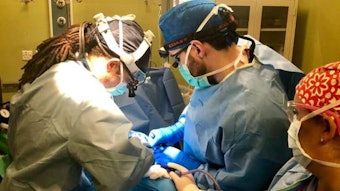
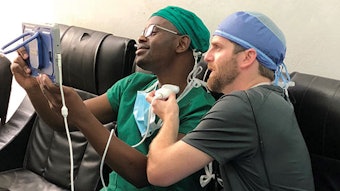
Team helps 493 patients in Migori, Kenya
This past October, a team of two otolaryngologists, a general surgeon, and an orthopedic surgeon descended upon Migori in Southwestern Kenya to provide a week of surgical care for adult and pediatric patients. I was fortunate to accompany this team with the support of the American Academy of Otolaryngology–Head and Neck Surgery Foundation Humanitarian Grant program.
Travel Grant Debrief
Matthew G. Crowson, MD, FRCSC
This past October, a team of two otolaryngologists, a general surgeon, and an orthopedic surgeon descended upon Migori in Southwestern Kenya to provide a week of surgical care for adult and pediatric patients. I was fortunate to accompany this team with the support of the American Academy of Otolaryngology–Head and Neck Surgery Foundation Humanitarian Grant program. Migori is a seven-hour ride from Nairobi through the rural countryside along undeveloped roads and small villages. The closest major hospital is six hours away in Kijabe, so the clinical facility in Migori is the lone outpost and care access center for the residents of southwestern Kenya and northeastern Tanzania.
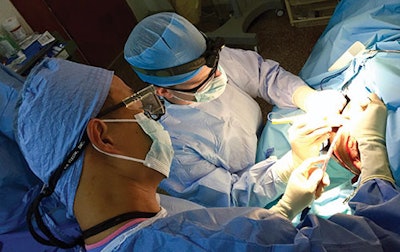
The trip was facilitated by Kenya Relief (KenyaRelief.org), an Alabama-based non-governmental organization that provides 20 short-term medical mission teams to work in various subspecialties. On site, Kenya Relief has built a hospital with two operating rooms, an observation unit, a laboratory, and a pharmacy. Their non-medical infrastructure includes a school with computer lab and an orphanage. Kenya Relief relies upon stateside donations in order to support American missionaries who lead the efforts, as well as the local teaching, medical clinic support, and security staff.
Upon our arrival, we were greeted with personalized signs by the residents of the Kenya Relief orphanage. The missionaries at Kenya Relief told us that the children and village residents are always appreciative when care teams come—reliable, consistent, basic healthcare is extremely limited in rural Southwestern Kenya. After getting settled, we were quickly oriented to the clinical infrastructure of the Kenya Relief clinic. When a medical team is on the way, Kenya Relief relies on radio bulletins and word of mouth to spread the message that care is available. Hopeful patients will either travel by bus or foot—sometimes for days—to Migori in order to be seen. Only relatively minor procedures are performed given the limited equipment availability (e.g. tympanoplasties, basic sinonasal procedures, cutaneous and subcutaneous lesion excision, thyroid lobectomies), and a lack of post-operative care support to manage significant surgical complications should they arise. Our first day was comprised of pre-operative assessments, and we were provided one operating room for the following three days. At the end of the week, the medical team was able to help 493 adults and children, 70 of which received surgical procedures.
I am grateful for the support from the AAO-HNS to participate in the life-changing mission trip. I came away with a new appreciation for all that we have in North America, and the substantial unmet need of our brothers and sisters across the Atlantic for basic otolaryngologic care.