COVID-19 and Racial Disparities: An Update
Early in the pandemic, the widespread, disproportionate impact of COVID-19 was evident among minorities, particularly Hispanic, Black, and Native American communities in the United States. This has been repeatedly demonstrated through different types of analyses, including evaluations of relative cases, hospitalizations, and deaths.

Zainab Farzal, MD, MPH, SRF Chair, and Kevin J. Contrera, MD, MPH, SRF BOG Governor
Early in the pandemic, the widespread, disproportionate impact of COVID-19 was evident among minorities, particularly Hispanic, Black, and Native American communities in the United States. This has been repeatedly demonstrated through different types of analyses, including evaluations of relative cases, hospitalizations, and deaths. For instance, the Centers for Disease Control and Prevention (CDC) reported that non-Hispanic Black, Hispanic or Latino, and non-Hispanic American Indian or Alaska Native persons were hospitalized at rates approximately five times that of non-Hispanic White persons.1 The data primarily focused on adult patients particularly since pediatric cases were initially rare. A pediatric study published in The New England Journal of Medicine in late July 2020 demonstrated a similar disparate incidence of a condition known as multisystem inflammatory syndrome in children (MIS-C). A diagnosis of MIS-C was made if certain criteria were met, including age under 21 years, fever >38°C lasting over 24 hours, multisystem (two or more) organ involvement, increase in inflammatory markers, and lab confirmation of SARS-CoV-2 infection. Conducted across 53 academic centers around the country, 61% of the patients were either Black or Hispanic non-White.2 Nearly all patients (73%) were previously healthy, but 71% also involved four or more organ systems.2
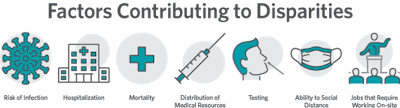
The data from the pediatric study highlight the intertwinement of comorbidities, systemic racism, and public health in the United States. Certain underlying conditions such as diabetes and cardiovascular disease put individuals at risk for COVID-19 and are disproportionately more common among people of color. However, the unequal incidence of COVID-19 among otherwise healthy children of color best highlights other, more deep-rooted, systemic risk factors. These include discrimination in testing, insurance status, or medical utilization. Additionally, many risks faced by people of color are occupational, pertaining to jobs with an inability to work from home, or socioeconomic such as living in more dense areas that limit families’ ability to socially distance. Unless these root causes of health-related disparities are addressed, efforts toward reducing comorbidities alone will minimally diminish the impact of health crises like COVID-19. As trainees and future healthcare leaders, we must be patient and be public health advocates battling these systemic inequities head on.
References
- Centers for Disease Control and Prevention, National Center for Immunization and Respiratory Diseases. COVIDView: a weekly surveillance summary of the U.S. COVID-19 activity. Updated September 4, 2020. Accessed September 7, 2020. https://www.cdc.gov/coronavirus/2019-ncov/covid-data/covidview/index.html
- Feldstein LR, Rose EB, Horwitz SM, et al. Multisystem inflammatory syndrome in U.S. children and adolescents. N Engl J Med. 2020;383(4):334-346. doi:10.1056/NEJMoa2021680