- February 2013
- House Energy & Commerce (E&C) Committee conducts hearing on SGR issue.
- House Ways & Means (W&M) Committee staff briefs physician community on development of SGR legislation.
- Congressional Budget Office (CBO) reduces cost estimate for SGR repeal.
- May 2013
- House W&M conducts hearing to collect information on potential reform proposals.
- Senate Finance Committee solicits feedback from physician community regarding future of fee-for-service system.
- House E&C briefs physician community on “framework” for SGR repeal legislation.
- June 2013
- House E&C releases revised SGR framework.
- July 2013
- House E&C conducts markup of SGR bill and unanimously votes to advance the proposal.
- October 2013
- Senate Finance and House W&M release legislative framework to repeal the SGR formula.
- November 2013
- Staff for Senate Finance and House W&M brief physician community on legislative framework.
- December 2013
- Senate Finance conducts markup of SGR framework; approved by Committee.
- House W&M conducts markup of SGR legislation; approved by Committee.
- Two-year budget deal signed into law; includes three-month SGR “patch.”
- February 2014
- Bipartisan, bicameral legislation (H.R. 4015/S. 2000) to repeal the SGR formula and reform the Medicare physician payment system introduced in Congress.
- Senate Finance Chairman Max Baucus (D-MT) departs U.S. Senate and is replaced by Sen. Ron Wyden (D-OR).
- March 2014
- H.R. 4015 passed by U.S. House of Representatives (March 14) with partisan offset.
- U.S. House passes 12-month SGR patch (March 27) via vote voice.
- U.S. Senate passes (64-35)12-month SGR patch (March 31).
- April 2014
- President signs 12-month SGR patch (April 1).
More from June 2014 - Vol. 33 No. 06

What do you see as the priorities of the Nominating Committee in selecting the future leaders of our Academy?
Phyllis Bergeron Bouvier, MD
The Nominating Committee is such an important entity in determining the ongoing success of our Academy. With the challenges we have and will be experiencing with healthcare reform come great opportunities to achieve our strategic goals through visionary leaders who will be able to influence policy, build and strengthen our grassroots infrastructure, and develop our global pillar. We see our membership becoming increasingly diverse, in terms of gender, age, race/ethnicity, types of practice, veteran and disability status, and sexual orientation. Our leaders must be responsive to the needs of each group, constantly connecting to and engaging both members and nonmembers of our otolaryngology community so that no voice goes unnoticed.
It is also important to have a blend of established physicians and young physicians, who will help envision our future through a different lens. I have had the opportunity to collaborate with varied members of our organization through my participation on many Academy committees, such as the Diversity Committee, the BOG, and the Endowment, Nominating, and Programs Committees of the WIO. As a member of the Nominating Committee, I would seek out those who would help fill in the gaps that may exist in our Academy’s Leadership. Thank you for this honor.
Brian A. Moore, MD
We are all leaders—in our families, communities, and hospitals—so it is truly a humbling experience to be considered for the Nominating Committee. Tasked with promoting the “Best of the Best,” the Nominating Committee seeks to uphold its responsibility to our membership by identifying those among us who have the dedication and drive to lead our profession through a dynamic period in healthcare. As a section-head at Ochsner Medical Center, a resident educator, an active member of various committees of the AAO-HNS, and a former military officer, I have been privileged to not only study the principles of leadership but also to struggle through its practice.
The Academy deserves leaders with the vision to recognize the challenges that lie ahead; wisdom to listen to its diverse membership; humility to promote a collaborative approach to overcoming these obstacles in concert with other stakeholders; devotion to service; grace to articulate the message and inspire us; and courage to uphold our core values, even when unpopular, in order to achieve the Academy’s stated mission of excellence. These leaders must reflect the practice, subspecialty, geographic, and demographic diversity of our great specialty.
Lisa Perry-Gilkes, MD
“Without vision the people perish.” The honor of being considered for the Nominating Committee is not taken lightly. This committee has the responsibility of selecting the physicians who will form the future and the vision of our academy.
Priority 1: Select leaders with insight to prepare us for the evolution of medicine. These changes are on all fronts and all modes of practice. Our specialty is rapidly advancing in patient care innovations. We will also conform to the changes required by the Affordable Care Act, ICD-10, and SGR.
Priority 2: Select leaders who are comfortable with and understand how legislation, medical advances, and health disparities affect our patients and our members.
Priority 3: Select candidates who reflect our members. We are a group of heterogeneous members from general otolaryngologist to subspecialist, members still in training to seasoned professionals, an ever-increasing diverse group, but we join together in one voice.
I serve on the Board of Governors, am Chair of the Diversity Committee, and am a standing guest of the AAO-HNS/F Boards of Directors. These opportunities allow me access to many dedicated members. I would be honored to serve in this new capacity. Thank you for your support.
Lawrence M. Simon, MD
The Nominating Committee of the AmericanAcademy of Otolaryngology—Head and Neck Surgery is a cornerstone of our organization. The candidates who the Nominating Committee offers to our membership will be responsible for guiding our Academy through one of the most tumultuous times for physicians in recent history. The policies they enact and the decisions they make will impact our specialty and our lives for many years to come. In this spirit, the top priority of the Nominating Committee is to identify the most qualified candidates for each opening. First, the search process must be fair and non-partisan with all potential candidates given their due consideration. Second, achieving diversity must also be a priority. Our Academy becomes more varied every day, and having leaders as diverse as our membership will help our organization develop a strategic plan that speaks to members of every practice model, ethnicity, gender, and age. Lastly, the Nominating Committee must also make certain that potential candidates possess the requisite knowledge and experience to fulfill their obligations and to facilitate the execution of the Academy’s Strategic Plan. Fulfilling this charge will require discretion and judgment in order to objectively evaluate potential nominees and select the best people possible. 
Given the uncertainty of today’s healthcare environment, what do you perceive as challenges and possible solutions to implementing the Academy’s strategic plan?
Paul M. Imber, DO
Is it kismet that I write my response to this provocative question on the evening that the Senate passes the 17th band-aid to the SGR debacle in 11 years, in spite of the potential to pass a bicameral, bipartisan permanent fix to the problem? The legislation also will delay ICD-10 implementation
by 12 months, and redirect savings from “misvalued codes” to “undervalued codes” and capture any excess as budget savings.
Advocacy is the ultimate tool of the Academy, as our members strengthen our presence with state and federal legislators. We can connect with our policy makers through the I-GO Program and obtain information from the biweekly Legislative Advocacy Network. Our Government Affairs staff members are superb stewards of our legislative interests, and are available resources to the membership to enhance engagement and unity.
The ever-changing reimbursement environment is replete with new, innovative experiments. The Academy can function as a research clearinghouse, collaborating the different structures and data from these projects, and sharing this information with the members to preclude repetition of failures and promote the proliferation of successes. The 3P is already in place to facilitate this process.
The need for practice and quality performance will be a component of any forthcoming payment reform program. The Academy needs to further sponsor the development of clinical guidelines, based on evidence-based research. The membership needs to avail itself of this knowledge.
The strategic plan can adapt in its direction, while maintaining its precepts, with appropriate leadership and counsel.
Jay S. Youngerman, MD
Challenges:
Ever increasing demands on physicians from patients, government, insurers, and businesses are driving the uncertainty in today’s healthcare environment.
First, the goal of higher quality and more efficient care is shared by all, but resulting regulations and metrics have encouraged standardization and bureaucracy at the expense of the best personalized care.
Second, as our colleagues become employees of large hospitals or groups, the shift of both daily and long-term decision-making from physician to administrator has diminished our collective influence on the way we practice.
Finally, information technology, in the form of cumbersome electronic records and online clinician ratings and patient information, has put us on the defensive rather than on the forefront.
Solutions:
Education: The Academy must be the recognized source on the web for the education of both clinicians and patients. Meetings must remain an indispensable forum for discourse, networking, and camaraderie.
Research and quality: Through evidence we can steer the tide of performance and efficiency toward truly better care for our patients. We must support models that simultaneously promote quality, reduce waste, and protect reimbursement.
Advocacy: Only the Academy can represent the specific interests of otolaryngology. We must continue to represent our specialty relentlessly at the national, state, and local levels.
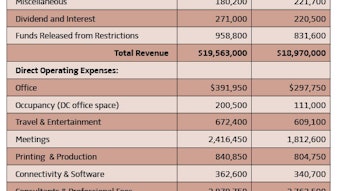
Sustainability: We must make particular efforts to attract our residents and young physicians, as well as the administrators, subspecialists, and physician extenders who are critical to our field. As the former Chair of the Board of Governors Development Committee, I will continue to encourage philanthropy through the Millennium Society, Women in Otolaryngology, and endowments. We must also encourage new revenue streams, corporate support, NIH grants, and CORE grant sponsors. The budget has been prepared on a cash basis. This basis is important to reflect the ability for an organization to meet its true financial obligations, regardless of whether the cash outlay is a true “expense” or merely balance sheet accounting. The FY15 budget prioritizes the direction of the BODs and is based on conservative estimates of both revenues and expenses. The FY15 balanced budget is presented at $18.97M, about three percent lower than the FY14 budget of $19.56M.
Nearly 75 percent of FY15 revenue, $14.06M, is budgeted to come from two major areas: membership dues and Annual Meeting revenue. Membership dues include a calendar year 2015 dues increase. Annual Meeting registration revenue is budgeted slightly higher than Vancouver but this is offset by a reduction in Instruction Course fees, mainly due to the change in the Annual Meeting length. Budgeted revenue reductions are in royalties income, which is primarily due to a change in presentation of Bulletin royalties, which are now reflected net of expenses, and corporate and individual support, which reflects the expected continued decline of unrestricted giving. As presented, overall revenues are down as compared to FY14; however, an ongoing commitment has been made to focus on increasing revenues as a result of new products and services.
To balance the budget with the expected reduction in revenue sources, operating expenses had to be thoroughly reviewed, streamlined, and affirmed as related to the strategic plan. The expenses for the AAO-HNS/F are separated into two areas.
The first area includes direct operating costs relating to each business unit; these are costs directly related to carrying out the priorities of the strategic plan and other ongoing mission-related programs. Two programs to be eliminated in FY15 are Partners for Progress (PfP) and Patient Management Perspectives in Otolaryngology (PMP). Also in FY15, the Washington, DC, office will be closed, although a small work space will be retained. In addition, the FY15 budget includes expenses related to expanding Quality Measures Development and added support to create a plan for the development of a comprehensive curriculum for otolaryngology.
The second area, allocated costs, relates to staffing and benefits as well as the operating costs that are incurred for the good of the whole organization, such as occupancy and building-related expenses, and organizational-wide HR, financial, and IT costs. Overall, allocated costs have increased due to inflation, contractual commitments, and salary adjustments; direct operating expenses have decreased due to the location of the 2014 Annual Meeting & OTO EXPOSM and streamlining other expenses.
The complete budget is available to any Academy member who requests it in writing. Email requests to Brenda S. Hargett, CPA, CAE, COO, to bulletin@entnet.org. 
James E. Saunders, MD
AAO-HNSF Coordinator
for International Affairs
International relations have long been an integral part of our Academy. The first international satellite and joint meeting with the Pan-American Otorhinolaryngology and Broncho-esophagology Congress was hosted in 1946 by the AmericanAcademy of Otolaryngology and Ophthalmology under the leadership of AAOO President Gordon New, MD, Chevalier Jackson, MD, and Paul Hollinger, MD.
Since then we have seen tremendous growth in the international scope of the AAO-HNS/F. Today nearly 40 percent of physician attendees at the Annual Meeting & OTO EXPOSM come from outside the United States. These attendees and our international members represent the best and the brightest of the global community of otolaryngology.
Our Academy is actively working to engage with these international colleagues. One cornerstone of this effort is Global Health 2014: Your Academy around the World. Originated by Gregory W. Randolph, MD, and now in its fourth year, this Miniseminar is a wonderful opportunity to hear international experts talk about their work and otolaryngology at home. At this exchange, we often find there are both striking similarities and differences in the problems we face.
Relatively new at the 2014 Annual Meeting is the International Assembly, in which Academy members and guests from our 55 International Corresponding Societies will honor the recipients of the International Visiting Scholarships and hear from our Academy leadership on topics of international interest.
The Academy is also proud to collaborate on five joint meetings with international societies throughout the year and four international satellite events at the Annual Meeting, including the new offerings of a Francophone Otolaryngology Update and a Combined AAO-HNSF and Middle Eastern Otolaryngology Societies Meeting Saturday, September 20 in Orlando.
As you can see, an important element of international relations is still getting otolaryngologists together in the same room. But, unlike that early meeting in 1946, we have new tools to help us reach out to otolaryngologists from around the world.
Last year, the Academy took the idea of a joint meeting one step further by reaching out to our Latin American Colleagues with a Latin American Webcast. More than 300 Latin American otolaryngologists participated in a Spanish-translated simulcast from Vancouver. This year we hope to expand this theme with an even wider distribution in Latin America and a broader international audience.
With the expansion of virtual meetings such as this, online journal access to Otolaryngology–Head and Neck Surgery, continued expansions in our online educational materials for international members, and online communities such as ENTConnect, your Academy keeps changing and evolving to maintain its position as a leader in the global community of otolaryngology.
Our Annual Meeting in 2014 promises to be the most advanced and internationally connected gatherings of otolaryngologists yet. Perhaps it is fitting that such a meeting should take place in Orlando, home of EPCOT®.
Just before his death, Walt Disney described his vision for the project as a “community of tomorrow” that will constantly change and never be completed. Today, the theme park is a “celebration of human achievement, technology innovation, and international culture.” Sounds a bit like our Academy, doesn’t it? 
