Vanderbilt Mission to Malindi, Kenya
Brannon Mangus, MD Humanitarian Travel Grant Awardee Otolaryngology, Head and Neck Surgery; Vanderbilt UniversityFor 12 days in November 2010, a team from Vanderbilt University led by James L. Netterville, MD, and Robert J. Sinard, MD, worked at two hospitals in Malindi, on the coast of Kenya. This trip to Malindi, Kenya, was an experience I will take with me the rest of my life. I have been on mission trips before, but this was my first medical mission trip. For anyone considering a medical mission trip, I highly recommend going on one that is as organized as this one. Because of the impeccable planning and efficiency, we were able to focus on patient care while we were there. The host organization, the Caris Foundation, arranged our transportation, food, and lodging, allowing us to focus on patient care. We were there for 12 days. Our group was divided into two groups: one group of surgeons, anesthesiologists, and nurses worked at Tawfiq Hospital (the Muslim hospital) and another group worked at Malindi District Hospital (the Christian hospital). This allowed us to maximize the number of patients that we could treat. Each day began with seeing patients that the local doctors had “saved up” for us. Most of these patients were instructed to be NPO so that they could undergo surgery that day. There was a great variety of cases including thyroid masses, neck masses, parotid tumors, cleft lips and palates, mandibular tumors, scar revisions, chronic sinusitis, tonsillitis, OSA, chronic ear disease, and frontal sinus fractures. We completed 125 procedures. The number of cases we could care for in such short time and at such relatively low cost made the greatest impression on me. Many of the supplies that we used would have been discarded as waste in the U.S. With little to no red tape, we were able to maximize patient care. Unfortunately, the hospital conditions that the patients had to endure postoperatively were less than ideal. Many patients had to share a bed with another patient—most patients in the U.S. would call patient affairs if they had to share a semi-private room. These patients shared a bed with another patient in a large room with 50 other patients. To learn more about humanitarian travel grants, visit http://www.entnet.org/Community/public/Residents-and-Fellows.cfm or contact humanitarian@entnet.org.
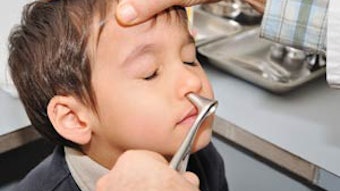
 Dr. Mangus examines a child with a cleft lip while rounding with Dr. Netterville and Dr. Sinard.
Dr. Mangus examines a child with a cleft lip while rounding with Dr. Netterville and Dr. Sinard.Brannon Mangus, MD
Humanitarian Travel Grant Awardee
Otolaryngology, Head and Neck Surgery; Vanderbilt UniversityFor 12 days in November 2010, a team from Vanderbilt University led by James L. Netterville, MD, and Robert J. Sinard, MD, worked at two hospitals in Malindi, on the coast of Kenya. This trip to Malindi, Kenya, was an experience I will take with me the rest of my life.
I have been on mission trips before, but this was my first medical mission trip. For anyone considering a medical mission trip, I highly recommend going on one that is as organized as this one. Because of the impeccable planning and efficiency, we were able to focus on patient care while we were there. The host organization, the Caris Foundation, arranged our transportation, food, and lodging, allowing us to focus on patient care.
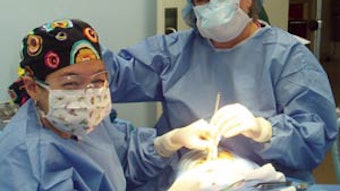
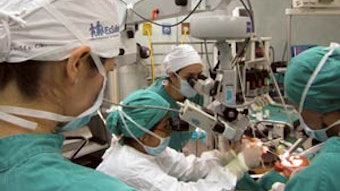
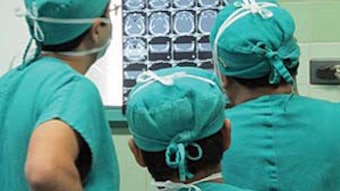
We were there for 12 days. Our group was divided into two groups: one group of surgeons, anesthesiologists, and nurses worked at Tawfiq Hospital (the Muslim hospital) and another group worked at Malindi District Hospital (the Christian hospital). This allowed us to maximize the number of patients that we could treat. Each day began with seeing patients that the local doctors had “saved up” for us. Most of these patients were instructed to be NPO so that they could undergo surgery that day. There was a great variety of cases including thyroid masses, neck masses, parotid tumors, cleft lips and palates, mandibular tumors, scar revisions, chronic sinusitis, tonsillitis, OSA, chronic ear disease, and frontal sinus fractures. We completed 125 procedures.
The number of cases we could care for in such short time and at such relatively low cost made the greatest impression on me. Many of the supplies that we used would have been discarded as waste in the U.S. With little to no red tape, we were able to maximize patient care. Unfortunately, the hospital conditions that the patients had to endure postoperatively were less than ideal. Many patients had to share a bed with another patient—most patients in the U.S. would call patient affairs if they had to share a semi-private room. These patients shared a bed with another patient in a large room with 50 other patients.
To learn more about humanitarian travel grants, visit http://www.entnet.org/Community/public/Residents-and-Fellows.cfm or contact humanitarian@entnet.org.