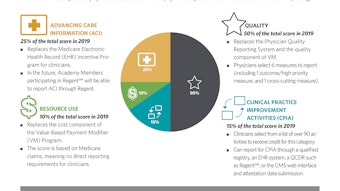
- MIPS: Under MIPS, a majority of eligible clinicians (ECs) will report on four categories that will add up to a composite performance score (CPS):
- Quality
- Advancing Care Information (ACI)
- Clinical Practice Improvement Activities (CPIA)
- Resource Use
The CPS will be used by CMS to determine whether or not an EC will receive a bonus payment or will be subject to a payment reduction.
- Advanced APM program: Alternative payment models are a form of payment reform that incorporate quality and total cost of care into reimbursement rather than a traditional fee-for-service structure.
- Eligible clinicians (ECs) that successfully participate in a CMS-defined Advanced APM may be exempted from MIPS reporting and receive a 5 percent incentive payment.
- Academy advocacy: To allow Members more time to learn and adapt their practice patterns to MIPS and APM reporting, the Academy is actively advocating for a later reporting period.
We have established Regent℠, a qualified clinical data registry (QCDR), which will:
- Help Members navigate evolving payment models and quality programs
- Focus on longitudinal perspective of clinical care
- Inform healthcare at a national level through clinical research
- Assist with satisfying Maintenance of Certification needs for Members
- House measures across all specialties of otolaryngology-head and neck surgery
To learn more visit, www.entnet.org/content/alternative-payment-models.
Download a pdf of “MIPS and APMs.”