Kavita Dedhia, MD
Humanitarian Travel Grantee
Raj C. Dedhia, MD
As husband and wife, we had the unique experience of traveling together from Pittsburgh, PA, to Butajira, Ethiopia, in early June to take part in a surgical mission for patients with chronic ear disease.
The trip was made possible by the collaboration of Ethiopian physician Nega Kiros, MD, and leader of Global ENT Outreach (GEO) Richard Wagner, MD. Dr. Wagner assembled an international team including himself, Marta Sandoval, MD (ENT-Spain), Pedro Benitez, MD (ENT-Spain), and Victor Estevez, MD, (Anesthesia-Spain) on the “Butajira Middle Ear Program.”
Dr. Wagner founded GEO in 2000. The organization has flourished during the last 13 years and now serves more than 10 countries. Dr. Wagner successfully established two temporal bone laboratories, one in Peru and the other in Cambodia.
Apart from the chief goal of providing patient care, there was a strong emphasis from the attending physicians on educating both Ethiopian otolaryngologists and us, residents from the United States. Two of the three microscopes had teaching arms allowing for attending oversight during cases. Additionally, one of the microscopes was hooked up to a projector system. This allowed the surgery to be viewed by a larger audience to allow better visualization of the procedures.
We met in Addis Ababa on Sunday, June 10, and traveled by car to the small town of Butajira. That afternoon, we evaluated nearly 100 pre-screened patients in clinic for surgical candidacy. While they patiently waited outside to see if they were to have surgery, we spent the next few hours triaging the group. We scheduled a total of 51 surgeries during the following five days.
We set out to complete roughly 10 complex cases per day including tympanoplasties, mastoidectomies, and tympanomastoidectomies with and without ossicular chain reconstruction. We used one large operating room, which was divided into three sections to maximize our efficiency by operating on up to three patients simultaneously. The majority of cases were performed under monitored anesthesia care (MAC) while younger children received general anesthesia.
Our day started with team breakfast at 7:30 am with an 8:00 am operating room start. We typically finished cases by 6:00 pm. Following dinner, we reviewed each of the cases from the day and reviewed surgery that had been recorded on one of the microscopes. It provided an excellent opportunity to reflect on our operative mistakes and learn from the experiences of others. Teaching the Ethiopian residents and physicians was the central goal of this surgical mission.
From June 11 through 15, we completed 51 otologic surgeries without notable complications. We provided care to an area that is profoundly underserved. To give perspective, the ENT nurse in Ethiopia stated that there were roughly 10,000 patients in Butajira on the waiting list to be seen in our clinic and possibly require surgery as sequelae from chronic otitis media. Ethiopia has a limited number of otolaryngologists, and of the otolaryngologists few are adept at providing complex otologic care. There are also virtually no supporting services such as trained audiologists and speech therapists. All of these factors increase the burden of ear disease in Ethiopia.
It is the hope of Dr. Wagner and the GEO to continue to train Ethiopian otolaryngologists (roughly 20 ENTs in a country of 84 million) in complex otologic surgery. In particular, the GEO is attempting to build an Ethiopian partnership to house a temporal bone laboratory in Addis Ababa and raise awareness for the devastating impact of middle ear disease.
We would like to thank the Academy for its generous support in providing Kavita the Humanitarian Travel Grant and allowing us the incredible opportunity to give back to the global community. 
Kanwar S. Kelley, MD, JD
Bryan Brandon, BS
Hamid Z. Djalilian, MD
For 200 years, the cause of Ludwig van Beethoven’s deafness has been the subject of much conjecture and intrigue. A great deal of controversy exists about Beethoven’s illnesses, of which there were many, and about the cause of his death. Many have tried to establish a unifying theory for his various illnesses, citing syphilis, Crohn’s, and lupus as potential diagnoses.1
What we do know is Beethoven exhibited diminished speech discrimination, hyperacusis, and progressive bilateral hearing loss (left greater than right), progressing to profound deafness during the course of his life, which was associated with constant bilateral tinnitus, but no vertigo.2
For the first time, we propose migraine-related hearing loss as a possible etiology of his deafness. There is evidence from various accounts that Beethoven suffered from chronic headaches, and it has been theorized that these headaches were migraine-related.3
Unfortunately, there is little literature documenting the exact nature of the headaches, but we do know Beethoven suffered from nearly all of the most common migraine triggers—poor sleep, irregular diet, and symptoms consistent with irritable bowel syndrome, which is frequently related to migraines.4,5
He was afflicted by recurrent colicky abdominal pain and alternating bouts of diarrhea and constipation, which have led many to believe he suffered from inflammatory bowel disease.6
In 1810, the same year as his last documented bout of headaches, he was described as having poor, “fitful” sleep, preferring wakefulness to any kind of sleep.4,5 In addition, Beethoven was noted to have a long history of depressive symptoms and myriad of life stressors.4
While the cause of Ludwig van Beethoven’s hearing loss will likely forever remain unknown, we propose adding migraine-related hearing loss to the long differential diagnosis.
References
Kubba A, Young M. Ludwig van Beethoven: a medical biography. Lancet. 1996;347:67-70.
Shearer PD. The deafness of Beethoven: an audiologic and medical overview. Am J Otol. 1990;11: 370-374.
Davies PJ. Beethoven in person: his deafness, illnesses, and death. Westport, CT: Greenwood Press; 2001.
François MM. Diagnosing genius: the life and death of Beethoven. Ithaca, NY: McGill-Queen’s University Press; 2007.
Albrecht T. Letters to Beethoven and other correspondence. Lincoln, NE: University ofNebraska Press; 1996.
Cooper M. Beethoven: the last decade. New York, NY: OxfordUniversity Press; 1985. 
In our ongoing efforts to address the results of the 2013 Education Needs Assessment Initiative, the Foundation will introduce enhancements to current education activities that are key drivers of engagement with the AAO-HNS/F. The Needs Survey measured the value of the Foundation Education Program on three levels: how a member rates the program on its own merits; in comparison to other organizations’ education activities; and on the likelihood to recommend to others.
The Education Steering Committee (ESC), comprised of the eight Education Committee chairs and under the leadership of Sonya Malekzadeh, MD, has reviewed all of the current education products offered by the Foundation based on the data gathered throughout the needs assessment. They developed a comprehensive list of enhancements to current activities and other changes that will increase the effectiveness of the Foundation’s education offerings.
Plans have been set to enhance existing education activities that have a strong influence on member engagement. A brief description of these enhancements follows.
AcademyQ®
Since its introduction in 2012, AcademyQ has seen immense growth and popularity. Those who have used the mobile app appreciate it for “offering a representative set of questions across all subspecialties” and “providing consistently high-quality content.” Knowing there is a need for constant updates in order to keep the app a useful product, the Foundation will add hundreds of new questions this year. Also exciting is the ability now to offer the app for operating systems other than Apple. This will allow the Foundation to build the new version of AcademyQ during the next several months.
Home Study Course
It’s probably no surprise to anyone that the Home Study Course (HSC) is most otolaryngologists’ first experience with the Foundation and a huge driver of member engagement with the Academy. Members report that it “provides consistently high-quality content” and “offers a reasonable price for the course.” HSC also succeeds in “covering the appropriate depth of content within each of the specialties.”
A Home Study Task force has been convened under the leadership of Brad W. Kesser, MD, and Richard V. Smith, MD, both members of the Education Steering Committee (ESC). This Task Force is charged with developing a plan to update and enhance the Home Study Course experience for a broader base of members. The Task Force conducted a survey with all current HSC subscribers. The survey yielded excellent information that will be used when developing a road map for the future of the activity. The Task Force plans to present its report to the ESC in September.
Annual Meeting & OTO EXPOSM Program Content
The Annual Meeting & OTO EXPOSM is also a strong driver of member engagement. About one-third of members attend the Annual Meeting every year while an additional 40 percent attend every few years. For those who attend the meeting, the part of the experience that has significant influence is “providing consistently high-quality content” and “offering an appropriate balance of clinical and practice management education.” Information from the education needs assessment has flowed into a comprehensive assessment of the annual meeting. One component of this assessment is to take a look at how Annual Meeting education content can be repurposed and offered to a wider member audience. Look for greater opportunities to access this content soon.
Clinical Otolaryngology Online (COOL)
COOL is designed for the non-otolaryngologist. For those who have used COOL, the resource influences their engagement in the education program. These individuals seek a resource that “provides an easy-to-understand assessment of otolaryngology-related topics” and “provides adequate information to make an appropriate otolaryngology referral.”
There is an increased emphasis at the Academy on reaching out to non-physician healthcare providers who work in otolaryngology-head and neck surgery. A re-evaluation and the development of new COOL courses is a part of this effort.
Coding and Reimbursement Workshops
Those respondents who have attended the Coding and Reimbursement Workshops indicate that their experience had a significant influence on their overall engagement with the Foundation.
Due to the timeliness and imperative regarding the adoption of ICD-10 in physician practices, the Coding and Reimbursement Workshops now has a third session on ICD-10 implementation. This full-day workshop assists both physicians and their staffs in preparing for the transition.
eBooks
It is very exciting to report that three AAO-HNSF publications are being updated and re-released in the next 12 months. Because of a formal publishing agreement the Foundation has entered into with Thieme Publishing, two books will be published online and in print this year. Geriatric Care Otolaryngology is being updated under the leadership of Robert T. Sataloff, MD. Otolaryngology Lifelong Learning Manual, a revised version of the Maintenance Manual for Lifelong Learning, will also be published under the leadership of Sonya Malekzadeh, MD, and the Education Steering Committee. Members of the eight Education Committees served as chapter reviewers and authors.
The Quick Reference Guide to Neck Dissection Classification and TNM Staging of Head and Neck Cancer is also being revised under the leadership of Daniel B. Deschler, MD. This will be the fourth edition of this helpful resource that will include the most recent AJCC Cancer Staging Tables.
Online Education
Online Education including the Online Lecture Series (OLS), which are recordings of Annual Meeting Instruction Courses and Online Courses that are developed by Education Committee members contribute influence by “presenting content logically so that it is easy to follow,” “providing consistently high-quality content,” and “covering the appropriate breadth of content across specialties.”
A clear message from the Needs Assessment Survey was the strong recommendation that the Foundation education activities be more web-based and more engaging. Look for new online courses that are cased-based, interactive, and self-paced.
A new Learning Management System will be built that will offer many more opportunities to develop high quality and engaging activities. In addition, the Professional Development pages of the new entnet.org have been redesigned to provide access to the resources members need to engage in education with the Foundation. Continue to look for improvements to current popular education products and the introduction of new eLearning technology to enhance relevance to members. What to Do Now to Mitigate Financial Risk
Cheryl L. Toth, MBA
Practices have many competing, high priorities these days: dealing with Electronic Health Records (EHR) implementation, qualifying for Meaningful Use, conducting diligence on the hospital’s employment offer, and, of course, transitioning to ICD-10.
Right now, everyone in the office is (rightfully so) running around, cross walking codes, modifying dictation habits, and chasing down payer end-to-end testing dates.
Meanwhile, back in the billing office, attention is slowly slipping away from the accounts receivable. Following up on overdue insurance balances, setting up patient payment plans, monitoring the A/R as they typically would are taking a back seat to ICD-10 and other “distractions.” This should concern you. A lot.
Despite competing priorities, practices must take the time to plan ahead for a potential post-October 1, 2015 revenue hit. Ripped from the headlines, here’s why:
“Implementation of ICD-10 May Cause Serious Cash Flow Problems for Providers.”1
This is according to many sources—most notably the Department of Health & Human Services (HHS). Enough said.
If you don’t already have one, apply for a line of credit soon. Banks prefer to dole these out before they are actually needed. And come October 2015, you don’t want to be the 45th physician in line at the bank, pleading for help.
You’ll rely on a line of credit less if you’ve got some cash squirreled away, so build a nest egg this spring and summer. Focus on cleaning up 90-day and 120-day insurance receivables—which typically have the highest payoff for the least effort. Hiring an experienced biller or collections specialist to conduct this cleanup on a project basis is money well spent. Having an extra set of hands frees up the billing team for transition planning and testing, as well as the potential deluge of claim denials and technology glitches after. Ask for a summary of follow-up results monthly. Set a goal to have the insurance A/R cleaned to the point that no more than 10 percent of all payer receivables are less than 90 days old on September 30 of next year.
For past due patient accounts, launch a “spring collection campaign.” Seventy-four percent of patients said they were willing and able to pay out-of-pocket expenses less than or equal to $1,000, and 62 percent were willing to pay medical bills greater than or equal to $1,000. Thirty-seven percent of patients said that a lack of payment options was the reason they didn’t pay healthcare bills.2 Interpretation: Do a better job asking patients to pay, and give them more payment options.
Instruct staff to focus on the highest balances first, and work accounts in descending balance order—not alphabetical order. Offer online bill pay through your vendor’s patient portal or a company such as TransFirst (www.transfirst.com) or PayPal (www.paypal.com). And make budget plan setting simple by offering patients automatic recurring payments. Like a Netflix subscription or gym membership, such payments are automatically charged to the patient’s credit card each month. TransFirst or PayPal also offer this feature.
“A Fifty Percent Decline in Productivity” and “Expect that Staff Will Have to Spend More Time in Follow-up with Plans.”
