A Practical Guide to Collaborative Pediatric Dysphagia Assessment
An otolaryngology-speech language pathology partnership is a smart approach to evaluating, diagnosing, and treating pediatric dysphagia.
Ashley L. Miller, MD, on behalf of the Airway and Swallowing Committee in collaboration with Amy Manning, MD, Prasanth Pattisapu, MD, MPH, and Maleah Blake, MA, CCC-SLP

June is National Dysphagia Awareness Month. In June 2025, Pamela A. Mudd, MD, MBA, and Nancy M. Bauman, MD, described the role of the otolaryngologist in identifying causes for dysphagia amenable to surgical treatment and emphasizing the need for multidisciplinary collaboration, which we will explore more in this article.
Speech Language Pathology and Otolaryngology Collaboration
Patients referred to an otolaryngologist for dysphagia evaluation present with a wide range of manifestations depending on age and overall level of severity. A comprehensive history and physical examination, often including flexible nasal laryngoscopy, is essential to further delineate the evaluation and treatment plan. During the initial visit, care is taken to assess which stage(s) of swallowing area may be impacted: oral, pharyngeal, esophageal, or multiple areas.
If not already in place, a referral to speech language pathology is of high utility in this patient population. In academic and tertiary referral centers, the otolaryngology-SLP partnership is often well-established; in other settings, face-to-face/direct communication may be more limited.
Following a clinical assessment of swallowing by the SLP, instrumental assessments of swallowing may be considered for further detailed characterization of swallow function. Oropharyngeal dysphagia is primarily evaluated with videofluoroscopic swallow studies (VFSS) (also referred to as modified barium swallow study, or MBSS) and flexible endoscopic evaluation of swallowing (FEES). Additional instrumental assessments of dysphagia include high-resolution pharyngeal and/or esophageal manometry, esophagram and/or upper GI studies, and pH impedance testing.
Instrumental Assessments of Swallowing
The recognition of dysphagia as an essential area of otolaryngologic practice is reflected in the AAO-HNS Otolaryngology Core Curriculum, which includes both a dedicated Laryngology module on Dysphagia and a Pediatric Otolaryngology module on Pediatric Feeding and Swallowing Disorders. That said, individual residents' hands-on experience with instrumental swallowing evaluations, especially in the pediatric population, can still vary considerably depending on training environment and case exposure.
Accurate interpretation of pediatric FEES, in particular, requires familiarity with normal and abnormal anatomy across developmental ages, knowledge of pediatric conditions that contribute to dysphagia, and interdisciplinary training with collaborating SLPs. Advanced fellowship training in pediatric otolaryngology may therefore be valuable for developing deeper competency in this area.
Importantly, while both VSS and FEES may be used to characterize pediatric swallowing concerns, these studies are not interchangeable. A comparison of FEES and VFSS is included in Table 1.
Table 1. FEES vs. VFSS: Key comparisons across clinically relevant domains.
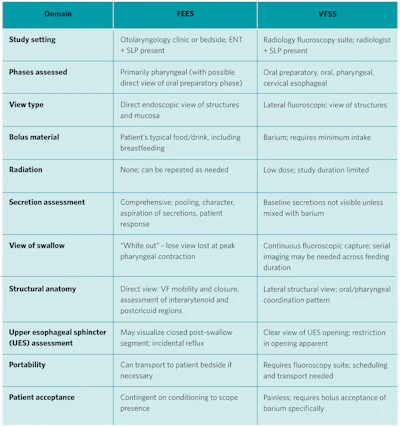
The decision to pursue FEES in place of or in addition to VFSS is typically driven by specific clinical indications.
Specific indications for FEES in pediatric patients include:
- Suspected pharyngeal dysphagia or aspiration in the breastfeeding infant (typical food/drink used during FEES, including breastfeeding directly)
- Abnormal vocal quality with concurrent swallowing concerns (may be indicative of laryngeal pathology)
- Post-surgical assessment when vagus nerve may be affected (cardiac surgery, posterior fossa/brainstem tumor resection, thyroid/neck surgery)
- Concern for secretion management as the primary clinical question (VFSS cannot assess baseline secretions)
- Diagnosed or suspected structural abnormality: laryngomalacia, vallecular cyst, laryngeal web, intubation trauma, interarytenoid height abnormality
- Odynophagia (pain with swallowing) that warrants direct mucosal inspection during food trial
- Globus sensation, particularly if symptom occurs with specific food consistencies
- History of repeated radiation exposure or contraindications to radiation (FEES carries no radiation burden)
- Positioning challenges that limit fluoroscopic view on VFSS and/or inability to transport patient to radiology suite
- Stridor or worsening stridor in association with feeding (real-time laryngeal visualization during eating)
- Persistent pharyngeal dysphagia symptoms despite prior VFSS; FEES may provide complementary and often additive information
- Need for repeated monitoring during feeding therapy; no radiation limits to the number of studies
Possible contraindications to FEES include:
- Severe nasal obstruction precluding scope passage (e.g., choanal atresia)
- Severe agitation and likely inability to cooperate with examination (relative contraindication; experienced teams can often proceed with appropriate preparation)
- Bleeding disorders or history of recent severe epistaxis
- Recent trauma to nasal cavity or surrounding tissues
- Severe micrognathia or glossoptosis limiting visualization (e.g., Pierre Robin Sequence—may require alternative positioning or VFSS)
- Pharyngeal stenosis limiting endoscopic access
Moving Toward Integrated Dysphagia Care
While both SLPs and otolaryngologists are able to perform FEES independently, a joint evaluation is considered the gold standard. Performing FEES studies via a collaborative, multidisciplinary approach with both SLP and otolaryngology leverages each provider’s unique expertise. In most pediatric centers, the otolaryngologist passes the laryngoscope and is able to evaluate the upper aerodigestive tract and laryngopharyngeal anatomy directly, while the SLP assesses the physiology and subsequent safety and efficiency of the patient’s swallow. The SLP can simultaneously test compensatory strategies in real time, including trialing varied flow rates, bolus viscosities, and patient positioning, which allows feeding recommendations and any indicated follow-up to be made collaboratively before the patient leaves the room.
In many tertiary pediatric centers, dedicated multidisciplinary dysphagia teams have formalized this model into structured clinics with consistent communication, shared documentation, and streamlined care pathways. When feasible, this integrated model allows for clear communication and shared decision-making that optimizes patient outcomes. However, meaningful collaboration does not require a fully built-out program to be effective. At its core, a strong SLP-otolaryngology partnership is built on cross-disciplinary familiarity and understanding the scope of practice of the collaborating service. Building strong SLP-otolaryngology partnerships is a clinically meaningful goal for any practice that cares for patients with dysphagia—and one that pays dividends in diagnostic precision, treatment efficiency, and patient outcomes.
Additional Information
You can share valuable resources on dysphagia and swallowing health with your patients and their caregivers this month and beyond.






