What’s on Your Radar Screen?
The fresh start of a new year always provides us opportunity for personal new beginnings. But sometimes, before we start to launch our automatic “New Year Resolutions” internal software, it might be worth it to take a step back and ask ourselves, “What is really important to me?” A useful technique often used by facilitators of strategic planning is to ask participants to plot significant concerns on a virtual “radar screen.” These visual representations of issues that confront us can be sobering, inspirational, informative, and suggestive of how to prioritize our businesses and our personal lives. Each of us can (and usually does) have multiple radar screens of important issues. We might have one screen related to business affairs, one for family issues, one for personal concerns, and so on. A professional radar screen of a busy medical practitioner might include concerns about healthcare reform, hospital privileges, new business models for medical practice, payment reform and its effects on profitability, CME, how to improve quality care and reduce risk for medical error, volunteer Academy service, staffing of the office, sub-specialization, access to care, and many more issues. (See Figure 1.) Looking at our personal lives, we might have a radar screen that includes personal health problems, care of a chronically ill parent or other family member, attending our teens’ school or sports functions, managing day care, putting time into our marriages and valued relationships, or community roles (PTA, homeowners association, public service), or saving for retirement. (See Figure 2.) Radar screens can represent any issue or set of issues that has a significant impact on our lives or a demand on our time and attention. We could create a time-based screen, showing a longitudinal view of the development of specific areas of interest. For example, most of us spend significant amounts of time and energy dealing with the Internet and social media. Plotting the amount of time spent on this demand for our attention over the years, we can begin to evaluate whether it is an irritation and intrusion on our lives or a valuable tool for desired communication. We also can make informed judgments about how it may change or affect us in the future. Significant public use of the Internet began in 1994. Today, its virtual offspring include not only email communications, but real-time audio and video communications, gaming, virtual reality, learning systems, shared business applications, cloud computing, and more. You can envision as many radar screens as needed to evaluate the various segments of your life. However, at some point, realistically, we have to superimpose all of these radar screens upon one another to get a true picture of the complexity of our lives. (See Figure 3.) This is where we see graphically all of the hats we wear and all of the commitments. We also may see why at times we have a sense of being out of control. Our radar screens can get pretty crowded. But this is also where we can start to get some clarity; we begin to see the need for simplification and prioritization. Just as with an air traffic controller, when the radar gets too crowded with too many aircraft in too close proximity, near misses can quickly turn into disasters. Are we living our lives with a high number of near misses? Is some of the air traffic on our radar screen distracting us from managing more carefully what we value most? Can we clear the radar screen of some excessive and distracting blips and focus more closely on the highest value priorities? As we embark on another challenging year, your Academy staff commits to continued focus on providing you with high value membership, meaningful and high quality medical education, excellence in research support and quality tools, and optimal communication. We look forward to working with you to make 2011 the best year yet.
 David R. Nielsen, MD, AAO-HNS/F EVP/CEO
David R. Nielsen, MD, AAO-HNS/F EVP/CEOThe fresh start of a new year always provides us opportunity for personal new beginnings. But sometimes, before we start to launch our automatic “New Year Resolutions” internal software, it might be worth it to take a step back and ask ourselves, “What is really important to me?”
A useful technique often used by facilitators of strategic planning is to ask participants to plot significant concerns on a virtual “radar screen.” These visual representations of issues that confront us can be sobering, inspirational, informative, and suggestive of how to prioritize our businesses and our personal lives.
Each of us can (and usually does) have multiple radar screens of important issues. We might have one screen related to business affairs, one for family issues, one for personal concerns, and so on. A professional radar screen of a busy medical practitioner might include concerns about healthcare reform, hospital privileges, new business models for medical practice, payment reform and its effects on profitability, CME, how to improve quality care and reduce risk for medical error, volunteer Academy service, staffing of the office, sub-specialization, access to care, and many more issues. (See Figure 1.)
Looking at our personal lives, we might have a radar screen that includes personal health problems, care of a chronically ill parent or other family member, attending our teens’ school or sports functions, managing day care, putting time into our marriages and valued relationships, or community roles (PTA, homeowners association, public service), or saving for retirement. (See Figure 2.)
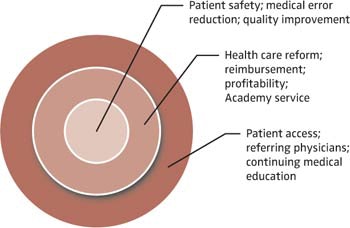 Figure 1. Business radar screen.
Figure 1. Business radar screen.Radar screens can represent any issue or set of issues that has a significant impact on our lives or a demand on our time and attention. We could create a time-based screen, showing a longitudinal view of the development of specific areas of interest. For example, most of us spend significant amounts of time and energy dealing with the Internet and social media. Plotting the amount of time spent on this demand for our attention over the years, we can begin to evaluate whether it is an irritation and intrusion on our lives or a valuable tool for desired communication. We also can make informed judgments about how it may change or affect us in the future. Significant public use of the Internet began in 1994. Today, its virtual offspring include not only email communications, but real-time audio and video communications, gaming, virtual reality, learning systems, shared business applications, cloud computing, and more.
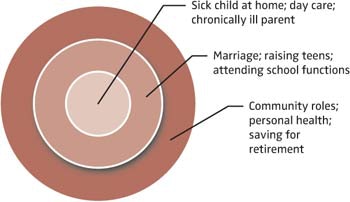 Figure 2. Personal radar screen.
Figure 2. Personal radar screen.You can envision as many radar screens as needed to evaluate the various segments of your life. However, at some point, realistically, we have to superimpose all of these radar screens upon one another to get a true picture of the complexity of our lives. (See Figure 3.) This is where we see graphically all of the hats we wear and all of the commitments. We also may see why at times we have a sense of being out of control. Our radar screens can get pretty crowded.
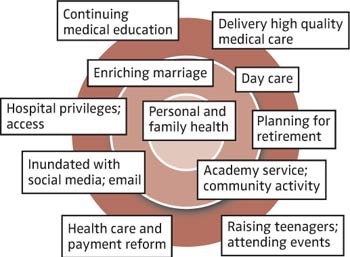 Figure 3. Combined radar screens.
Figure 3. Combined radar screens.But this is also where we can start to get some clarity; we begin to see the need for simplification and prioritization. Just as with an air traffic controller, when the radar gets too crowded with too many aircraft in too close proximity, near misses can quickly turn into disasters. Are we living our lives with a high number of near misses? Is some of the air traffic on our radar screen distracting us from managing more carefully what we value most? Can we clear the radar screen of some excessive and distracting blips and focus more closely on the highest value priorities?
As we embark on another challenging year, your Academy staff commits to continued focus on providing you with high value membership, meaningful and high quality medical education, excellence in research support and quality tools, and optimal communication. We look forward to working with you to make 2011 the best year yet.