In its ICD-10 Implementation Guide for Small Practices, the Centers for Medicare & Medicaid Services (CMS) warns practices to expect more claim denials and an increased follow up time.3 Multiple reputable sources and studies predict significant slowdowns in staff’s ability to code a claim or case and get a claim out the door. ICD-10 pilot results presented at the Medical Group Management Association (MGMA) 2013 annual conference mirrored the experience of Canada’s ICD-10 transition: staff productivity drops 50 percent when staff attempted to identify the proper ICD-10 codes from physician documentation.4,5
Don’t deny these productivity predictions, and don’t wait until next summer to hire people. Staff up now, before the hospital snaps up the best candidates.
And if you think outsourcing the billing is a solution—it’s not. Even under the best circumstances, the outsourcing process is painful. And what if the billing company isn’t fully prepared for ICD-10? Better to hire an additional part-time or full-time coder and/or billing office staffer capable of consistent denial management who will keep cash flowing come fall.
“Docs Charting Falls Short of ICD-10 Demands.”6
While this information is not a complete surprise, it should be an eye opener for those who were hoping “someone in billing” would handle ICD-10, instead of the physicians. Actually, nothing could be further from the truth. Without the additional detail required by ICD-10, coders won’t be able to select the right code, resulting in backlogs of claims (read: unrealized revenue) and the need for staff to constantly follow up with physicians to obtain more detail.
And don’t forget about prior authorization letters for surgeries after October 1, 2015, which must be written to justify medical necessity using ICD-10 terms and codes. Because prior authorizations are typically done three to four weeks before surgery, physicians will be pre-authorizing in ICD-10 at least three or four weeks ahead of the deadline. If surgeries are booked months in advance, your practice may be required to pre-authorize (and pre-certify) using ICD-10 as early as next summer.
Revise dictation prompters and letter templates and check payer sites to determine how date of service and date of discharge affect which system to use for procedures scheduled close to October 1.
For other ICD-10 resources, visit the Academy’s ICD-10 page at http://www.entnet.org/Practice/International-Classification-of-Diseases-ICD.cfm.
Cheryl Toth, MBA, is a senior consultant and writer with Karen Zupko & Associates, Inc.
Please note: After passage of Protecting Access to Medicare Act of 2014 (PAMA) the deadline for compliance is now October 1, 2015.
References
1. Seidman M. ICD-10 and Version 5010. Bulletin. April 2012;31(4):11. http://bulletin.entnet.org/Assets/AAOBulletin/pdf/Bulletin_Apr_2012.pdf
2. McKinsey & Company. McKinsey on Payments. April 2009. http://www.mckinsey.com/App_Media/Reports/Financial_Services/US_healthcare_payments_Remedies_for_an_ailing_system.pdf
3. ICD-10 Implementation Guide for Small and Medium Practices. Issue brief. Centers for Medicaid Services 2013. Web. 1 Aug. 2013. http://www.cms.gov/Medicare/Coding/ICD10/Downloads/ICD10SmallMediumPracticeHandbook.pdf
4. McCann E. The ICD-10 Pilot That Was Just Plain ‘Scary.’ Government HealthIT. October 14, 2013 http://www.govhealthit.com/news/icd-10-pilot-was-just-plain-scary-coding-coders
5. Implementing ICD-10: A Canadian Perspective from the Front Line. Revenue Cycle Strategist. 2009:3. http://www.hfma.org/Publications/Newsletters/Revenue-Cycle-Strategist/Archives/2009/February/Revenue-Cycle-Strategist—February-2009-Issue/.
6. Pittman D. Docs Charting Falls Short of ICD-10 Demands. MedPage Today. April 12, 2013.
Learn More
Learn more revenue-cycle tactics and technologies at the Academy-sponsored workshop Kicking Revenue into High Gear.
Attend an AAO-HNS Coding & Reimbursement workshop as soon as possible. Physicians should be practicing in ICD-10 regularly.
Visit http://www.entnet.org/coding. The Medicare Payment Advisory Commission, otherwise known as MedPAC, is the independent commission charged by law to annually review the Centers for Medicare & Medicaid’s (CMS) Medicare payment policies and then make recommendations to control costs under the system. In March, MedPAC sent its annual report to Congress with recommendations that would considerably affect physician and other health professional services, Ambulatory Surgical Center Services (ASCs), hospital inpatient and outpatient services, and more. To keep members apprised of any important communication exchanged between MedPAC and Congress, the Health Policy team not only regularly attends MedPAC meetings, but also reviews the Commission’s two annual reports. Below is a brief summary of the key provisions from this year’s report that are relevant to otolaryngology-head and neck surgery.
Background
One of the main responsibilities of MedPAC is to make payment update recommendations for providers paid under FFS Medicare. An update refers to the percentage change by which the base payment rate is changed from one year to the next. Base payment rates are the payments for all providers in a payment system. The update is determined by looking at a variety of factors, including adequacy of payments to providers in the current year, beneficiaries’ access to care, quality of care provided, providers’ access to capital, and associated costs for both Medicare and providers. In addition, MedPAC looks at what features are likely to change in the coming year (i.e., the year the update will take place). Further, consideration of other influences is also factored into the equation, with MedPAC then determining whether or not a recommended increase, decrease or no change in payment is warranted. The relevance to you is that “these update recommendations, if enacted, could significantly change the revenues providers receive from Medicare.” (Report to the Congress: Medicare Payment Policy. March 2014:xiii.)
This year, MedPAC made recommendations affecting several FFS settings, some of which included hospital inpatient and outpatient services, physicians and other health professionals, and ASCs.
Hospital Inpatient and Outpatient Services
A host of changes were recommended for hospital payment systems for 2015 in an effort to reduce perceived excessive payment rates and create equity among various settings. According to MedPAC, Medicare typically pays more for services performed in hospital outpatient departments (HOPDs), even though such services are often performed in the physician office setting. This discrepancy is viewed as creating an incentive for hospitals to purchase physician offices and convert them to HOPDs, thus receiving nearly double the payment despite no real difference in location and patient mix. To limit this distortion, and address other concerns, MedPAC made the following recommendations:
Differences in payment rates between outpatient departments and physician offices for selected ambulatory payment classifications should be reduced or eliminated.
Long-term care hospital (LTCH) base payment rates should be set from non-chronically ill (CCI) cases to those of acute care hospitals (ACHs), the savings from which should be redistributed to create additional inpatient outlier payments for CCI.
Payment rates for ACHs’ inpatient and outpatient prospective payment systems in 2015 should be raised by 3.25 percent, so as to be concurrent with the changes made to the outpatient systems and LTCH systems.
Physicians and Other Health Professionals
As members know, the services provided by physicians and health professionals are paid under a fee schedule, with total payments being governed in theory by the sustainable growth rate (SGR). The flawed SGR system has been a continuous concern for MedPAC, and it once again has emphasized the need for its repeal. In making this standing recommendation, MedPAC emphasized the various components it considers when making recommendations regarding physician and other health professional payment updates. Those considerations largely relate to preserving beneficiary access to physician services and maintaining stability for beneficiaries and providers. In the March report, MedPAC made the following recommendations:
Repeal the SGR system and replace it with a 10-year path of statutory fee-schedule updates. Particular emphasis should be placed on including a payment rate update that is higher for primary care services than that of specialty services, so as to reduce the disparity between the two types of providers.
Increase incentives and opportunities for shared savings for physicians who participate in two-sided risk accountable care organizations (ACOs).
Regular collection of data from efficient practices, not just a sample of all practices, to better establish work and practice expense values.
Identify overpriced services and reduce their relative value units (RVUs) accordingly. The identification of overpriced services should be based on the data collected from efficient practices, and not that from a mere sample of all practices.
Beginning in 2015 and following each five consecutive years thereafter, RVU reductions should achieve an annual numeric goal. The goal should be at least 1 percent of fee-schedule spending.
Ambulatory Surgical Centers (ASCs)
According to MedPAC, payment adequacy for ASC services remains positive. This indicator, coupled with the notion that access to capital appears adequate for ASCs, the number of which continues to grow, led the Commission to make the following recommendations:
Eliminate update to payment rates for ASCs for 2015.
Require ASCs to submit cost data on the cost of services they provide to Medicare beneficiaries, so that a Medicare margin, similar to that of other provider types, can be calculated to better assist with determining payment adequacy to ASCs.
Status Report: Medicare Advantage (MA)
In addition to making payment update recommendations to Congress, MedPAC also submits a status report to Congress regarding the MA program. As members are aware, the MA program allows Medicare beneficiaries the opportunity to receive benefits via private plans as opposed to receiving benefits via the traditional FFS Medicare program. The status report provided by MedPAC essentially provides insight on factors such as enrollment trends, plan availability, and payment comparisons between MA plans versus traditional FFS Medicare beneficiaries. This year’s report included the following findings and recommendations:
Enrollment in MA plans increased by nine percent in 2013, which is roughly 28 percent of all Medicare beneficiaries.
Employer group MA plans’ bids and resulting payments should be changed to be more in line with the competitively set bids of nonemployer plans. According to MedPAC, employer group MA plans typically have higher bids than nonemployer plans, largely due to the fact that the employer group plans do not have to attract individual participation. Because of such, the employer group plans often lack any incentive to submit competitive bids. To deter this practice, which will reduce Medicare program spending, MedPAC recommends Congress direct the Secretary of Health and Human Services (HHS) to set payments for employer group MA plans more in line with that of nonemployer plans.
Beginning in 2016, include hospice in MA benefits packages to promote coordinated and consistent care.
The full detailed report along with summaries of recent MedPAC meetings can be found at http://www.entnet.org/Practice/CMS-News.cfm. If members would like additional information on MedPAC, please email the Health Policy team at healthpolicy@entnet.org. 
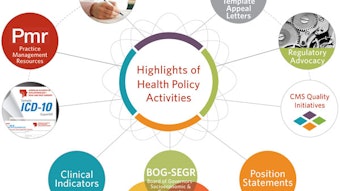
The Academy’s Physician Payment Policy (3P) Workgroup is the senior advisory body to Academy leadership and staff on issues related to socioeconomic advocacy, regulatory activity, coding and reimbursement, and practice services or management. 3P and the Health Policy staff work to ensure that members’ interests are appropriately represented. 3P oversees the review and content for the Clinical Indicators and the Position Statements, provides resources to members such as template appeal letters and CPT for ENT coding guidance articles. Coordination with other Academy committees, subspecialties, and medical specialty societies are critical to 3P’s success.
During the last strategic plan that spanned 18 months (January 2013-May 2014), 3P and the Health Policy team were busy with a continued high level of activity, constant emails and monthly calls, working diligently and tirelessly on behalf of all members. The next year will be no different with efforts focused on the strengths of the Academy: 1) Advocacy, 2) Annual Meeting, and 3) Quality Products (Clinical Practice Guidelines). The Board of Directors agreed to these strengths during the March 2014 strategic planning meeting.
While Health Policy is under the Advocacy section of the strategic plan, the team overlaps and coordinates closely on many related activities with Government Affairs, Research and Quality Improvement, Education, Component Relations (BOG), with support from Member Services, Communications (including Marketing and Graphic Design), and Information & Knowledge Management units.
The Health Policy team will continue to work closely with other team units within the Academy to collaborate to meet the measurements of success. Examples of collaborating with other teams to meet Academy goals include:
Government Affairs—Provided input on the health policy language included in the SGR payment reform legislation, developing the AAO-HNS position.
Research and Quality Improvement—Advocacy efforts with CMS resulted in the inclusion of four new adult sinusitis measures for PQRS reporting in 2014.
Coding & Reimbursement—Provided input on the content of the AAO-HNSF Coding Workshops conducted by Karen Zupko & Associates.
Component Relations (BOG)—Developed a 3P/BOG SEGR Communication Flow Chart outlining the socioeconomic issues that will be addressed at the local level by the BOG, or by 3P and the Health Policy team at the national level.
During the course of the next strategic plan, which will cover a one-year period, from July 2014 to June 2015, 3P and the Health Policy team will help the Academy be a powerful voice in influencing legislative, political, regulatory, health policy, and third-party payer policies, seeking ways to increase member awareness of and involvement in these critical advocacy activities. Below are the two goals of the health policy unit with the main focus on the following actions as they assigned priority by the Board of Directors. This does not mean the 3P and the Health Policy team will not continue to provide other services. However, it does mean that activities under these goals will take precedence over other activities.
Goal 1: Integrate health policy-specific priorities, using input from the 3P Workgroup, to maintain our visibility and credibility with national representatives regarding socioeconomic and federal regulatory issues.
ACTIONS
Advocate for relevant and validated quality and cost measures, and develop guidance on payer quality initiatives.
Develop a more refined approach to CPT/RUC code participation, working more effectively with industry partners.
Integrate priorities of quality knowledge products with code development and payer coverage needs.
Analyze trends and developments in payment reform and influence the payment and delivery system reform.
Goal 2: Advocate for appropriate reimbursement and fair policies with Medicare and private payers, providing members with information and guidance on reimbursement issues encountered at the state and local level.
ACTIONS
Provide guidance for members at the state and local level to advocate for appropriate payment.
Develop guidance on coding and practice management resources to physician leaders.
Provide coding guidance (i.e., ICD10 transition, new codes, etc.) and develop educational resources.
The 3P and the Health Policy team look forward to working on these priority issues during the next year. Updates on the action items will be provided in a future Bulletin article. For questions, please email the Health Policy team at HealthPolicy@entnet.org. Robert M. Portman, JD, MPP*
The Physician Payments Sunshine Act (PPSA or Sunshine Act), now being implemented as the Open Payments program, is upon us. The primary purpose of the program is to shed light on the financial ties between the healthcare products industry and physicians. Most physicians know this law is going to require public reporting of their financial relationships with drug and device companies, but many doctors have less than a full picture of what the law requires and how it will affect them. This article summarizes the key provisions of the final PPSA rules that were issued in 2013 by the Centers for Medicare and Medicaid Services (CMS) and provides answers to frequently asked questions about the Open Payments program. While the final rule covers the reporting obligations of both manufacturers and GPOs, this article will focus only on the obligations of manufacturers. Much more information about the program can be found at the Open Payments website at go.cms.gov/openpayments.
