American Head & Neck Society
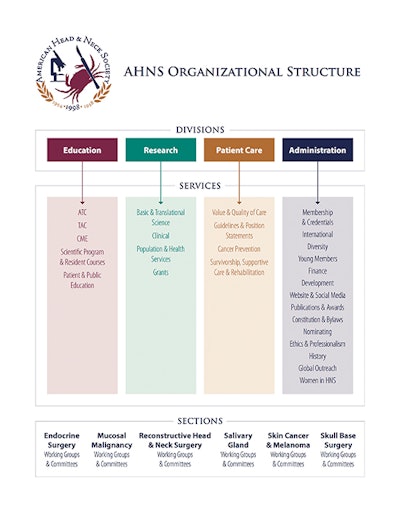
The American Head & Neck Society (AHNS) is a vibrant society committed to being patient centric, collaborative, innovative, ethical, value based, and global. To maximize member engagement, AHNS restructured to have sufficient organizational capacity in achieving their mission (as displayed in the graphic). So what are the challenges and opportunities in practice and patient care?
Christine G. Gourin, MD, MPH, and Richard J. Wong, MD, AHNS Scientific Program/Resident Courses Service members, Cherie-Ann O. Nathan, MD, AHNS President

The “face” of head and neck cancer in 2020 has changed, with fewer tobacco-related cancers and an increasing number of HPV-related oropharyngeal, thyroid, and skin cancers. The HPV-related oropharyngeal cancer epidemic is associated with a growing cohort of long-term survivors. Deintensification of radiation and/or chemotherapy can be accomplished with transoral surgery in patients without evidence of extranodal extension and clear margins, all being studied in globally initiated multidisciplinary clinical trials. Surgeon-initiated trials include elective versus therapeutic neck dissection in node negative oral cavity cancer and the E3311 transoral surgery study, with a postoperative radiation deintensification arm.
Immunotherapy and targeted therapy show promise for advanced skin and head and neck mucosal cancers, with a better tolerated side effect profile. Melanoma mortality rates have started to decline for the first time in decades. The U.S. Food and Drug Administration approved cemiplimab for advanced cutaneous squamous cell cancer and hedgehog inhibitor for advanced basal cell carcinoma. In recurrent mucosal head and neck cancer, response rates with immunotherapy are 10%-20%. Neoadjuvant immunotherapy trials are underway to determine the role of immunotherapy in primary treatment for mucosal disease.
Active surveillance is increasingly recognized as a safe option for patients with low-risk thyroid cancers that are favorably located and without metastases. Molecular analysis of FNA samples can determine the relative risk of malignancy. Targeted therapy now exists for medullary and anaplastic thyroid cancer based on molecular profiling. RET-mutated medullary thyroid cancers have response rates of 60%-70% range to the new RET inhibitors LOXO-292 and BLU-667. Anaplastic thyroid cancers with BRAF mutations have a response rate of 69% to combination BRAF and MEK inhibition. This is a dramatic improvement over prior ineffective therapies for a disease viewed as fatal.
As patients with head and neck cancer live longer, survivorship issues are increasingly important. Multidisciplinary care is required to address lymphedema, dysphagia, dental issues, surveillance, new primaries, and radiation-induced malignancy. Speech-language pathology-directed swallowing exercises during and after treatment reduce the incidence of late dysphagia. Salvage surgery is associated with increased morbidity and mortality and often requires reconstruction and complex decision making. The opioid epidemic has led to unintended consequences of pain management for patients who suffer protracted pain from treatment. The management of head and neck cancer continues to evolve with the changing disease landscape, the emergence of new technologies and therapies, and a stronger emphasis on optimizing quality of life.
The COVID-19 pandemic presents an entirely new set of challenges. How do we prioritize care during this pandemic? How do we protect our staff during procedures that may aerosolize virus, particularly in mucosal sites that carry high viral loads? How can telemedicine allow us to best connect remotely with our patients? The AHNS website’s COVID-19 Bulletin Board is an outstanding resource that addresses many of these issues.