Eosinophilic Esophagitis: Implications for the Otolaryngologist
Eosinophilic esophagitis (EoE) is a clinicopathological disorder characterized by eosinophil predominant inflammation of the esophagus (>15 eosinophils/hpf) and esophageal dysfunction. The prevalence in children in the United States is 10-50/100,000 and EoE has become increasingly recognized in children and adults over the past two decades.
Margo McKenna Benoit, MD; Mathieu Bergeron, MD; Anatoli F. Karas, MD; Esther Prince, MD; and John J. Faria, MD
Eosinophilic esophagitis (EoE) is a clinicopathological disorder characterized by eosinophil predominant inflammation of the esophagus (>15 eosinophils/hpf) and esophageal dysfunction. The prevalence in children in the United States is 10-50/100,000 and EoE has become increasingly recognized in children and adults over the past two decades. The disease is characterized by periods of remission and relapses and includes vague presenting symptoms, making it difficult to diagnose. Due to its nonspecific presentation, up to 15% of patients with EoE may initially present to an otolaryngologist, therefore making it an important differential diagnosis in our clinics.
Presenting symptoms vary with age. Infants and toddlers typically present with feeding difficulties, vomiting, food refusal, or failure to gain weight. School-aged children will usually present with vomiting, regurgitation, and abdominal pain, while adolescents will tend to present with food impaction, dysphagia, and abdominal pain. However, patients with EoE develop coping mechanisms to compensate for their symptoms. It is of utmost importance to keep a high degree of suspicion and to question any changes in food habits. Changes in food habits include cutting food into smaller pieces, pocketing of food in the mouth, or drinking larger amounts of liquids with meals to help alleviate symptoms. A personal or atopic family history such as atopic dermatitis, asthma, eczema, or IgE-mediated food allergies, as well as family history of EoE, should increase the clinical index of suspicion for EoE. Atopic disorders and EoE are thought to share similar underlying mechanisms.
While EoE usually presents with gastrointestinal symptoms, it can also have extraesophageal manifestations refractory to conventional treatment. Several otolaryngologic symptoms are associated with EoE, and these may be the initial presenting symptoms in the absence of traditional gastrointestinal symptoms. Nasal symptoms and rhinosinusitis are reported in up to 25% of children with EoE. To a lesser extent, the same applies for laryngeal symptoms (chronic cough, hoarseness, dysphonia), recurrent laryngotracheobronchitis (croup), and other airway manifestations such as “active airway” or failed airway reconstruction. Of note, it is now a standard of care to rule out EoE prior to attempting laryngotracheal reconstruction as such disorder doubles the odds of a failed reconstruction. It has also been noted that patients with EoE are more likely to undergo ENT surgery. For example, 15% of patients with EoE will have bilateral myringotomy with tubes versus 6.8% of the general population. Up to 30% of patients with EoE will require multiple sets of tubes, which represents approximately 10% more than the general population.
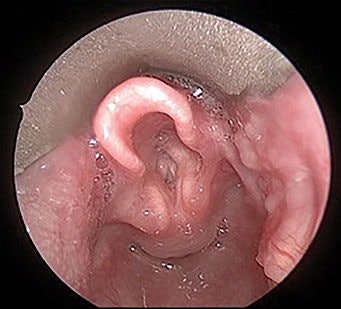
Revised diagnostic criteria for EoE were published in 2018, refining presenting symptoms and the role of esophageal biopsies. More importantly, the diagnostic algorithm removed the need for the use of proton pump inhibitors (PPI) prior to performing an EGD. It was felt that PPIs were better classified as treatment of EoE rather than part of the diagnostic criteria. EoE should be suspected on a clinical basis with chronic symptoms of esophageal dysfunction such as food impaction, heartburn, abdominal pain, and/or cough. When EGD is indicated, the examination should focus on endoscopic signs of EoE, such as longitudinal furrowing, esophageal rings, edema, exudates, or strictures. It is also recommended to quantify the findings using a validated tool, like the EoE Endoscopic Reference Score. Normal mucosa does not exclude EoE. During an EGD, esophageal biopsies should be taken whenever EoE is suspected. EoE is considered a patchy disease and 2-4 biopsies should be taken from the proximal and distal esophagus focusing on areas that appear suspicious. A diagnosis of EoE is made when biopsies demonstrate greater than 15 eosinophils/hpf and the patient has symptoms compatible with this disorder. Of note, the presence of esophageal eosinophilia on biopsies without the presence of symptoms of EoE does not necessarily lead to its diagnosis. All patients with esophageal eosinophilia should be evaluated for other causes of esophageal eosinophilic. These conditions include gastroesophageal reflux and Crohn’s disease as well as other diseases.
EoE management includes both medical and dietary therapies. PPI and swallowed steroids (budesonide and fluticasone) are the cornerstone of the medical treatment. Swallowed fluticasone has demonstrated to improve symptoms and histology with uncommon and often mild side effects (candida overgrowth). Biological therapy demonstrated some histological benefit, especially those that targeted the Th2 axis.
Dietary therapy should be considered and discussed in all patients with a diagnosis of EoE. Consultation with a dietician is highly recommended. Therapy options may include a total elimination diet (amino acid-based formula), selective elimination diet (eliminating major food allergens), and directed diet (eliminating foods based on allergy skin testing). The use of dietary therapy may lead to complete or near-complete resolution of both clinical and histological abnormalities. A response to any treatment supports but is not required for diagnosis.
EoE is a complex disorder with a non-specific presentation and affects a wide range of ages. Investigation and treatment require a multidisciplinary approach, with a pivotal role from a dietician, gastroenterologist, and allergist. Otolaryngologists should consider EoE whenever a patient presents refractory aerodigestive symptoms unresponsive to conventional treatment.
References
- Furuta, G.T.L., C. A.; Collins, M. A., Eosinophilic Esophagitis in Children and Adults: A Systematic Review and Consensus Recommendations for Diagnosis and Treatment. Gastroenterology, 2007. 133.
- Lynch, M.K., et al., Topical Review: Eosinophilic Esophagitis in Children: Implications for Health-Related Quality of Life and Potential Avenues for Future Research. J Pediatr Psychol, 2015. 40(8): p. 727-32.
- Thompson, D.M. and L.J. Orvidas, Otorhinolaryngologic manifestations of eosinophilic esophagitis. Gastrointest Endosc Clin N Am, 2008. 18(1): p. 91-8; ix.
- Dellon et al. Updated International Consensus Diagnostic Criteria for Eosinophilic Esophagitis: Proceedings of the AGREE Conference. Gastroenterology 2018;155:1022-1033.
- Ko E, Chehade M. Biological Therapies for Eosinophilic Esophagitis: Where do we stand? Clin Rev Allergy Immunol. 2018 Oct;55(2):205-216.
- Patel, RV, Hirano,I. New Developments in the Diagnosis, Therapy and Monitoring of Eosinophilic Esophagitis. Curre Treat Options Gastroenterol. 2018 March ;16(1):15-26.
- Hudson S, Sampson C, Muntz HR, Jackson WD, Smith ME. Foreign body impaction as presentation of eosinophilic esophagitis. Otolaryngol Head Neck Surg. 2013. Nov;149:679-81
- Kelly EA, Linn D, Chun RH, Keppel KL, Noel RJ. Otolaryngologic surgeries are frequent in children with eosinophilic esophagitis. Ann Otol Rhinol Laryngol. 2015. May; 124-355-360