Summary of Final Rule
The PPSA rules impose two types of reporting requirements on “applicable manufacturers,” defined as those companies that manufacture a Medicare, Medicaid, or Children’s Health Insurance Program (CHIP)-covered drug, device, biological, or medical supply and whose products are sold or distributed in the United States. First, they require any applicable manufacturer to report transfers of value to a physician or teaching hospital, which the final rule refers to as “covered recipients.” Second, applicable manufacturers are required to report separately any physician ownership and investment interests and payments of value to physician owners, investors, and immediate family members, including spouses, children, parents, siblings, and other close relatives (but note that the names of family members do not need to be reported, just the physician’s name). This includes physicians with an ownership interest or stock with an applicable manufacturer, regardless of the amount, but only where the manufacturer is aware of such ownership interest. Failure to adhere to these reporting requirements may result in civil monetary penalties for manufacturers.
The final rule requires manufacturers to report a transfer of anything of value to a covered recipient, regardless whether it was requested, to a physician or teaching hospital. “Anything of value” includes:
Cash or cash equivalents
Space rental or facility fees
In-kind items or services
Stocks, stock options, or any other ownership interests, dividends, profits, or other returns on investments
The rule outlines a number of exclusions from the reporting requirements, including but not limited to:
Transfers of value of less than $10 unless the aggregate amount over a year exceeds $100, with an exception to the aggregation requirement for pens, notepads, and other de minimis items provided at conferences or other large scale events;
Product samples intended for patients;
Educational materials that directly benefit patients;
Discounts or rebates;
Payments to speakers and tuition discounts for attendees at certain accredited CME events; and
In-kind items for charity care
Applicable manufacturers must report the name, date, NPI, state license number, specialty, and address of the entity or individual receiving the payment to CMS. The report must specify the amount of the payment, the nature of the payment (such as consulting fee, food, entertainment, travel, education, or research), and the form of payment (such as cash, stock, stock option, or in-kind items or services).
Once the data is submitted to CMS, the agency aggregates and sorts it by individual covered recipients and provides them with 45 days to review and dispute manufacturer reports and another 15 days for manufacturers to submit corrections. CMS will publish the reports in a publicly searchable database on the Open Payments website with the individual physicians’ names and information and whether the report is disputed.
Frequently Asked Questions about the Open Payments Program
Scenario EXAMPLE. What kinds of final relationships with manufacturers are reportable?
The Sunshine Act covers virtually any kind of direct or in-kind remuneration from a manufacturer to a physician or teaching hospital, including:
Consulting fees
Compensation (services other than consulting, includes serving as faculty or as speaker at an event other than a continuing education program)
Honoraria
Gifts
Entertainment
Food and beverage
Travel and lodging
Education
Text books and journal reprints
Research
Charitable contributions
Royalty or license
Current or prospective ownership or investment interest
Compensation for serving as faculty/speaker for unaccredited and non-certified continuing education program
Direct compensation for serving as faculty/speaker for accredited and certified continuing education program
Grants
Space rental or facility fees (teaching hospital only)
Stock or stock options
Scenario EXAMPLE. If a manufacturer pays for lunch at our group practice, but I don’t attend or don’t eat the food, will I still be reported?
No, only those who attend and partake of the meal will be reported—assuming that the meal is more than $10 in value. The value of the meal must be calculated on a per-person basis, including all attendees, not just physicians.
Scenario EXAMPLE. I’ve heard that if I eat a meal at an industry-sponsored AAO-HNS/F meeting or receive an AAO-HNS/F research grant funded by a drug or device company that my name might be reported to CMS, is that true?
Yes, the Sunshine Act requires manufacturers to report indirect transfers of value to physicians through third parties, like medical societies, when the manufacturer directs, instructs, or otherwise causes the medical society or other organization to provide the payment to the physician and the manufacturer knows or easily could ascertain the identity of the physician recipient(s). If a manufacturer sponsors a dinner at the AAO-HNS/F Annual Meeting, the per-person value of that dinner would have to be reported for all of the physician attendees. Likewise, if a manufacturer funds a research grant that is administered by AAO-HNS/F to be awarded to an AAO-HNS physician member, the value of the grant would be reportable for the physician awardee.
By contrast, if the manufacturer gives AAO-HNS/F an unrestricted grant for the Annual Meeting, (i.e., without specifying how the money should be used), and AAO-HNS/F decides to use some or all of those funds to subsidize a dinner at the Annual Meeting, that would not be reportable because the manufacturer did not cause the funds to be used to transfer something of value to physicians. [Cautionary note: some manufacturers are taking a very conservative interpretation of the Open Payments rules and are saying they will report even unrestricted grants if they learn that the money was eventually used to make indirect transfers of value to physicians and they can easily identify the physician beneficiaries; even though they did not cause the funds to be transferred to a physician.] Similarly, an industry-funded lunch buffet in the Annual Meeting exhibit hall would not be reportable because it would likely constitute a “large-scale event” for which the identity of the physician beneficiaries could not be easily ascertained.
Payments to physician faculty and tuition discounts for attendees of manufacturer-funded CME are not reportable if the event is accredited by, among others, the Accreditation Council for Continuing Medical Education, the American Medical Association, the American Osteopathic Association, or the AmericanAcademy of Family Physicians. Under this exception, the manufacturer also may not have any role in picking speakers or content and cannot pay the faculty or attendees directly. This exception would not cover any meals or other kinds of transfers of value provided to the attendees of accredited CME events.
Scenario EXAMPLE. Is AAO-HNS/F required to provide my name and other information to industry sponsors if I receive an indirect transfer of value through the Academy or Foundation?
Technically, medical societies like AAO-HNS/F are not covered by the Sunshine Act and therefore do not need to provide information to industry about indirect transfers of value to their physician members. But, future industry funding is likely to be conditioned on such cooperation; and if AAO-HNS/F does not provide the information, manufacturers will report based on their best guess of the identity of the physician recipients and the value of the benefit. This could lead to wildly inaccurate reporting by industry and cause even bigger problems for AAO-HNS members.
Scenario EXAMPLE. Can I avoid being reported by redirecting payments to charities or friends and family?
No, if a physician redirects an industry payment to a family member, friend, or favorite charity, the law still requires the manufacturer to report the payment as if it has been made to the physician directly. However, the third party does not need to be reported.
Scenario EXAMPLE. Will I have a chance to review and dispute reports about me?
Yes, as noted above, the Open Payments program gives physicians a 45-day window to review and dispute reports about their financial relationships with, or ownership interests in, manufacturer companies. During this period of time, the physician can contact the manufacturer and try to persuade the company to change or remove the report. The manufacturer then has 15 days to correct the report. But, if the manufacturer refuses to do so, CMS will only mark the report as disputed; it will not remove it or otherwise arbitrate the dispute.
Scenario EXAMPLE. When are these reporting requirements effective?
Manufacturers were required to start collecting data as of August 1, 2013 and needed to submit data through December 31, 2013 to CMS by March 31, 2014. The Open Payments public database goes live on September 30, 2014. In future years, the website will post reports by June 30 for the previous year’s data.
Scenario EXAMPLE. What can I do to protect myself from inaccurate reports or explain my industry relationships to patients?
Physicians and their practice groups should track and retain their own records of items of value received from manufacturers to ensure they are prepared to evaluate and challenge the accuracy of reports that include them. (Note that the Open Payments website is offering a mobile app to assist physicians in tracking their industry relationships.) With only a 60-day period for dispute resolution and no independent review, physicians need to respond quickly to improve the chances of resolving discrepancies. Failure to resolve a dispute will lead to publication of a manufacturer’s report “as is,” albeit in some cases with a note that the report is disputed. But physicians will have no opportunity to publish an explanation of their position.
CMS recommends that all covered recipients register on the agency’s website. Registration supposedly will ensure that CMS will notify physicians in a timely manner after the manufacturer submits a report so that the physician will have an opportunity to check to see if his or her name has been included and, if necessary, dispute the report. CMS will not notify physicians when their particular name has been reported. It will be up to each physician to search the database for their name or NPI number. In this regard, it will be critical that CMS and manufacturers have the physician’s current name and NPI number to avoid inaccurate reports.
Physicians would also be well advised to develop talking points to use in responding to questions from patients, colleagues, and, in some cases, the media, about their industry relationships. They may also want to preempt such questions by putting information about their relationships with industry on their practice website or in other patient communications.
Robert M. Portman, JD, MPP, is an association and healthcare attorney with Powers Pyles Sutter & Verville PC in Washington, DC. He also serves as legal counsel for AAO-HNS/F. This article is provided for informational purposes only and does not constitute and should not be treated as legal advice. Opposition to federal legislation designed to inappropriately expand the scope of practice of audiologists has long been one of the AAO-HNS’ key legislative priorities. For years, the national organizations representing the audiology community sought passage of federal legislation that would provide audiologists with unlimited “direct access” to Medicare patients without a physician referral. However, in late 2012, we learned the audiology community was no longer coalesced around the direct access issue, and the three groups representing audiologists would instead pursue separate legislative initiatives. As expected, dueling pieces of audiology legislation have been introduced in the 113th Congress, with yet another bill on the horizon. They are:
American Academy of Audiology (AAA)—H.R. 4035/S. 2046, a recycled bill to provide audiologists with unlimited direct access to Medicare patients without a physician referral. Introduced in February 2014 by Rep. Jim McDermott (D-WA) and Sen. Sherrod Brown (D-OH). AAO-HNS opposes.
American Speech-Language-Hearing Association (ASHA)—H.R. 2330, a bill designed to align Medicare coverage of comprehensive audiology services with current billing and reimbursement standards of other non-physician therapeutic services covered by Medicare (PT, OT, SLP). This bill specifically retains the requirement for a physician referral, as well as physician oversight of plans of care. Introduced in June 2013 by Rep. Gus Bilirakis (R-FL). AAO-HNS supports.
Academy of Doctors of Audiology (ADA)—Legislation not yet introduced. Expected to move forward with its new “18 x 18” campaign—an effort to pass legislation by 2018 that would amend Title XVIII (18) of the Social Security Act to include audiologists in the definition of “physician.” This new initiative would also provide direct access similar to the AAA legislation and the comprehensive benefits outlined in the ASHA proposal. AAO-HNS will oppose.
The shift in the audiology community’s strategy is not an anomaly. Since passage of the Affordable Care Act and the President’s subsequent reelection, there has been a slightly more favorable environment on Capitol Hill regarding efforts to expand access to non-physician healthcare providers to help fill perceived gaps in care.
Given these evolving legislative “environment” variables, and the strategic shift within the audiology community, the AAO-HNS has remained proactive in its approach to ensuring Members of Congress (and their staffs) are well educated on the various audiology initiatives. In addition to several AAO-HNS letters to Capitol Hill and numerous meetings with legislative and committee staffs, the Academy spearheaded two coalition sign-on letters opposing the direct access effort (H.R. 4035/S. 2046). We are pleased to report that nearly 110 national, state, and local medical societies—including the American Medical Association and the AmericanCollege of Surgeons—are signatories to our letters.
Thus far, our efforts have received a positive response from many Capitol Hill offices. However, our success should not breed complacency. The AAO-HNS urges its members to follow these issues closely. As these legislative efforts continue to unfold, applicable legislative “action alerts” and other advocacy-related materials will be communicated to AAO-HNS members.
For more information regarding audiology legislation in the 113th Congress, contact legfederal@entnet.org. Or, visit the Legislative and Political Affairs webpage at www.entnet.org/advocacy for access to the Academy’s position letters and/or additional resources pertaining to these issues. Are you tired of hearing about the “SGR” yet? By now, the answer is probably “yes.” The SGR, or Sustainable Growth Rate, formula used to determine payments to physicians in the Medicare program is the proverbial “thorn in the side” federal legislative issue for physicians. For more than a decade, the physician community has urged Congress to permanently repeal the flawed formula, and this spring was supposed to be “the time.” Unfortunately, Congress (again) lacked the political will to make this generally despised issue disappear. Read on for an overview of the past, present, and future outlook for ridding the House of Medicine of this flawed formula that continues to wreak havoc on physicians and patients within the Medicare program.
Past: What is the SGR and Where Did It Come From?
The SGR became law as part of the Budget Control Act of 1997, and was intended to act as a mechanism to ensure that the yearly increase in the expense per Medicare beneficiary did not exceed the growth in GDP (gross domestic product). However, one inherent flaw of the formula is that it assumes a positive correlation between the GDP and Medicare spending. So, in a strong economy, GDP and spending would theoretically grow at a similar rate and payments would remain positive. However, in a weaker economy, when spending exceeds the GDP, the formula is designed to trigger reductions in Medicare physician payment rates.
The triggered reductions came to fruition in the early 2000s and have resulted in an annual exercise of intense lobbying from the physician community to spur Congressional action to prevent (usually at the last minute) the payment cuts. Congress has prevented scheduled cuts from going into effect each year except for 2002, when physicians absorbed a nearly five percent cut in their Medicare payments. Compounding the complexity of this issue is the cumulative nature of each year’s scheduled cut. In basic terms, Congress’ proclivity for short-term remedies for this long-term problem means that with each year’s payment “patch,” the percent of the next year’s cut, and the estimated cost of repealing the formula, grows.
Present: The “Stars Aligning” (February 2013 through Spring 2014)
Since the SGR emerged as an annual issue for Congress, there has been broad (and growing) bipartisan support for permanently repealing the flawed formula. However, two issues have regularly been blamed for thwarting these efforts. First, lack of agreement from the physician community regarding what type of payment policy should replace the SGR. Second, simply put, cost. Despite these challenges, the “stars began to align” in early 2013 (see box next page), and it became widely believed that the year that the SGR issue would finally—and permanently—be resolved had arrived.
First, leaders from the Congressional committees with jurisdiction over Medicare collectively stated in early 2013 that repealing the SGR formula would be their top priority for the year. These statements spurred an ongoing dialogue between Capitol Hill and the physician community in order to craft, and eventually coalesce around, a new payment model designed to better incentivize the delivery of high-quality, efficient healthcare. Around the same time, the Congressional Budget Office (CBO) released an updated projection of the estimated cost of SGR repeal—reducing the amount to $138 billion during 10 years. Previous estimates had scored SGR repeal at more than $300 billion.
Throughout the remainder of 2013, efforts to repeal the SGR continued. By year’s end, the House Energy and Commerce (E&C), House Ways and Means (W&M), and Senate Finance Committees had each unanimously passed versions of the SGR repeal policy that had evolved with input from the physician community, and lawmakers agreed they would likely only need a couple of more months to finalize offsets for the permanent package. As a result, Congress passed an amendment to the Bipartisan Budget Act of 2013 to halt (for three months) the 24 percent cut in Medicare physician payments scheduled for January 1, 2014. Instead, physicians received a .5 percent positive increase during that time. This payment “bridge” was intended to avoid payment disruptions as Congress completed its work on permanent SGR repeal legislation during the first several months of 2014.
Initially, it seemed as though Congress was poised to keep its word in terms of continuing to work on the SGR issue in the new year. In February, the aforementioned Congressional committees announced they had successfully negotiated the “melding” of the policy included in their respective SGR bills and that conversations to identify the necessary offsets for the bill could/would begin. Unfortunately though, the introduction of the finalized bill coincided with the departure of one of SGR repeal’s key champions, Senate Finance Committee Chairman Max Baucus (D-MT). Ultimately, Chairman Baucus’ departure (to become Ambassador to China) acted as a double-edged sword for ongoing SGR efforts. It spurred the final bill to be introduced, but it also delivered a serious blow to the momentum needed to actually achieve final passage of a bipartisan, bicameral permanent SGR repeal package (H.R. 4015/S. 2000).
In the weeks following, the necessary offset negotiations failed to materialize and leaders in the U.S. House of Representatives opted to put forth a partisan offset (delay of the ACA individual mandate) as the key funding for H.R. 4015, and passed the bill on March 14. While many lawmakers argued their strategy was simply to pass the bill from the chamber, the partisan politics slowed action in the U.S. Senate. Dueling bills were subsequently introduced in the upper chamber, using equally partisan offsets. As a result, the likelihood of permanent repeal by the March 31 deadline began to fade, and Congressional leaders began preparing a 12-month SGR patch, the decade’s 17th temporary fix.
In an unprecedented move, the physician community, including the AAO-HNS, reacted to the Congressional leadership’s “bait and switch” by actively opposing the proposed 12-month patch, and instead urged lawmakers to continue work on the policy agreement that had previously been negotiated. Unfortunately though, House leaders ignored the pleas from the physician community, and on March 27 resorted to unprecedented stealth floor tactics to force a voice vote on the patch and avoid an “on the record” vote tally. The U.S. Senate followed suit on March 31, passing the temporary SGR bill by a vote of 64-35. The President signed the bill into law soon thereafter.
Future: Hard to See an Immediate Path Forward
Despite Congress’ claim that the large price tag (currently about $150 billion) associated with permanent SGR repeal remains its greatest roadblock, the fiscal reality is that the total price of all the SGR patches to date exceeds the cost of permanent repeal. And, another patch only increases the price of any future effort to permanently repeal the flawed SGR formula.
Most importantly, the length of the negotiated patch seriously diminishes the likelihood of permanent repeal in the near future. Although Congressional leaders claim efforts to permanently repeal the SGR formula can still be advanced in the coming months, several variables—mid-term elections, a lame duck Congress, followed by potential leadership changes in the 114th Congress—raise serious doubts about the viability of advancing a permanent package before another patch would be necessary in March 2015. The AAO-HNS is extremely disappointed with the inability of Congress to deliver on its promise to seek bipartisan offsets for the permanent SGR bill. Congress missed a critical opportunity to—finally—provide stability for the nation’s seniors and physicians participating in the Medicare program.
Interested in more information? Contact legfederal@entnet.org with specific questions regarding the process and policy outlined above. In addition, visit the Legislative and Political Affairs webpage at www.entnet.org/advocacy to view the Academy’s SGR comment letters and/or additional information about the negotiated policy to repeal the SGR. 
What do you see as the priorities of the Nominating Committee in selecting the future leaders of our Academy?
C. Gaelyn Garrett, MD
We are in the midst of exciting yet daunting changes in medicine. As physicians, we should be leading the charge to insure that these changes positively impact our primary goal of providing the highest standards of medical care to our patients. The American Academy of Otolaryngology—Head and Neck Surgery (AAO-HNS) is uniquely positioned to provide the resources and support to accomplish this goal. The strength of the AAO-HNS is clearly its fellow members; as a member of the Nominating Committee, I will seek leaders who are forward thinkers and motivators of the membership to foster the relationship between clinicians and policymakers. Rather than be stymied by these challenges, our leaders will embrace the opportunities to build on what is successful and redirect what is not. With that positive relationship, the AAO-HNS can continue to be our advocate for advancing our primary missions of patient care, education and scientific innovation. We are physicians first—but we need to recognize the necessity for expanding our influence beyond the clinical realm. Our future Academy leaders will continue to help us lead this charge.
Stacey L. Ishman, MD, MPH
I believe we must select physician volunteers who have a commitment to service, an understanding of the issues affecting medicine, and the integrity and passion to carry out this important work. Our academy is blessed with a multitude of talented and collaborative members and it is the job of the Nominating Committee to select the best of this gifted group. I feel that an ideal candidate should have the vision to continue our Academy’s national leadership on quality and patient outcome efforts while remaining aware of the diverse perspectives that are necessary to represent our broad constituency.
My experiences in the Academy have helped me to understand effective leadership qualities. I have been highly involved in the Board of Governors and currently serve on the Executive Committee as the Member-at-Large. I have been a member of multiple Academy committees as well as the Advisory Council for Quality and the Guidelines Development Taskforce. I have also served locally as the President of the Maryland Otolaryngology Society and Surgical Director of a multidisciplinary UpperAirwayCenter at Cincinnati Children’s Hospital. I would appreciate the opportunity to use this knowledge and serve my fellow otolaryngologists as a member of the Nominating Committee.
Albert L. Merati, MD
Future AAO-HNS leadership must recognize and address evolving trends in membership as the next generation of otolaryngologists is increasingly likely to self-identify as subspecialists.
The future leaders of the AAO-HNS must understand what will always be the heart of otolaryngology practice—the general otolaryngologist—but also recognize that the nature of the membership is changing.
Otolaryngology program graduates (naturally the largest growth area for AAO-HNS membership) are increasingly likely to pursue fellowship training and enter group practices as their designated “ear” person or “nose” specialist. Already happened in your practice? Or the practice down the street?
The AAO-HNS will be affected by this trend: our capacity for patient and practice advocacy depends on preserving meeting and membership revenue. The budget choices made by leadership will reflect the needs and demands of paying members. If the growing group of self-identified subspecialists loses the sense of connection to the AAO-HNS as a group, our power to make the positive impact as outlined in our mission will be compromised.
As a member of the Nominating Committee, I will use my experience connecting with thousands of members in practices all over the U.S. to help keep all members in mind while submitting names for election.
Rodney Taylor, MD, MSPH
The task of the Academy’s Nominating Committee is to provide a dynamic roster of the best individuals for its members to select a leadership team that can harmoniously navigate the Academy through our current and future challenging environment. The responsibility of selecting our leaders is second only to actually providing the leadership that will be essential to the ongoing success of our Academy.
The navigators of our Academy should be bright and sympathetic individuals who are uniquely passionate and engaged in providing guidance for a subspecialty of surgeons widely considered among the most talented and well-rounded physicians in medicine. Our leaders should distinguish themselves for outstanding character, vision and integrity; individuals who unhesitatingly demand justice with a clarion voice, and have the experience to represent the compelling interests and wonderful diversity of our wide-ranging members. If I am elected for this crucial role, I will be dedicated to providing a leadership roster that will be the most capable and committed group to direct our Academy going forward. 
Given the uncertainty of today’s healthcare environment, what do you perceive as challenges and possible solutions to implementing the Academy’s strategic plan?
Carol R. Bradford, MD
There is no question that our members are facing unprecedented challenges in today’s healthcare environment. The era of healthcare reform, the intrusion of the electronic medical record, and the fear of changing models for reimbursement all seem to threaten the ideals we hold dear: our commitment to deliver the best patient care and our aspiration to improve the health of all people suffering from ear, nose, and throat diseases. It is clear that our future success is dependent upon our collective ability to deliver and measure value (outcomes/cost). Our Academy is well positioned for this future with its advocacy for relevant and validated quality and cost measures and its efforts to develop guidance about value-based purchasing and meaningful use of the EMR, among many other efforts. It is essential that the AAO-HNS remain proactive in addressing the rapid pace of the changing healthcare environment and serve its members by advocacy, quality, and educational efforts.
If elected, I aspire to be a servant leader. I will listen and serve the robust membership of this society in order to allow us to reach our vision of empowering otolaryngologist-head and neck surgeons to deliver the best patient care.
Cherie-Ann Nathan, MD
This is a stressful time for our members with the looming perfect storm of ACA, ICD-10, and pay-for-performance. Never before in the history of our profession have so many changes occurred in so many areas in so short a time. I am honored by this nomination and will help the Academy rise to the challenge of helping our members cope with these dramatic sea changes.
Using my leadership experience gained by serving on numerous national committees not only in the Academy, but also the AHNS, ASCO, NCI Task Force, and HNCA, I believe I can help the Academy navigate us through these difficult times in the following areas:
Best practice guidelines, outcome measures, consensus statements
Understanding and implementing ICD-10
Preparation for ACA and pay-for-performance
Customized educational activities
Real-time mobile app updates
Supporting research to publish studies that will help guide best practices
I would encourage the board to give monthly updates on each problem area: ACA/ICD-10, best practice guidelines, fiscal issues, and cutting-edge information. Having been on CORE, I would promote research efforts toward outcome measures and technologies for personalized medicine in cancer that will cut cost and improve survival. I will spearhead efforts to promote large multicenter trials for evidence-based, cost-effective treatments that emphasize patient safety—options that third-party payers covet.
These are challenging times indeed, and our Academy, as one of the most progressive specialty societies, is uniquely positioned to lead the way for a new era in physician advocacy and leadership. 
What is your particular experience or interest that would make you an effective member of the Audit Committee of the Academy?
It is my great pleasure to run for re-election to the Audit Committee of the AAO-HNS. The committee’s important role is to confirm that the budget is aligned with the Academy’s strategic plan. This is a critical mission that ensures greater accomplishments in the future so an Audit Committee member should have a global understanding of the Academy’s function, as well as training in the ability to evaluate financial statements. I have both of these requirements, and I also have a passion for the Academy. As an active member in committees, associate editor for the journal, CORE grant reviewer, and involved with presenting at the scientific and research programs, I believe that I have a great understanding of the value of this work. Adding to this perspective is my devotion to these and other activities outside the Academy, such as instruction courses, resident and fellow education at the Mount Sinai Medical Center, publishing, and community involvement. I am also the upcoming treasurer of the American Laryngological Association, and have a background in accounting and finance from a recent program in Managing Healthcare Delivery at Harvard Business School. I look forward to the opportunity to serve on this committee. 
What is your particular experience or interest that would make you an effective Secretary-Treasurer of the Academy?
Rahul K. Shah, MD, MBA
It is an honor to be nominated to serve as the Secretary-Treasurer of the AmericanAcademy of Otolaryngology—Head and Neck Surgery. I have dedicated much of my professional career during the past two decades to advocacy and leadership through the AAO-HNS. I have served as co-chair of the its Patient Safety and Quality Improvement Committee and as chair of the Advisory Council on Quality. I have also twice co-chaired the Home Study Course Section 2. I have also served on myriad other official and ad hoc Academy committees and working groups. My work with the Academy has been recognized with the Honor Award and the Distinguished Service Award.
I received a combined BA/MD from BostonUniversity and completed my residency at TuftsUniversity with a fellowship in pediatric otolaryngology at Children’s Hospital Boston. I completed my MBA with a healthcare focus at the GeorgeWashingtonUniversity. I am an associate professor of otolaryngology and pediatrics at the GeorgeWashingtonUniversity.
My leadership activities extend outside the Academy as well. On an international level, I am the Executive Director of the Global Tracheotomy Initiative. I have played an instrumental role in its accounting, budgeting, forecasting, governance, and overall structure. On the hospital level, I am the President of the Medical Staff and Associate Surgeon-in-Chief at Children’s NationalMedicalCenter in Washington, DC, and hold various other leadership positions within our hospital including Medical Director of Peri-Operative Services. In my position as the Associate Surgeon-in-Chief, I am responsible for the safety, quality, efficiency, and finances of the peri-operative services, a major revenue driver for the organization.
The role of Secretary-Treasurer carries significant fiduciary duties that require a deep understanding of the accounting, finances, and investments of the American Academy of Otolaryngology—Head and Neck Surgery. I have a penchant for such and am confident that as the Secretary-Treasurer, I will be an excellent steward of Academy resources. My internal and external portfolios of experiences have helped me to build the foundation of skills required to serve as the Academy’s Secretary-Treasurer.
I realize that this position demands more than just a requisite skill set. Healthcare reform is complicated, can be confusing, and is in constant flux. The Secretary-Treasurer and the Board of the Academy must be nimble and adaptable to prepare our organization for what the next decade will bring. Our current and past Academy leadership has done an amazing job of staying focused through this tumultuous healthcare climate while continuing to deliver value for our Members. I am confident that I have the necessary time, resources, and passion to successfully serve as your Secretary-Treasurer through the challenges that lie ahead.
Scott P. Stringer, MD, MS
I have had the opportunity to serve in leadership roles throughout the Academy, organized medicine, health systems, and academic medicine, which give me a broad perspective and background from which to contribute as Secretary-Treasurer of the Academy. My administrative medicine master’s degree and my extensive healthcare leadership experience have prepared me to quickly understand strategic, financial, personnel, and organizational issues that face organizations like ours.
Service on a variety of Academy committees and in elected Academy offices gives me an excellent perspective on our organization. As chair of the Rhinology and Paranasal Sinus Committee, I have been intimately involved in the interface between vendors, payers, and our organization. It has allowed me to be closely involved in the development of Academy policy. My service on the Audit Committee, including two terms as chair, allows me to better understand the finances of the Academy.
I have had the opportunity to manage the financial affairs of large organizations in my career, which is important to success in the position of Secretary-Treasurer. As chair of an otolaryngology department, I oversee a budget of approximately $17 million. I have also served as Associate Vice Chancellor for Clinical Affairs and president of the board of our 662-member faculty practice plan. In these roles, I was responsible for a healthcare system with combined revenues of approximately $1 billion.
Leadership opportunities in a number of specialty societies and in organized medicine provide me with a broad understanding of issues facing our membership. As president of both the Association of Academic Departments of Otolaryngology and the Society of University Otolaryngologists-Head and Neck Surgeons, I have developed broad and diverse relationships throughout our specialty that will allow me to better represent our membership. As a long-term member of the Council of Faculty and Academic Societies of the Association of American Medical Colleges, I have a broadened understanding of healthcare issues beyond our specialty, which is important for our success in working with other specialty organizations in support of issues of importance to our membership. I have also served as secretary-treasurer and subsequently president of both my county medical society and my state otolaryngology society.
I welcome the opportunity to give back to our specialty and to my mentors, colleagues, and trainees by serving and contributing as Secretary-Treasurer. I am thankful that I was fortunate enough to join a specialty that I love and to have so many colleagues that I admire and respect. I have been able to gain leadership experience and skills by serving in a wide variety of roles in organized medicine, academic medicine, and a number of our specialty societies. It is my duty and would be my pleasure to use these experiences to serve my specialty and my colleagues. I believe that I can make a positive difference on behalf of our specialty and the patients that we serve. 
Sujana S. Chandrasekhar, MD
These are challenging times in medicine, and especially in otolaryngology. It seems with every breath there is another arrow of uncertainty headed our way, whether it is ACOs, patient satisfaction surveys, decreasing reimbursements, education for MOC, healthcare reform rollout, ICD-10, or internal divisions between subspecialties, practice types, etc.
Navigating these challenges requires experienced leadership. I have practiced successfully in two academic settings, and for the past 10 years I have had a successful solo private neurotology practice while working part-time at the VA and building a new multidisciplinary clinical program within a large hospital system. With my Academy experience as past Board of Governors (BOG) chair, at the Board of Directors (BOD), in education, advocacy, development, and with the Women in Otolaryngology (WIO), Diversity, and Young Physician Section (YPS), I have a good understanding of the needs of the entire otolaryngology community.
If I become President-Elect, my three goals will be:
1. Increase member participation in all areas of the Academy
It is disheartening to hear members say that they don’t see value in their membership, that they don’t need the Academy or the meetings, that they are only involved in their subspecialty, or that they think that ENT is so small that we can’t make a difference. What we’ve got here is a failure to communicate.
As President-Elect, I would like to harness our website to enhance member and committee communications, to go to where the members are, and to find out who’s not participating and why. Our Member Handbook highlights educational, financial, and advocacy benefits of membership and must reach all otolaryngologists. I would continue to strengthen our working relationship with subspecialty ENT societies. We thrive by identifying and mentoring future leaders, whether they are residents or fellows or well into their careers. That is one of my passions.
2. Strengthen the Academy’s position as a leader in organized medicine
Despite its relatively small size, our Academy has been a leader in organized medicine. We are strong with legislators and we collaborate with the larger house of medicine on key issues. We lead in Guideline development and at the Choosing Wisely® campaign.
As President-Elect, I will work with the new EVP/CEO to strengthen our leadership position and to spearhead efforts that help our members thrive financially by making it as easy as possible to comply with upcoming regulations, including establishing ENT-pertinent quality measures. With 100 percent participation in the PAC, we can show our strength on Capitol Hill.
3. Make the Academy’s website the go-to site for ENT information
Fifty percent of all doctor visits are for ENT problems. Our Academy has vetted teaching materials, but they are hard to access. As President-Elect I would work to expand mobile access to our website so that when physicians or patients search for detailed ENT information, they come to our site. This would also help our members serve their patients better while practicing more efficiently.
It has been a pleasure serving the Academy for all of these years, and it would be an honor to serve as its President.
J. Pablo Stolovitzky, MD
My first and foremost goal as president is to empower our members to face the most significant healthcare reform we have ever confronted. Never has the Academy been more important to the future of our specialty.
The paradigm shift from fee-for-service to value-based payment is on the horizon. How do we address this challenge?
I Will Set a High Priority to:
Develop specialty-specific quality measures and value payment models or they will be developed for us.
Educate and empower otolaryngologists participating in Accountable Care Organizations (ACOs) to negotiate equitable bundled payments.
Vigorously advocate for our members on healthcare reform issues affecting our specialty.
My experience as a member of the Ad Hoc Payment Model Workgroup has enabled me to evaluate trends in healthcare payment reform and to develop practical methods for participating in new models.
Through these contributions, the Academy will empower our members to retain equitable payment and thrive as we navigate healthcare reform.
My Second Goal Is Specialty Unity.
We must align strategies with our subspecialty societies to speak with a stronger voice.
We should collaborate to develop quality measures and MOC materials to achieve economies of scale.
My third goal, which will extend into my past-president year, is to secure sustainability.
Our strategic plan prepares us for change, but requires significant revenue.
Five years on the Financial and Investment Subcommittee provided me with a thorough understanding of the Academy’s budget process and its relationship to strategic initiatives, giving me excellent insight in securing sustainability.
I Will Work Diligently to:
Support development initiatives
Increase alternative revenue streams
Expand our international membership
Increase opportunities for members abroad to purchase annual meeting content. My experience on the International Steering Committee and my relationship with International Leadership gives me a unique perspective to achieve this goal.
As President-Elect, I Will Increase Members’ Engagement and Value by:
Improving our website for mobile access to
Educational activities
Expanded clinical research
Otolaryngology-specific EMR tools
Enhancing our two-way communications with members through the newly launched ENTConnect and social media
Synergizing our constituencies:
Board of Governors (BOG)
Specialty Society Advisory Council
Women in Otolaryngology (WIO)
Young Physicians, Residents, and Fellows (YP, and SRF)
Now more than ever, the Academy needs a president who has the skills and experience to lead our members to adapt and succeed through challenging times.
My Leadership Experience Includes:
Co-founder and CEO of a thriving practice with 20 otolaryngologists
Clinical faculty at Emory University, which gives me a unique perspective of both private practice and academic otolaryngology
Multiple Academy leadership roles:
Secretary and Chair of the Board of Governors
Director on the Board of Directors
Executive Committee of the Board of Directors
My vision is to engage and empower our members, while enhancing our core mission of education, advocacy, and research.
I am confident that my leadership experience, long term involvement in organized medicine, successful practice, and my academic and business expertise have prepared me to lead the Academy.
I would be deeply honored to serve as your president. As Members it is the privilege and responsibility of all to vote for future leadership. The following pages present the official statements of the candidates. Note in the box on this page the details of the voting process. Voting eligibility is outlined in the AAO-HNS/F Bylaws, and reads:
Categories of Membership and Voting
There shall be the following categories of membership in the Academy: Fellows, Life Fellows, Retired Fellows, International Fellows, Inactive Fellows, Honorary Fellows, Scientific Fellows, Members, Life Members, Retired Members, Inactive Members, International Members, Resident Members, International Resident Members, Associate Members, and Affiliate Members. The eleven (11) categories of membership entitled to vote on any matter shall be Fellows, Members, Fellows in Training, Members in Training, First Year Fellows, First Year Members, Scientific Fellows, Life Fellows, Life Members, Retired Fellows, and Retired Members. The phrase “voting Fellow or Member” used in these Bylaws shall mean only persons within those eleven categories of membership cited above.
Each President-Elect candidate responded to three questions posed by the Nominating Committee. They are:
During your term as president, what three goals would you like to accomplish that would position our Academy best for the future? What would you do as president-elect to lay the groundwork for fulfilling these goals, and what would you do as immediate past-president to promote a lasting benefit?
How would you lead our Academy in adapting to healthcare reform through advocacy, quality initiatives, and member engagement? In what ways could the Academy best empower members to participate and thrive in the evolving healthcare reform landscape?
How would you increase member engagement within the Academy and improve the value members receive for their annual dues?
While this section begins with the candidates for President-Elect, every position open is an important position and we encourage Members to read each statement and vote for the future they envision.
AAO-HNS 2014 Annual Election: Electronic Ballot
All eligible voting members of the Academy, for whom we have an active email address, will receive a personal email in advance of the ballot’s “go live” date. To assure your election-specific broadcast email arrives safely in your inbox, simply add the following email address as an approved sender: noreply@directvote.net.
This email will contain your confidential password to access the electronic ballot. For those eligible members for whom we do not have an email address on record, you will receive a letter in the mail with your personal confidential password. Members who wish to receive a paper ballot must submit a request in writing to ExecutiveOperations@entnet.org or call the Academy at 1-703-836-4444 and request to speak to someone in Executive Operations. The AAO-HNS election ballot goes “live” Monday, July 7, and closes at midnight Thursday, August 21. From the AAO-HNS Medical Devices and Drugs Committee
Committee Chair and Series Editor: Anand K. Devaiah, MD,
Boston University School of Medicine and Boston Medical Center
Jennifer Long, MD, PhD
UCLA David Geffen School of Medicine and Greater Los Angeles VA Medical Center
Otolaryngologists have a number of tools in development that may revolutionize how we practice medicine. Cell and tissue engineering is one of these exciting scientific frontiers deserving special attention by otolaryngologists. The therapeutic potential of isolated cells is a subject of intense investigation, with basic science and translational studies underway in all areas of otolaryngology. Conditions as diverse as hearing loss, vocal fold scar, the aging face, peripheral nerve injury, chronic rhinosinusitis, microtia, cleft palate, and head and neck neoplasms could benefit from cell-based therapies. Concepts for treatment include replacing injured or dysfunctional tissues, delivering a drug or therapeutic molecule directly to the site of interest, and modifying the immune or wound response to attack cancer cells or prevent adverse sequelae from injuries or surgery.
We are learning more almost daily about an ever-expanding array of cell-based therapies, their behaviors in culture dishes and in animals, and new methods to generate or analyze them. With so many studies earning attention, otolaryngologists may be left wondering how to employ these emerging treatments for their patients. In reality, of the thousands of proposed ideas, far fewer are currently vetted enough for clinical trials. Thorough animal study and subsequent regulatory review is required to ensure safety and efficacy before advancing to human use, as discussed here.
Cell-based therapies, defined as the introduction of cells to humans after some isolation or manipulation ex vivo, are regulated by the FDA. Like traditional pharmaceuticals, they require submission of extensive pre-clinical data in an Investigational New Drug Application, or IND, prior to any human application or clinical trial. However, the standard pre-clinical testing paradigm that has been used for decades in pharmaceutical research (centered on dose response, metabolic kinetics, and toxicities) is often inapplicable to these complex “biological therapeutics.” As such, the FDA has issued special guidance to industry, investigators, and users of cell-based technologies when preparing for clinical trials.
The FDA’s Center for Biologics Evaluation and Research (CBER), Office of Cellular, Tissue, and Gene Therapies (OCTGT), published a guidance statement in November 2013 to assist in design and implementation of pre-clinical trials of biological therapies in preparation for IND application.1 The rapid evolution of biological therapies poses challenges from a regulatory standpoint. Each IND is therefore considered in a case-by-case manner, allowing for a more individualized approach than in traditional drug and device applications. Nonetheless, the CBER has identified key objectives for pre-clinical study for new “biological products.”
These include:
Establishing biological plausibility, feasibility, and safety, including of the route of administration
Defining patient selection criteria, starting dose and administration schedule, and outcome and monitoring parameters
Identifying any public health risk to healthcare workers or patient contacts
The guidelines urge investigators to address these points in animal trials submitted for IND application. Additionally, the pre-clinical study model (animal species and disease model) should be relevant to humans, and the pre-clinical product should be as similar as possible to the intended human product.
CBER also issued a draft guidance statement of design considerations for early phase clinical trials, in July 2013.2 In particular, risk-benefit analysis for study participants is stressed, in light of study-related deaths and tumors that occurred in early gene and cell therapy trials. Some level of risk is inherent in studies of new therapies, especially where prior experience in humans is still limited. CBER has acknowledged the need to balance individual risk to study volunteers with potential benefits to the individual and to the greater community. This ethical issue should be considered with each new therapy and trial, including single-patient “emergency” or “compassionate use” applications that do not proceed through standard clinical trial mechanisms.
Despite the scientific complexity and uncertainty about long-term risks after implantation, cell-based therapies are now being performed in humans. Trachea tissue has become an unlikely golden child in the tissue-engineering arena, thanks to multiple implantations worldwide. The first recipient of a tissue-engineered organ recently reached five years of survival with her cell-populated bronchus replacement.3 The knowledge gained from these few initial patients is invaluable for promoting the concept of cell-based therapies. Their success should support more widespread introduction of pioneering technologies into carefully planned clinical trials.
References
1. Guidance for Industry: Preclinical Assessment of Investigational Cellular and Gene Therapy Products. November 2013. http://www.fda.gov/BiologicsBloodVaccines/GuidanceComplianceRegulatoryInformation/Guidances/CellularandGeneTherapy/UCM376136.htm
2. Draft Guidance for Industry: Considerations for the Design of Early-Phase Clinical Trials of Cellular and Gene Therapy Products. July 2013. http://www.fda.gov/downloads/BiologicsBloodVaccines/GuidanceComplianceRegulatoryInformation/Guidances/CellularandGeneTherapy/UCM359073.pdf
3. Gonfiotti A, Jaus MO, Barale D, et al. The first tissue-engineered airway transplantation: 5-year follow-up results. The Lancet 2014;383(9913):238-244.
Disclosures: Dr. Long is currently an investigator in a clinical trial of a cell-based therapy. The industry sponsor, Fibrocell Technologies, supplies the processed cells. Dr. Long does not receive any compensation or research funds from the sponsor, and holds no financial interest in the company.
This is another in a series of articles being produced by the Medical Devices and Drugs Committee, written by committee members, consultants, and invited guests for the AAO-HNS member. Do you have a question or topic we can address that may fall under the committee’s charge? Do you have a comment about an article? Please let us know! Email our coordinator, Harrison Peery, at hpeery@entnet.org and the chair, Anand Devaiah, MD, at anand.devaiah@bmc.org, with the subject line “MDDC question/article,” so we can properly identify and answer your query. We strive to quickly answer our “fan mail.” Please note that we will ask your permission to publish your note, in anonymous or edited form, if it becomes the inspiration for a Bulletin article. The 2014 AAO-HNSF Annual Meeting & OTO EXPOSM is more than just an opportunity to earn Continuing Education credit. It’s the ideal place to find out what’s hot in otolaryngology. The conference affords you the opportunity to learn from the experts, meet interesting people, make contacts for the future, and, in general, interact with colleagues from around the world.
Complementing the more than 400 hours of relevant and compelling education sessions are AAO-HNS/F membership activities, evening receptions, and forums designed to enrich your conference experience. Here’s a glimpse of some of the signature events you’ll benefit from while attending the conference.
AAO-HNSF Member and First Time Attendee Orientation
5:30-6:30 pm, Saturday, September 20
This session will give you insights on how to maximize your membership with AAO-HNS by taking advantage of all member benefits and opportunities. The orientation will also focus on getting the most out the Annual Meeting to maximize your experience. Come to this session to learn about the value of the AAO-HNS, meet key leaders, and ask questions of our knowledgeable staff.
Career Fair
5:30-7:30 pm, Monday, September 22
The AAO-HNS Career Fair, hosted by HEALTHeCAREERS Network. This event will take place at the Hyatt Regency Orlando. The AAO-HNS Career Fair provides opportunities for candidates in all specialties and levels of training to speak face to face with hiring representatives. Employers can leverage this opportunity to personally engage with numerous qualified job seekers at one time.
Alumni Receptions
6:30-8:00 pm, Tuesday, September 23
Visit with your friends from your medical school days and colleagues from other institutions while enjoying a lavish selection of delicious appetizers and treats, and local entertainment. Check our website frequently at www.entnet.org/annual_meeting to see the latest list of alumni receptions.
Board of Governors (BOG) General Assembly
5:00-7:00 pm, Monday, September 22
The BOG is the grassroots member network of the AAO-HNS and is made up of local, state, regional, and national otolaryngology societies from across the U.S. and Canada. Members of the BOG are primarily community practitioners, but all members are invited and encouraged to attend this event.
CORE Research Awards Ceremony
10:30-11:50 am, Tuesday, September 23
Join us to acknowledge this year’s CORE grantees. The AAO-HNSF, specialty societies, and industry sponsors will celebrate those individuals who have developed meritorious research projects and been awarded funding through the Centralized Otolaryngology Research Efforts (CORE) grant program in 2014.
Humanitarian Efforts
Committee Forum
1:30-3:30 pm, Sunday, September 21
At this popular forum, the recipients of the Distinguished Award for Humanitarian Service and the Arnold P. Gold, MD Foundation for Humanism in Medicine share their overseas mission experiences. Other Academy members, residents, and fellows-in-training who recently returned from missions themselves are also invited to contribute to the discussion. This is a great networking opportunity for anyone planning a medical mission.
International Assembly
3:00-5:00 pm, Tuesday, September 23
International attendees are invited to the International Assembly, a forum for recognizing guest country delegates for making awards to the International Visiting Scholars, and for leaders of International Corresponding Societies to discuss issues. Eugene N. Myers, MD, will moderate a conversation with Eben L. Rosenthal, MD, the Scientific Program Coordinator. You will also hear caucus reports from Africa, Europe, the Middle East, Latin America, and the Pacific Rim. No reservations needed!
International Reception
(invitation only)
8:00-10:00 pm, Tuesday, September 23
All registered international attendees and their spouses are invited to this reception where AAO-HNSF President Richard W. Waguespack, MD, will honor the delegates from our guest countries—Dominican Republic, Ecuador, Saudi Arabia, and the United Kingdom. Celebrate with a DJ, dancing, and enjoying delicious hors d’oeuvres. We encourage our international colleagues to wear their national dress or a lapel pin with their country’s flag or society emblem.
Otolaryngology Historical Society Meeting
6:30 pm – 8:30 pm, Monday, September 22
Join fans of the history of our specialty at the Annual Meeting reception for an evening of papers and networking. Tickets can be purchased when you register.
Poster Presentation Breakfast
7:00-8:00 am, Tuesday, September 23
Learn about the latest advancements in research directly from the sources. Ask questions and share experiences with poster presenters for a truly interactive session.
President’s Reception
6:00-7:30 pm, Sunday, September 21
Held in the OTO EXPOSM, the President’s Reception is open to all Annual Meeting & OTO EXPOSM attendees, including registered guests. One of our most popular events, this reception honors the outgoing President and provide an opportunity for you to explore the Exhibit Hall.
Section for Residents and Fellows-in-Training (SRF) General Assembly
2:30 pm-4:30 pm Monday, September 22
Join other medical students, residents, and fellows-in-training to discuss topics important to you at this stage in your career. The General Assembly will feature presentations from AAO-HNS leaders, a keynote speaker, section elections, an update of the annual SRF survey, and presentation of awards. As a medical student, resident, and/or fellow-in-training, this is an ideal venue to meet colleagues, have a voice, and get involved in AAO-HNS initiatives and activities.
Women in Otolaryngology (WIO) Section Luncheon
Noon-2:55 pm Monday, September 22
This year the WIO Section’s keynote speaker is Susan Miller, PhD, Voice and Communications Consultant, Washington, DC. Her presentation is titled, “Presenting Your Best Self.” The session is geared to encourage participants to engage in fun, interactive exercises to teach the important aspects of communication (our voice and body language) in a practical format.
Women in Otolaryngology (WIO) Section General Assembly
1:00-2:00 pm Monday, September 22
The WIO Section exists to enhance the careers of women otolaryngologists. Join WIO members and supporters for presentations from AAO-HNS leaders, a keynote speaker, section elections, and presentation of awards. 
Lee D. Eisenberg, MD, MPH
My connection to the Academy has spanned many years and it began immediately after my otolaryngology training at the University of California, San Francisco, in 1977. While I was a resident, our chairman, Roger L. Boles, MD, always stressed the importance of being involved. At his recommendation, I was appointed to the Committee of Terminology, the predecessor of the CPT committee, for the Academy. What I didn’t realize was, as I got closer to the inner workings of programs and resources, my philanthropic commitment would also grow.
During the early years of my professional career, I gravitated to committees focusing on ensuring members had access to the body of knowledge necessary to understand the business side of medical practice. I also developed an interest in quality of care by our specialty to better serve our patients. I served on committees addressing primary care referral and patient management guidelines and was a member of the Instruction Course Advisory Committee and the Home Study Course faculty.
How did these early experiences inspire my philanthropy? What impressed me as a committee and Board member was the commitment of resources that the Academy dedicates to creating, continually assessing, and delivering educational programs and products for the members to keep them informed of the advances in the practice of otolaryngology-head and neck surgery. The Home Study Course is an outstanding example of a tool appreciated and used by many Academy members that has had lasting value and adapted over time. It has a dollar value of many hundreds of dollars—and, therefore, provides great value for the membership dollar. I learned that as important as membership dues and Annual Meeting revenues are to providing operational support, these two revenue streams do not cover the costs of what is dedicated to the area of education. What covers the difference? Charitable support helps to fill the gap.
The AAO-HNS is our representative in the socioeconomic arena. I have been fortunate to be involved in this area as well for many years as a BOG member, coordinator for Practice Affairs, member of the CPT Editorial Panel, Physician Payment Policy (3P) Workgroup, Surgical Quality Alliance member, and consultant to the Patient Safety Quality Improvement Committee. All of these areas require significant Academy resources, both personnel and financial.
Throughout the years, I have done the math to calculate the costs entailed to ensure these meetings continue to take place. The Academy pays all the expenses incurred for sending volunteers like me and staff to be present at these critical meetings. Where would we all be if these conversations were not happening with the right people at the right time? Again, thanks to the supplemental support that comes from charitable donations, this vital effort continues.
Looking at the future of the Academy, our ability to be a body of influence relies on being relevant to the physicians who are choosing our specialty. For many members, the Foundation provides research grant funding that could not be acquired elsewhere. We all understand the challenging environment that exists for obtaining such funding. We can appreciate the value of this support to those beginning their careers in the specialty. Equally important are the travel grants awarded to enable residents to connect to the Academy during the Annual Meeting and the Leadership Forum. The Board members and committee chairs of today were those who, like me, got engaged right at the start. Charitable support to these areas is an investment in our specialty and ourselves.
As we know, the Academy sells its educational products, charges registration fees for the annual meeting and, of course, collects annual membership dues. These revenue sources alone are insufficient to enable us to accomplish all that is necessary to serve the needs of our members. The appreciation for all that the Academy provides, as well as the commitment of member volunteers to pursue the best for patient care in the specialty has inspired my philanthropy. Many members support the Millennium Society and are Hal Foster, MD Endowment donors. With the support of additional members, we can accomplish even more. So, please join me and the many members of the Academy who are already supporting our mission. Take a moment and visit www.entnet.org/donate. Peruse the many different ways you can support the Academy. It’s easy to support the AAO-HNS/F in a way that is meaningful to you. For questions, please contact Ron Sallerson, senior director of development, at rsallerson@entnet.org or 703-535-3775. Thank you in advance for your support. 
By Gavin Setzen, MD
Secretary-Treasurer
Budgeting for FY15 represents the collaborative work of both the staff leadership and the members of the Finance and Investment Subcommittee (FISC) to develop a proposed combined AAO-HNS/F budget for the next fiscal year, July 1, 2014, through June 30, 2015. The debt covenant requirement for a balanced budget continues to be a challenge; however, the AAO-HNS/F continues to work to support its members in the most effective and efficient way possible.
The budget presented reflects the continuing effort to streamline processes and focus resources to support the strategic plan for the upcoming year. While strategic planning is an ongoing process, this year reflects a significant change from prior years. The official Strategic Plan is now aligned with AAO-HNS/F’s fiscal year and in sync with the annual budget planning. As a result, the FY15 budget takes into account the strategic priorities identified by the Boards of Directors (BODs), including critical new activities and a challenge to implement new net revenue producing activities, reduce operating expenses, and restructure/eliminate low impact programs in order to free up resources to concentrate on high-impact and new program areas.
In early spring, the FISC reviewed financial results for the first six months of the FY14 budget year and we were pleased to see that AAO-HNS/F was projecting a favorable variance, as compared to budget, for the year. The 2013 Annual Meeting & OTO EXPOSM once again netted favorable results and staff continues to identify cost savings. This was all done under the leadership of David R. Nielsen, MD.
The budget planning process involved each of the business units of AAO-HNS/F submitting their budget to the financial team that worked with them to assure that the revenue and expenses were in line with the mission and priorities of AAO-HNS/F. The financial team is composed of Brenda S. Hargett, chief operating and financial officer (COO); Lynn Frischkorn, director of Budgeting and Special Projects; and Carrie Hanlon, senior director of Financial Operations. The financial team presented the proposed budget to the FISC for an initial review in early March and then a final proposed budget in late March. Once reviewed and approved by FISC, the proposed FY15 budget was presented to the Executive Committees (ECs) of the BODs recommending their endorsement for approval by the BODs. The ECs endorsed the FY15 proposed budget during their April meeting. Also in April, the BODs reviewed and conditionally approved the FY15 budget that is presented here for our membership. Kanwar S. Kelley, MD, JD
Chair, Section for Residents
and Fellow in Training
Resident, U.C. Irvine
In early March, residents and fellows-in-training from around the country had the opportunity to attend the Academy Leadership Forum in Alexandria, VA. In spite of a winter storm, snarled travel plans, and the annual in-service exam the day before the forum—a record number of residents and fellows (29) were able to attend thanks to the incredible generosity of the Academy and donors who supported Resident Leadership Grants. A total of 103 members were present.
As part of the BOG and Academy’s dedication to outreach for residents and young physicians, content was tailored to the specific needs of our group. Panels on practice management, hospital and employee contract negotiation, legislative and political advocacy, and health policy all ensured an enriching experience. The forum guest speaker Rep. Andy Harris, MD, (B.-MD) of the U.S. House of Representatives highlighted the presentations, and networking events between residents and Academy leaders were dedicated to the training and development of young physicians.
One of the Section for Residents and Fellows-in-Training’s (SRF) top priorities this year has been to increase resident and fellow involvement in advocacy related efforts. In coordination with the ENT PAC the AAO-HNS political action committee, the SRF campaign has had a great start. It was my absolute pleasure to announce at the forum that U.C. Irvine was able to achieve 100 percent resident participation in 2013. Other programs made great progress as well. With an election year in full swing, every resident and fellow is encouraged to become a donor to ENT PAC no matter how small the dollar amount.
The Leadership Forum provided incredible insight about health policy, advocacy efforts, and leadership development. We recommend every resident or fellow take part in during the course of their training. I hope to see everyone in Orlando, Monday, September 22, during the SRF General Assembly and in Alexandria next March.
If you know a resident or fellow doing exceptional work inside or outside of his/her program, nominate her/him now for our quarterly resident and fellow spotlight. Email your nomination to SRF@entnet.org and we will contact you.
*Contributions to ENT PAC are not deductible as charitable contributions for federal income tax purposes. Contributions are voluntary, and all members of the American Academy of Otolaryngology-Head and Neck Surgery have the right to refuse to contribute without reprisal. Federal law prohibits ENT PAC from accepting contributions from foreign nationals. By law, if your contributions are made using a personal check or credit card, ENT PAC may use your contribution only to support candidates in federal elections. All corporate contributions to ENT PAC will be used for educational and administrative fees of ENT PAC, and other activities permissible under federal law. Federal law requires ENT PAC to use its best efforts to collect and report the name, mailing address, occupation, and the name of the employer of individuals whose contributions exceed $200 in a calendar year.
2014 AAO-HNS Leadership Forum a Great Success!
Otolaryngologists from around the country convened in Alexandria, VA, March 2-3, to participate in a successful inaugural AAO-HNS Leadership Forum. Despite a city-stalling snowstorm, a warm and exciting exchange of information and friendships took place. The clear message: our voice is heard amongst the AAO-HNS leadership. The Board of Governors (BOG) is an integral participant in the Academy’s Executive Committee, with our chair a voting member, and our chair-elect a standing guest. Along with the immediate past chair of the BOG both are voting members of the Board of Directors (BOD). In addition, the BOG has formal representation to the 3P (Physician Payment Policy) Workgroup. All of these venues allow the BOG to communicate important information to and from you, the membership, and the Academy. The focus of this year’s Leadership Forum was on Advocacy, Research and Quality, Education and Knowledge, Sustainability, and Membership Strength and Unity.
See the whole story online at www.entnet.org when you Login as a Member. 
The 2014 AAO-HNS Leadership Forum which took place March 2-3 in Alexandria, VA, was a rousing success bringing AAO-HNS, BOD, and BOG members (including a significant number of otolaryngology residents) together to discuss a wide variety of topics including the transitioning to ICD-10 coding. Robert R. Lorenz, MD, gave an informative talk on where our practices should be in the ICD-10 transition process as we approached the scheduled October 1, 2014 deadline. Shortly after that meeting the U.S. House of Representatives changed that schedule when it quickly passed by voice vote bill HR 4302, “Protecting Access to Medicare Act 2014.” This bill, which was also passed by the Senate and signed by the President, delayed the onset of the ICD-10 changes by a minimum of one year, now starting no earlier than October 1, 2015. On its face this legislation could have appeared to be a win for many of our independent practice colleagues who may not have been on schedule for the October 1, 2014 deadline. However, this postponement of the ICD-10 implementation could also be viewed as a wolf in sheep’s clothing due to the Sustainable Growth Rate (SGR) patch that was once again used to delay a permanent fix to this broken system of adjusting Medicare payments.
The AAO-HNS has been committed to supporting legislation to repeal the SGR for the last several years. They have worked to educate Congress regarding the instability of the Medicare payment system. They have repeatedly outlined to Congress that this instability in the Medicare payment system is threatening our patients’ access to healthcare by making it difficult for our members to make plans for the future of their practices, to invest in their practices, to provide for their employees and to make investments to help improve the quality and efficiency of the care they provide. The quick passage of yet another SGR patch ignores significant cooperative efforts and sacrifices offered by the House of Medicine over the past year to permanently fix the SGR. The cost of fixing the SGR had never been as affordable as it was this past year yet all these efforts were brushed aside and the SGR can was once again kicked down the road. The short-term gain of an ICD-10 delay seems to have sugar-coated this otherwise bitter political pill.
Delay in the implementation of the ICD-10 system has in its own right caused some concerns for many institutions who were “on track” for the October 1, 2014 implementation date. Many institutions have spent millions of dollars and significant time and effort in preparing for the implementation. The delay in the timeline so close to the start date means that the delay occurs just as the testing of the modified systems was set to begin. Testing typically occurs in the last six months checking how the system will work with third party payers. There are significant resources put into the education of the providers and staff as well. Many organizations have contracts with outside consultants hired to educate the providers. These contracts may need to be amended or extended to avoid a large gap between the time of education and the time of implementation of the new paradigms. Some institutions may have to maintain both the ICD-9 and ICD-10 systems in parallel until the change is made permanently. This can significantly alter an institution’s project management perspectives. Another issue is that the change in implementation date is not yet fixed as the legislation reads “not before” Octobert 1, 2015 which means this could be delayed yet again. Since the decision was taken out of the hands of CMS (which had vowed not to delay ICD-10 implementation ever again) we are left with Congress once again holding hostage our ability to plan for the future of our practices.
The brave new world of healthcare reform continues to show us an ever-changing and therefore unpredictable landscape. We must continually educate our colleagues and our representatives as to the ultimate impact of many of the decisions made in our state houses and in Washington. We should never lose sight of the forest for the trees!
References
AAO-HNS Overview: Federal Legislative Priorities. Government Affairs, www.entnet.org/advocacy.
Carr, David. ICD-10 Delay Creates Headaches. Information Week Healthcare 4/3/14. 
As time passes, I become more used to the ebb and flow of Academy timelines. June marks the end of the school year and the beginning of summer for our youth. It also means the introduction of our candidates for Academy leadership positions, and reminds me of the incredible legacy each Academy member leaves as he or she participates in strengthening our specialty.
Please take time to get to know the candidates for Academy offices and carefully review their statements, backgrounds of service, and their perspectives on the future of the specialty. Each year, the Nominating Committee does a remarkable job of poring over dozens of names, evaluating their merits in light of the strategic direction of the AAO-HNS/F, and matching the best people they can with critical positions of leadership. I express my heartfelt thanks to James L. Netterville, MD, Nominating Committee Chair, and these thoughtful and hardworking Academy volunteers who take this assignment seriously and put in a tremendous amount of work to ensure our leaders are chosen from truly outstanding candidates. I also want to offer my thanks to those who were so highly respected that their names were solicited and who agreed to be considered, but may not have been nominated at this time. Out of thousands of Academy members, it is a great honor from your colleagues to be asked if you would allow your name to be considered for nomination. I am certain, and history bears this out, that those who were considered, but not nominated this year, will have future leadership opportunities.
Author and leadership consultant Holly Duckworth of Leadership Consultants International recently presented a stimulating session at the 2014 Great Ideas Conference of the American Society of Association Executives (ASAE) on inspiring action in associations and their leaders. Using the model of “rebooting” our computers to upgrade or improve function, she advises that we “control/alt/delete,” or reboot, in our leadership lives, too.
Leaders often face the challenges, doubts, and fears of constrained resources matched against unlimited demands. Successful leaders learn to control their doubts and fears; alternatively replacing them with courage, faith, and abundance. Deleting the inertia, sacred cows, irrelevant programs, special interest resource sinks, and outdated policies of the past is essential before we can replace them with the changes that will increase our relevance, value, and meaning to our members.
As leaders, we have to ask ourselves, to what degree are we taking control of, or owning our responsibility to influence, our attitudes and biases and those for whom we have stewardship? Do we bring to the table an attitude of abundance or of scarcity? Do we recognize every challenge as an opportunity, or just a barrier to getting what we want? (To see the slides from Ms. Duckworth’s presentation, visit http://www.slideshare.net/hollyduckworth/140121-isae-ctrlaltbelieve.) In suggesting solutions, she counsels us to replace the word “delete” with “believe.” Look for her book, Control, Alt, Believe, in the fall.
In December 1996, author John Brockman began an online community with about 50 people known as “Edge—The World Question Center.” Its purpose? To arrive at the edge of the world’s knowledge, seek out the most complex and sophisticated minds, put them in a room together, and have them ask each other the questions they are asking themselves. It’s now grown to millions of individual users. For its 10-year anniversary, the 2007 Edge Annual Question was “What are you optimistic about?”
What a great question! How would you respond? I’m optimistic about the future of our specialty. I’m optimistic about advancing technology and improving the lives and health of our patients. I’m optimistic about our residents and the next generation of otolaryngologists. I’m optimistic about our future leaders—and the slate of candidates for office. I’m optimistic about the professional skill, creativity, and problem solving ability of our wonderful staff. I’m incredibly optimistic about the loyalty, volunteerism, and contributions of our membership. Few associations have members who truly “own” their organization the way we do. As members, we own by engagement and participation, not just simply by fiscal standards.
This summer, I hope every Academy member will take time to evaluate the leaders who will provide direction and guidance for the coming years. Vote, engage, share your perspective. Let our leaders know what you expect and how you are willing to work with them to achieve the vision of a brighter future as we work together to empower doctors to provide the best ear, nose, and throat care. 
This issue premiers the official statements of the candidates for Leadership 2014. Having had this same task as a potential candidate, I remember the thought and preparation required. It is not an easy assignment even when one has been deeply involved in the complexity of the socioeconomic needs of our specialty over many years. The opportunity to lead is exciting and daunting in equal shares.
Like many of you, I had opinions about our organizations’ greatest strengths, weaknesses, opportunities, and vulnerabilities. I further researched the available data and concluded that our strategic planning process and the caliber of Academy/Foundation leadership were our greatest strengths. I saw, too, the immensity of the one challenge that gave me the most concern, “the relentless trend of decreasing reimbursement and increasing expenses and administrative burdens.” And as I saw the looming reach of the Affordable Care Act, I was troubled by the “additional mandates to employ EMRs, utilize electronic prescribing, and implement ICD-10 diagnostic coding.” I said then that I believed it was the Academy’s role to provide members with as many tools as possible to deal with these coming changes and to mitigate negative impacts when possible. See more at: http://bulletin.entnet.org/article/official-statements-of-leadership-candidates-3/. Indeed, this has been the challenge that we continue to address as you can see in almost every Bulletin and weekly e-mail of AAO-HNS The News.
But, what really has been my professional experience of leadership, and what can I share with you about how you as a Member can influence your leaders when your appointment book is full?
Influencing Your Leaders for Better Outcomes
While the step-by-step role of leadership in working on such challenges initially looked definable to me, I have been somewhat surprised by what has turned out to be the biggest responsibility and benefit of leadership. Let me rely here on an expert to explain. Jim Yong Kim, MD, current leader of the World Bank, spoke recently with Lillian Cunningham, of The Washington Post, about facing challenges on the occasion of its first reorganization in 20 years and his accompanying pledge to save $400 million in administrative costs. Dr. Kim simply expressed this opportunity:
“One of the most important things about leadership is that you have to have the kind of humility that will allow you to be coached. . . . No matter how good you think you are as a leader, my goodness, the people around you will have all kinds of ideas for how you can get better. So for me, the most fundamental thing about leadership is to have the humility to continue to get feedback and to try to get better — because your job is to try to help everybody else get better.” (http://www.washingtonpost.com/blogs/on-leadership/wp/2014/04/10/trying-to-change-the-world-bank)
So, I know well that your patients and your practices are your first priority as they should be and that you are often pulled in myriad directions for what small time you can reserve for other responsibilities and interests. My message here is that you can give more than you know when you communicate with your leaders about how they are addressing your needs, your concerns, your solutions, your challenges. This is the time of year when you can influence the AAO-HNS/F most—with your vote.
Ensuring the future
My partner, our colleague, our AAO-HNS/F trusted representative for 12 years, David R. Nielsen, MD, will conclude his tenure as Executive Vice President and CEO in January 2015. David has acted often as my coach in big and small ways over my term as your President. I have had total confidence in his ability to stand in for the voice of the specialty within the greater world of medicine, and regulatory bodies. While epitomizing the humility that Dr. Kim sees in great leadership, Dr. Nielsen has maintained that necessary passion for open direct dialog with members and others that forwards both his and the specialty’s growth and change–the most nourishing elements for a sustainable future.
With your continuing feedback to leaders like Dr. Nielsen, take this moment to further ensure our continued organizational success following David’s actions. Give back to the specialty though the David R. Nielsen, MD Endowment. This gift directly influences our future as the funds will be applied where needed most. Don’t let this opportunity go to extend your influence today, more at www.entnet.org/donate.